Pre-Conception & Risks - The Baby Blueprint
-
Goal: Achieve and maintain remission for ≥3-6 months before conception. Disease activity, not medications, is the primary driver of adverse outcomes.
-
Maternal Risks (from active disease):
- ↑ Pre-eclampsia
- ↑ Venous Thromboembolism (VTE)
- ↑ C-section rates
-
Fetal Risks (from active disease):
- ↑ Preterm birth (<37 weeks)
- ↑ Low birth weight (<2500g)
- ↑ Small for Gestational Age (SGA)
⭐ Most IBD medications are safe in pregnancy. The key exception is Methotrexate, which is teratogenic and must be discontinued 3-6 months prior to conception in both men and women.
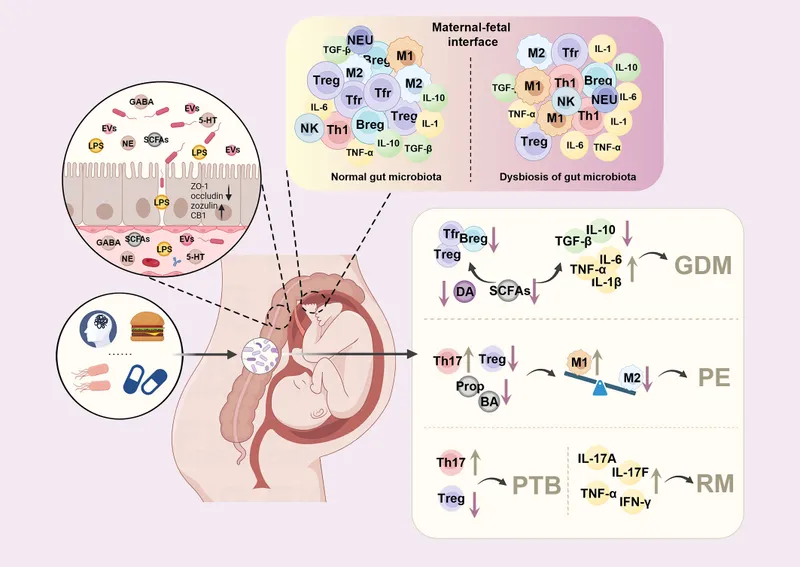
Disease Activity & Fetal Outcomes - The Great Balancing Act
- Primary Goal: Maintain remission ≥3 months pre-conception & throughout pregnancy.
- Active inflammation is the principal driver of adverse outcomes, far outweighing the risks of most IBD medications.
⭐ The greatest risk for adverse fetal outcomes (e.g., preterm birth, low birth weight, SGA) stems from active maternal IBD, not from the majority of IBD medications used for maintenance.
Pharmacotherapy - Safe Harbor Meds
Maintaining remission is crucial; the risk of active IBD outweighs the risk of most medications. Generally, the pre-conception regimen should be continued, with exceptions noted below.
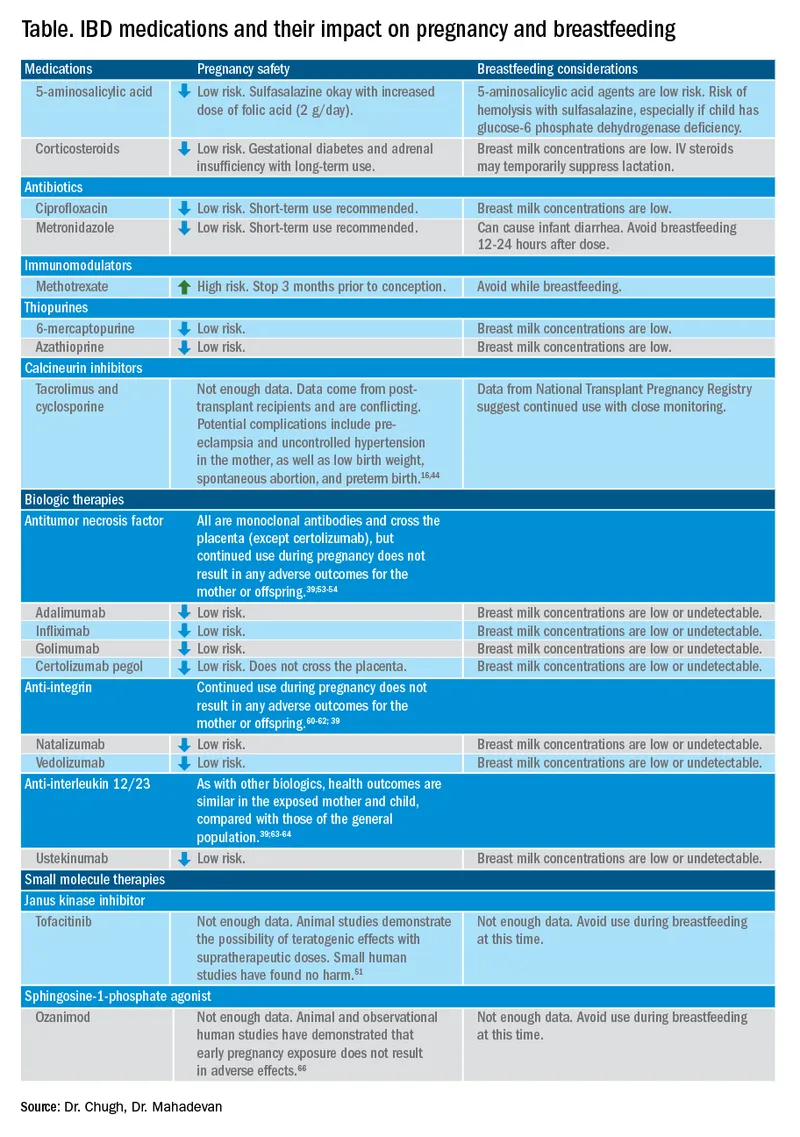
| Drug Class | Pregnancy Safety | Breastfeeding Safety |
|---|---|---|
| 5-ASA Agents | Safe. ⚠️ Supplement with folic acid ($2 mg/day$) for sulfasalazine. | Safe. |
| Corticosteroids | Use for flares; lowest effective dose. Small ↑ risk of cleft palate (1st tri). | Safe. |
| Thiopurines | Safe. Benefits of disease control outweigh theoretical risks. | Safe. |
| Anti-TNFα Agents | Safe. Can be continued through pregnancy. Consider stopping at 24-26 wks. | Safe. |
Delivery & Postpartum - The Final Push
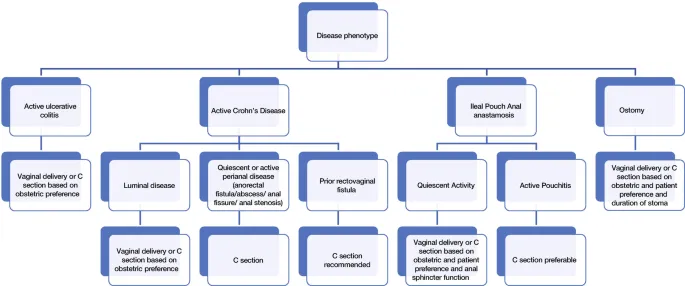
- Mode of Delivery:
- Vaginal delivery is preferred for most patients.
- C-section is indicated for active perianal disease (fistulas, abscesses) or a history of ileal pouch-anal anastomosis (IPAA) to protect sphincter function.
- Postpartum Flare Risk:
- ↑ risk of flare, especially in the first 3 months postpartum.
- Risk is highest if IBD was active at conception or during pregnancy.
- Breastfeeding & Meds:
- Encouraged; most IBD medications are compatible (e.g., 5-ASA, biologics).
- ⚠️ Contraindicated: Methotrexate, Tofacitinib.
⭐ Active perianal disease is a key indication for Cesarean section to prevent sphincter damage and worsening fistulas.
High‑Yield Points - ⚡ Biggest Takeaways
- Disease activity at conception is the strongest predictor of flares during pregnancy.
- Most IBD medications are safe, including 5-ASA, biologics (anti-TNF), and steroids.
- Methotrexate is an absolute contraindication due to teratogenicity.
- Sulfasalazine requires supplementation with high-dose folate.
- Vaginal delivery is preferred unless there is active perianal disease.
- Breastfeeding is safe with most IBD drugs; avoid methotrexate and cyclosporine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

