Pathophysiology & Genetics - A Sickle Situation
- Genetic Defect: Autosomal recessive point mutation in the β-globin gene (HBB).
- A single base substitution replaces hydrophilic glutamic acid with hydrophobic valine.
- This results in the formation of abnormal Hemoglobin S (HbS).
- Mechanism:
- Under low O₂ conditions (e.g., infection, dehydration, acidosis), HbS polymerizes into rigid, insoluble fibers.
- This deforms RBCs into a sickle shape, causing:
- Vaso-occlusion: Blockage of microvasculature → ischemic pain, organ damage.
- Hemolysis: Premature destruction (lifespan 10-20 days) → chronic anemia, jaundice.
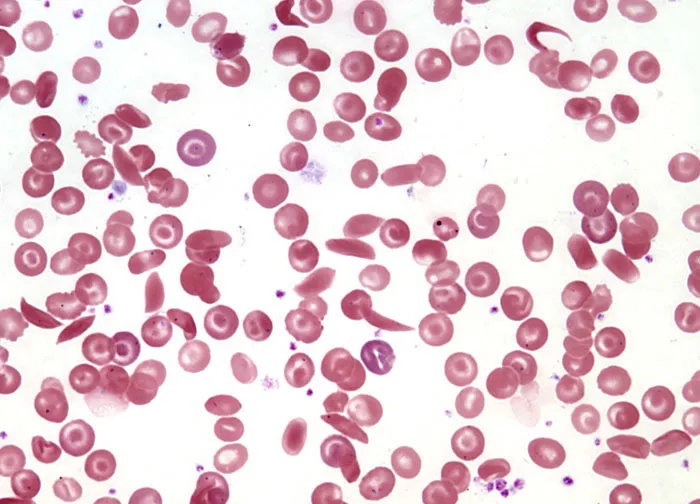
⭐ Heterozygotes (HbAS, Sickle Cell Trait) are typically asymptomatic and exhibit resistance to Plasmodium falciparum malaria.
Clinical Features & Diagnosis - Spotting the Sickle
- Vaso-Occlusive Crisis (VOC): Hallmark of SCD.
- Dactylitis: Swelling of hands/feet; often the first sign in infants.
- Acute Pain: Excruciating pain in bones, chest (Acute Chest Syndrome), abdomen.
- Stroke: High risk, even in children.
- Chronic Manifestations:
- Functional Asplenia: ↑ risk of infection from encapsulated organisms (e.g., S. pneumoniae).
- Avascular necrosis (hip, shoulder), leg ulcers, priapism.
- Diagnosis:
- Screening: Newborn screening is standard.
- Labs: Normocytic anemia, ↑ reticulocytes.
- Confirmatory: Hb electrophoresis shows predominantly HbS.
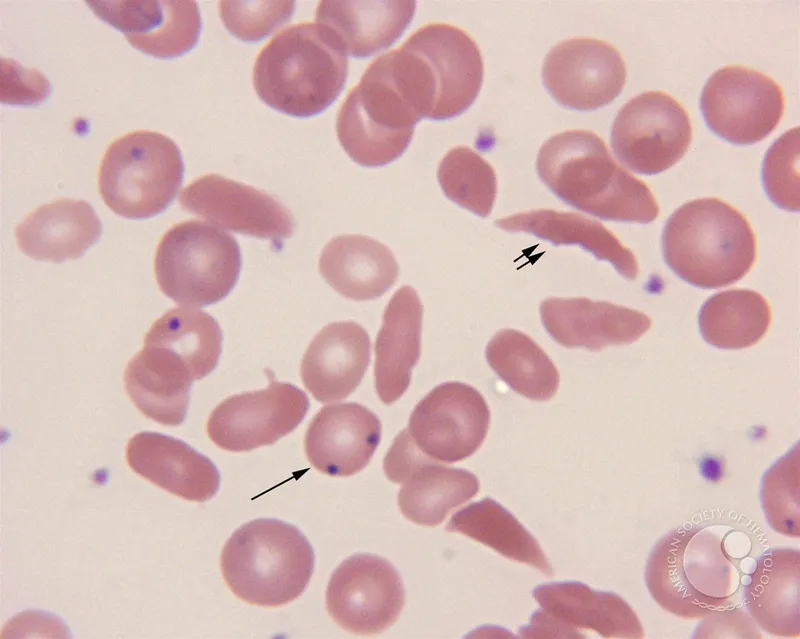
⭐ Acute Chest Syndrome: A leading cause of death. Defined by a new pulmonary infiltrate on CXR plus fever, cough, or chest pain. Often triggered by infection or fat embolism from bone marrow.
Complications - The Vaso-Occlusive Fallout
- General: Chronic hemolysis → bilirubin gallstones (cholelithiasis), aplastic crisis (Parvovirus B19).
- Organ-Specific Damage:
- Brain: Stroke (ischemic > hemorrhagic).
- Lungs: Acute Chest Syndrome (ACS) - new infiltrate + fever/respiratory symptoms.
- Kidney: Papillary necrosis → hematuria; renal medullary carcinoma.
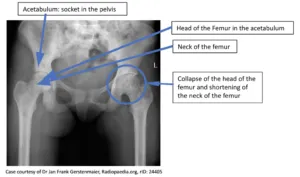
- Bone: Avascular necrosis (femoral/humeral head), osteomyelitis (📌 Salmonella > S. aureus).
- Spleen: Autosplenectomy → ↑ risk of encapsulated bacteria (S. pneumo, H. flu, N. meningitidis).
- GU: Priapism.
⭐ Exam Favorite: While S. aureus is the most common cause of osteomyelitis in the general population, Salmonella species are classically associated with osteomyelitis in patients with sickle cell disease.
Management - Taming the Crisis
- Acute Vaso-occlusive Crisis (VOC):
- 📌 HOP to it: Hydration (IVF), Oxygen (if SpO₂ <94%), Pain control (opioids).
- Vigorously search for and treat infectious triggers.
- Chronic Management & Prevention:
- Hydroxyurea: ↑ HbF, reducing sickling and crisis frequency.
- Folic acid supplementation (due to high RBC turnover).
- Routine vaccinations (esp. S. pneumoniae, H. influenzae, N. meningitidis).
- Transfusions for severe anemia or stroke prevention.
⭐ Hydroxyurea is a cornerstone of chronic management but can cause myelosuppression (neutropenia, anemia, thrombocytopenia), requiring regular blood count monitoring.
High‑Yield Points - ⚡ Biggest Takeaways
- Autosomal recessive point mutation in the β-globin gene (glutamic acid to valine) causes HbS.
- Hallmarks are vaso-occlusive crises (VOC), causing severe pain, and chronic hemolytic anemia.
- Acute chest syndrome is the leading cause of death in adults; presents with fever, cough, and chest pain.
- Functional asplenia increases susceptibility to encapsulated organisms like S. pneumoniae.
- Aplastic crisis is most commonly precipitated by Parvovirus B19 infection.
- Hydroxyurea is the primary disease-modifying therapy; it works by increasing fetal hemoglobin (HbF).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

