ICDs - Shocking Rhythms Right
- Primary Prevention of SCD:
- Reduces mortality in HFrEF (NYHA II-III) with LVEF ≤ 35% despite ≥3 months of optimal medical therapy (OMT).
- Also for post-MI (>40 days) with LVEF ≤ 30%.
- Patient must have a reasonable expectation of survival > 1 year.
- Secondary Prevention of SCD:
- Survivors of cardiac arrest from ventricular tachycardia (VT) or fibrillation (VF).
- Spontaneous sustained VT.
- Mechanism:
- Detects fatal arrhythmias (VT/VF).
- Delivers a high-energy shock to defibrillate.
- Can also use anti-tachycardia pacing (ATP).
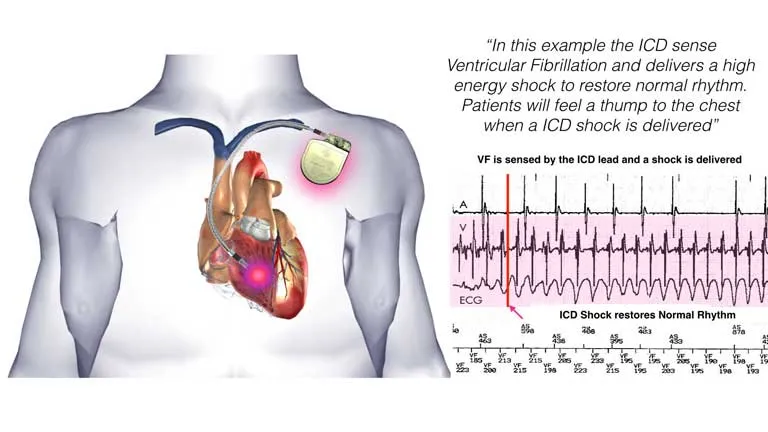
⭐ ICD placement is delayed for at least 40 days post-MI and 90 days post-revascularization (PCI/CABG) to allow for potential LV function recovery and avoid treating transient electrical instability.
CRT - Syncing Up the Squeeze
- Goal: Corrects electrical dyssynchrony (e.g., LBBB) to improve the mechanical efficiency of the heart's contraction. It's essentially a "biventricular pacemaker."
- Core Indications:
- NYHA Class II-IV symptoms on optimal medical therapy.
- LVEF ≤ 35%.
- Wide QRS complex ≥ 150 ms, particularly with LBBB morphology.
- Mechanism: Paces both right and left ventricles simultaneously, restoring a coordinated squeeze. The LV lead is typically placed via the coronary sinus.
- Outcomes: Improves symptoms, reduces HF hospitalizations, promotes reverse LV remodeling, and provides a mortality benefit.
⭐ High-Yield: The presence of a Left Bundle Branch Block (LBBB) is the strongest ECG predictor of a positive clinical response to CRT.
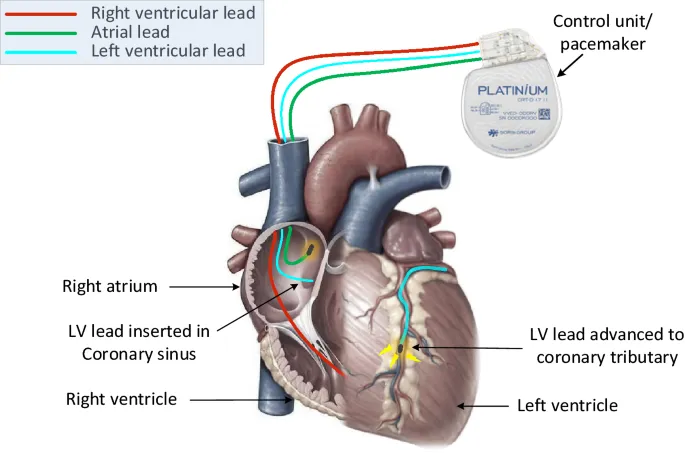
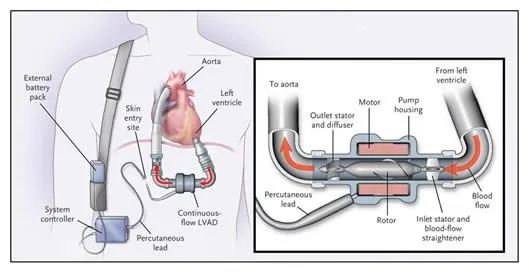
LVADs - The Mechanical Bridge
- Function: A surgically implanted mechanical pump that draws blood from the left ventricle and pumps it into the aorta, unloading the LV and improving systemic perfusion.
- Indications:
- Bridge-to-Transplant (BTT): For transplant-eligible patients awaiting a donor heart.
- Destination Therapy (DT): Permanent support for transplant-ineligible patients with end-stage HF (NYHA Class IV).
- Bridge-to-Recovery (BTR): Temporary support to allow native heart recovery.
- Complications:
- Bleeding (esp. GI from acquired von Willebrand disease & AVMs).
- Thrombosis (pump, aortic root) & Stroke.
- Driveline infections.
- Right heart failure.
⭐ Clinical Pearl: Continuous flow from an LVAD often results in a non-palpable pulse. Blood pressure must be measured with a Doppler ultrasound to obtain a mean arterial pressure (MAP); the target is typically 65-85 mmHg.
Device Algorithm - The Big Picture
- Eligibility: Symptomatic HFrEF (NYHA II-IV) on Guideline-Directed Medical Therapy (GDMT).
- ICD (Primary Prevention): LVEF ≤ 35% + reasonable expectation of survival > 1 year.
- CRT: Add for LVEF ≤ 35%, Sinus Rhythm, + LBBB with QRS ≥ 150 ms for maximal benefit.
⭐ The greatest mortality benefit from Cardiac Resynchronization Therapy (CRT) is observed in patients with a wide QRS complex (≥ 150 ms) and Left Bundle Branch Block (LBBB) morphology.
High‑Yield Points - ⚡ Biggest Takeaways
- ICDs are primarily for preventing sudden cardiac death in HFrEF patients with an LVEF ≤35%; wait at least 40 days post-MI.
- CRT is for symptomatic HFrEF (NYHA II-IV) with LVEF ≤35% and a wide QRS (≥150 ms, esp. LBBB) to improve symptoms and mortality.
- CRT-D is a combination device used when criteria for both an ICD and CRT are met.
- LVADs are used as a bridge-to-transplant or destination therapy for end-stage, refractory heart failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

