ECG & Pathophysiology - Chaotic Conduction
- Atrial Fibrillation (A-Fib):
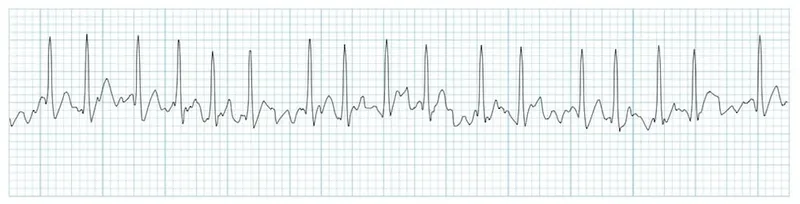
- ECG: Irregularly irregular rhythm, no P waves, chaotic fibrillatory (f) waves, narrow QRS.
- Pathophysiology: Multiple ectopic foci near pulmonary vein ostia fire chaotically (>350 bpm), leading to asynchronous atrial contraction & variable AV node conduction.
- Atrial Flutter:
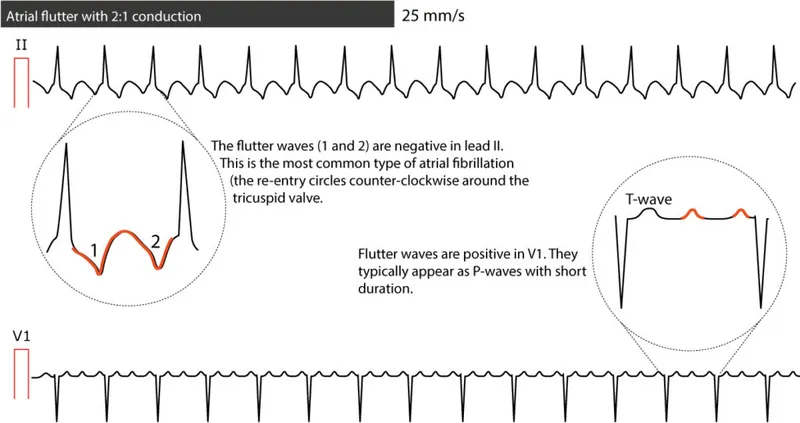
- ECG: "Sawtooth" flutter (F) waves (best in II, III, aVF). Atrial rate ~300 bpm. Ventricular rate is a fraction of atrial rate due to AV block (e.g., 2:1, 3:1).
- Pathophysiology: Large re-entrant circuit.

⭐ High-Yield: The re-entrant circuit in typical atrial flutter involves the cavo-tricuspid isthmus, a key target for catheter ablation.
Presentation & Workup - Spotting the Signs
- Presentation: Palpitations, dyspnea, fatigue, or asymptomatic.
- Physical Exam: Irregularly irregular pulse (AFib) or a rapid, regular pulse (AFlutter).
Key Investigations
- ECG is diagnostic:
- AFib: No P waves, irregularly irregular R-R intervals, fibrillatory waves.
- AFlutter: Characteristic "sawtooth" flutter waves, especially in leads II, III, aVF.
- Labs: Check TSH/T4 (thyrotoxicosis), electrolytes (K+, Mg++), CBC.
- Echocardiogram (TTE): Crucial to assess for underlying structural heart disease, valvular function, and chamber size. TEE is better for spotting left atrial appendage thrombus.
⭐ In a young patient without structural heart disease, always ask about triggers like binge drinking ("holiday heart syndrome"), stress, or caffeine.
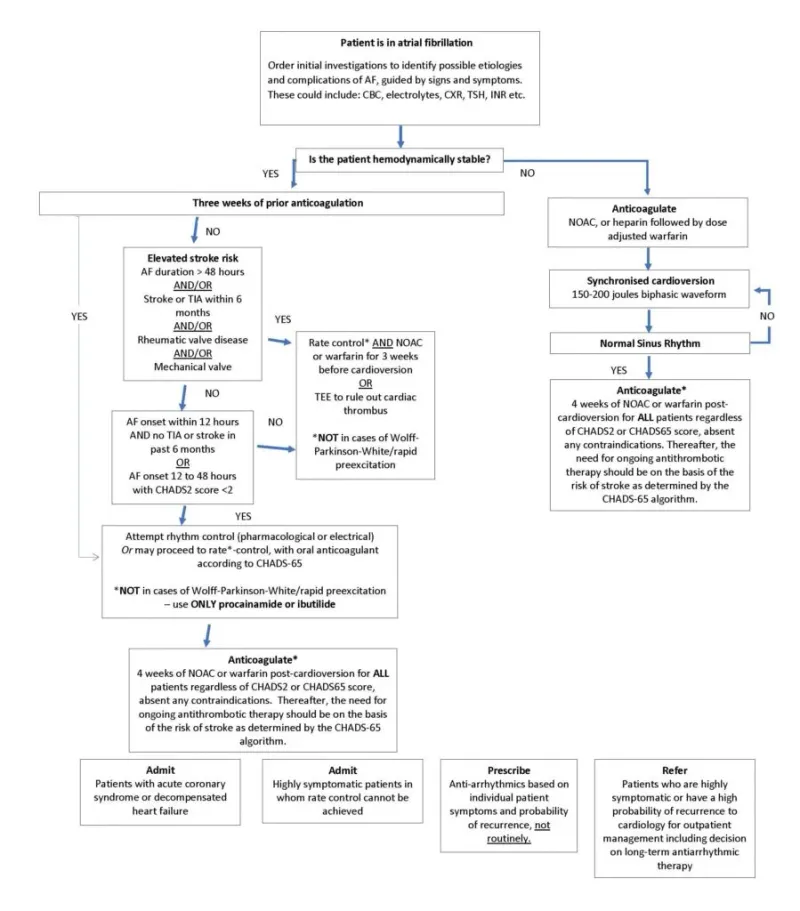
Acute Management - Taming the Tachycardia
Initial assessment hinges on hemodynamic stability. The primary goal is controlling the rapid ventricular rate (RVR).
- Rate Control Agents:
- β-Blockers: Metoprolol, Esmolol.
- Non-DHP CCBs: Diltiazem, Verapamil (Avoid in HFrEF).
- Digoxin: Slower onset; useful in hypotension or HFrEF.
- Amiodarone: Refractory cases or if other agents are contraindicated.
- Anticoagulation: Assess stroke risk (CHA₂DS₂-VASc). If AF duration >48h or unknown, anticoagulation is needed before elective cardioversion.
⭐ In patients with Heart Failure with reduced Ejection Fraction (HFrEF), non-dihydropyridine calcium channel blockers (Verapamil, Diltiazem) are contraindicated due to their negative inotropic effects, which can worsen heart failure.
Chronic Management - Clots & Control
1. Anticoagulation (Clot Prevention)
- Stroke Risk: Assessed via CHA₂DS₂-VASc score to guide therapy.
- Action Thresholds:
- Score ≥ 2 (males) or ≥ 3 (females): Anticoagulation indicated.
- Options: Direct Oral Anticoagulants (DOACs) are first-line over Warfarin.
- 📌 CHA₂DS₂-VASc: CHF, HTN, Age ≥75 (2), Diabetes, Stroke/TIA (2), Vascular dz, Age 65-74, Sex category (Female).
2. Rate & Rhythm Control
- Rate Control First:
- Goal: Lenient resting HR < 110 bpm if asymptomatic.
- Agents: β-blockers, non-dihydropyridine CCBs (diltiazem, verapamil).
- Rhythm Control:
- Consider for persistent symptoms despite rate control.
- Methods: Cardioversion, antiarrhythmic drugs (amiodarone, flecainide).
⭐ The HAS-BLED score (HTN, Abnormal renal/liver fxn, Stroke, Bleeding history, Labile INRs, Elderly >65, Drugs/alcohol) assesses bleeding risk before starting anticoagulants.
High‑Yield Points - ⚡ Biggest Takeaways
- Atrial fibrillation is an irregularly irregular rhythm with no P waves; atrial flutter shows a sawtooth pattern.
- The biggest risk is thromboembolism (stroke); use the CHA₂DS₂-VASc score to guide anticoagulation.
- Rate control is the initial strategy, most commonly with β-blockers or calcium channel blockers.
- Rhythm control (cardioversion, ablation) is reserved for persistent symptoms or hemodynamic instability.
- For stroke prevention, direct oral anticoagulants (DOACs) are preferred over warfarin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

