IBD in Pregnancy - Bumps & Bowels
- Fertility: Unaffected in inactive IBD. May be ↓ in active disease, especially with pelvic surgery (e.g., IPAA).
- Pregnancy Outcomes: Disease activity is the key predictor.
- Active IBD: ↑ risk of preterm birth (< 37 weeks), low birth weight (< 2500 g), and miscarriage.
- Inactive IBD: Outcomes are comparable to the general population.
⭐> The single most important factor for a healthy pregnancy is achieving and maintaining remission for at least 3-6 months prior to conception.
Medication Management in Pregnancy & Lactation
| Medication Class | Pregnancy/Lactation Safety |
|---|---|
| 5-ASA Agents | Generally safe; supplement with high-dose folate ($2$ mg/day). |
| Corticosteroids | Safe for flares; monitor for gestational diabetes/hypertension. |
| Thiopurines | Generally safe; benefits of maintaining remission outweigh risks. |
| Anti-TNFα | Generally safe; may consider holding in the third trimester. |
| Methotrexate | ⚠️ Contraindicated (teratogen); stop 3-6 months before conception. |
IBD in the Elderly - Golden Year Guts
- Diagnostic Challenges: Symptoms mimic other geriatric conditions like ischemic colitis, diverticulitis, and malignancy. A high index of suspicion is crucial.
- Disease Presentation:
- ↑ incidence of Ulcerative Colitis (UC), often left-sided (proctitis).
- Crohn's Disease (CD) is more commonly colonic (L2) and non-stricturing.
- Management Considerations:
- Higher risk of opportunistic infections and malignancy with immunosuppressants.
- Polypharmacy & comorbidities complicate treatment.
- Cautious use of steroids due to ↑ risk of side effects (osteoporosis, hyperglycemia).
⭐ Exam Favorite: Elderly IBD patients have a significantly higher risk of severe Clostridioides difficile infection, which is associated with increased morbidity and mortality.
Pediatric IBD - Growing Pains
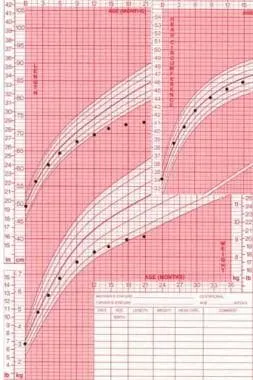
- Unique Presentation: Growth failure is a highly specific sign. Look for delayed puberty, malnutrition, weight loss, and anemia. Abdominal pain can be less prominent than in adults.
- Disease Patterns:
- Crohn's Disease (CD): Typically more extensive, often ileocolonic (L3) disease.
- Ulcerative Colitis (UC): More likely to present as pancolitis (~80% of cases), leading to a more severe initial course.
⭐ Primary Therapy: Exclusive Enteral Nutrition (EEN) is a first-line, steroid-sparing therapy to induce remission in pediatric CD, promoting mucosal healing and catch-up growth.
Post-Surgical IBD - After the Cut
-
Crohn's Disease (CD): High recurrence risk after resection.
- Risk Factors: Smoking, penetrating/fistulizing disease, prior resections.
- Surveillance: Ileocolonoscopy at 6-12 months post-op to guide therapy.
- Staging: Rutgeerts score (i2-i4) indicates need for treatment escalation (e.g., biologics).
-
Ulcerative Colitis (UC): Pouchitis after total proctocolectomy with IPAA.
- Acute Pouchitis Tx: Ciprofloxacin or Metronidazole.
- Chronic Pouchitis: Consider probiotics (e.g., VSL#3) or long-term antibiotics.
⭐ Up to 80% of Crohn's patients experience endoscopic recurrence within one year of surgery without prophylactic treatment.
High‑Yield Points - ⚡ Biggest Takeaways
- Pregnancy & IBD: Most meds are safe, except methotrexate and thalidomide. Disease control before conception is crucial for better maternal and fetal outcomes.
- Elderly Onset: Often presents atypically. Higher risk of C. difficile, malignancy, and medication side effects. Biologics require cautious use.
- Pediatric IBD: Key features include growth failure and delayed puberty. Exclusive enteral nutrition is a first-line therapy, especially in Crohn's disease.
- Post-Surgery: Proctocolectomy with IPAA is curative for ulcerative colitis. Surgery in Crohn's is for complications, not a cure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

