ADHF Basics - The Pump Falters
- Definition: Acute or sub-acute worsening of chronic heart failure signs and symptoms, requiring urgent medical intervention. It represents a catastrophic failure of the heart's pumping ability, leading to systemic/pulmonary congestion (wet) or hypoperfusion (cold).
- Precipitants (📌 FAILURE):
- Forgot Meds (non-compliance)
- Arrhythmia (e.g., AFib)
- Ischemia/Infarction
- Lifestyle (↑Na+/fluid)
- Upregulation (infection)
- Renal failure
- Embolism (Pulmonary)
⭐ The most common cause of right-sided heart failure is left-sided heart failure.
Presentation & Phenotypes - Signs of Sinking
Key signs are driven by two axes: congestion (wet) and hypoperfusion (cold).
- Congestion ("Wet"):
- Pulmonary: Rales, orthopnea, paroxysmal nocturnal dyspnea (PND).
- Systemic: Jugular venous distension (JVD), peripheral edema, ascites.
- Hypoperfusion ("Cold"):
- Cool extremities, altered mental status, narrow pulse pressure, worsening renal function.
⭐ "Warm & Wet" is the most common clinical phenotype, presenting with adequate perfusion but significant congestion.

Diagnostics - Confirming the Crisis
- Labs:
- ↑ BNP (>400 pg/mL) or NT-proBNP.
- Troponins (rule out ACS), renal function (BMP).
- Imaging:
- ECG: Check for ischemia, arrhythmia triggers.
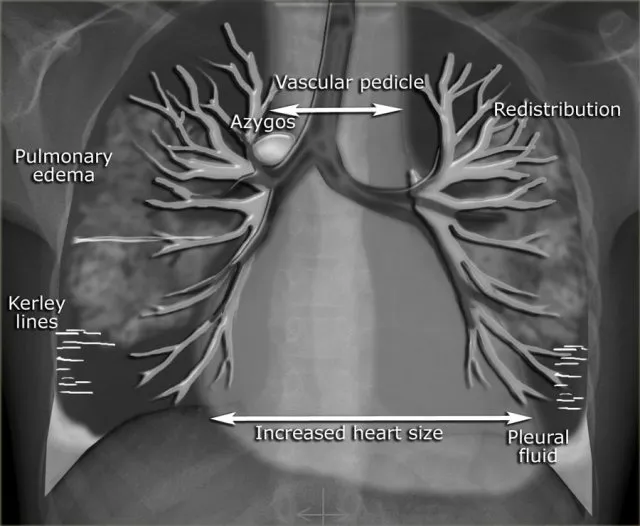
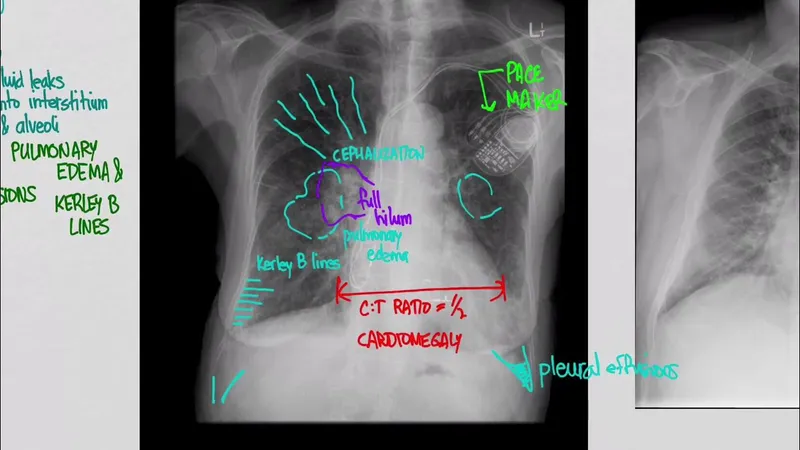
- CXR: Cardiomegaly, cephalization, Kerley B lines, pleural effusion.
- Echocardiogram (Key): Assesses LVEF, diastolic function, valves, filling pressures.
⭐ A normal BNP level (<100 pg/mL) has a high negative predictive value, making ADHF unlikely.
Management - Stemming the Tide
Initial stabilization focuses on identifying the clinical profile: congestion ("wet" vs. "dry") and perfusion ("warm" vs. "cold"). This guides therapy.
-
Immediate Interventions (📌 LMNOP):
- Lasix (Furosemide): IV bolus, typically 2-2.5x the patient's home oral dose.
- Morphine: For severe dyspnea and anxiety; causes venodilation. Use cautiously.
- Nitrates (Nitroglycerin): Reduces preload and afterload. Best for patients without hypotension.
- Oxygen: Maintain SpO₂ > 90%; consider BiPAP for respiratory distress.
- Position: Have the patient sit upright with legs dangling to reduce preload.
-
Profile-Guided Therapy:
- Congestion ("Wet"): IV loop diuretics are the cornerstone. For refractory edema, consider adding a thiazide diuretic.
- Hypoperfusion ("Cold"): If systolic BP is < 90 mmHg, start inotropes (Dobutamine, Milrinone) to improve cardiac output.
⭐ High-Yield: Avoid initiating or uptitrating beta-blockers during an acute decompensation episode. They can be continued only if the patient is on a stable chronic dose and not in cardiogenic shock.
High-Yield Points - ⚡ Biggest Takeaways
- Acute decompensated heart failure (ADHF) is a clinical diagnosis, often triggered by non-compliance, arrhythmias, or ischemia.
- The "warm & wet" profile (well-perfused but congested) is the most common presentation, treated with IV diuretics and vasodilators.
- "Cold & wet" patients (hypoperfused and congested) may require inotropes (dobutamine) if hypotensive.
- Always assess for and address the underlying precipitant of decompensation.
- Do not initiate beta-blockers and use caution with existing doses during acute decompensation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

