Pathophysiology & Genetics - Gluten's Gut Grudge
- Genetic Predisposition: Over 95% of patients have HLA-DQ2 or HLA-DQ8 haplotypes. This is necessary but not sufficient for disease development.
- Pathogenesis:
- Trigger: Gliadin, a component of gluten, is resistant to degradation.
- Key Enzyme: Tissue transglutaminase (tTG) deamidates gliadin, increasing its immunogenicity.
- Immune Cascade: Antigen-presenting cells (APCs) present deamidated gliadin on HLA-DQ2/8 molecules to CD4+ T-cells, initiating a Th1-mediated inflammatory response.
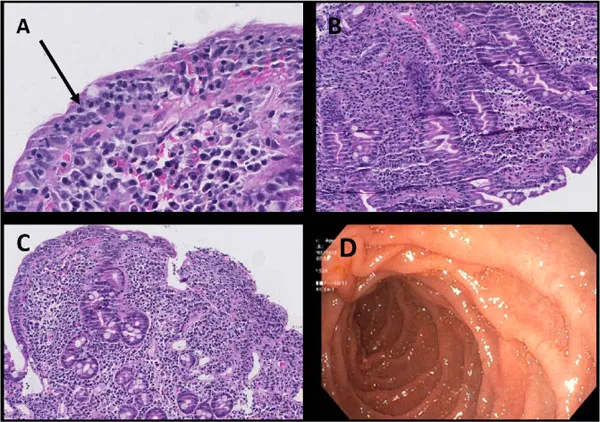
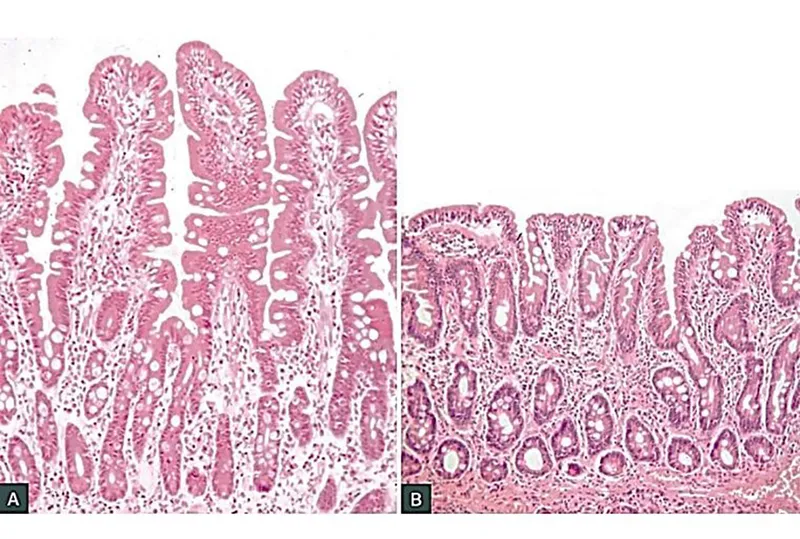
- Result: Leads to characteristic small bowel findings: villous atrophy, crypt hyperplasia, and ↑ intraepithelial lymphocytes.
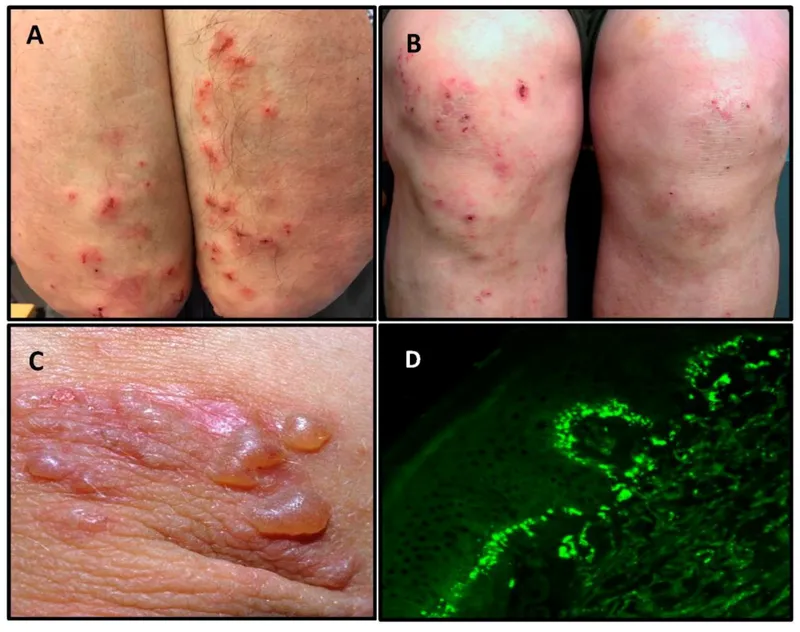
⭐ Dermatitis herpetiformis, an intensely pruritic papulovesicular rash on extensor surfaces, is a pathognomonic skin manifestation caused by IgA deposition in the dermal papillae.
Clinical Presentation - The Celiac Chameleon
- Classic GI (Malabsorptive): Chronic diarrhea, steatorrhea, weight loss, bloating, abdominal distension.
- Atypical (Extra-intestinal): More common in adults.
- Dermatologic: Dermatitis herpetiformis (pruritic papulovesicles on extensor surfaces).
- Hematologic: Refractory iron deficiency anemia, folate deficiency.
- Skeletal: ↓ bone mineral density, osteomalacia, osteoporosis.
- Neurologic: Peripheral neuropathy, cerebellar ataxia.
- Reproductive: Infertility, recurrent fetal loss.
⭐ Celiac disease is strongly associated with other autoimmune conditions, especially Type 1 Diabetes and autoimmune thyroiditis (Hashimoto's).
Diagnosis - Catching the Culprit
- Initial Screening:
- IgA anti-tissue transglutaminase (tTG) antibody is the single best serologic test.
- If suspicion is high despite negative IgA tTG, check for selective IgA deficiency. If present, order IgG-based tests (e.g., IgG-DGP).
- Gold Standard:
- Small bowel biopsy (duodenal) is required for confirmation.
- 📌 VACIng the gut: Villous Atrophy, Crypt hyperplasia, Intraepithelial lymphocytosis.
- Genetic Testing:
- HLA-DQ2/DQ8 testing has a >99% negative predictive value. Useful to rule out the disease.
⭐ Dermatitis herpetiformis (pruritic papules/vesicles on extensor surfaces) is pathognomonic. A skin biopsy showing granular IgA deposits at the dermal-epidermal junction can confirm the diagnosis without needing an intestinal biopsy.
Management & Complications - Dodging the Dough
-
Primary Treatment: Lifelong, strict gluten-free diet (GFD).
- Avoid wheat, barley, rye. 📌 Mnemonic: Barely Reaching Wheat.
- Permitted: Rice, corn, soy, potatoes.
-
Nutritional Support: Correct deficiencies at diagnosis.
- Commonly supplement iron, folate, vitamin B12, calcium, and vitamin D.
-
Monitoring: Follow-up with serology (tTG-IgA) to ensure dietary adherence and intestinal healing.
-
Complications of Untreated/Refractory Disease:
- Anemia (iron deficiency), osteoporosis.
- Dermatitis Herpetiformis: Pruritic papules/vesicles on extensor surfaces.
- Malignancy: Increased risk of small bowel adenocarcinoma & Enteropathy-Associated T-cell Lymphoma (EATL).
⭐ EATL is a rare but aggressive T-cell lymphoma of the small intestine; it is a feared complication almost exclusively seen in celiac disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Celiac disease is an autoimmune disorder triggered by gliadin in genetically susceptible individuals, primarily those with HLA-DQ2/DQ8.
- The most specific and sensitive initial test is IgA anti-tissue transglutaminase (tTG) antibody.
- The gold standard for diagnosis is a small bowel biopsy showing villous atrophy, most prominent in the duodenum.
- Strongly associated with dermatitis herpetiformis, a pruritic papulovesicular rash.
- Management is a strict, lifelong gluten-free diet.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

