Pathophysiology - Cracking Plaques
- Foundation: Atherosclerosis leads to vulnerable plaques in coronary arteries.
- Plaque Morphology: Characterized by a thin, rupture-prone fibrous cap over a large, inflammatory lipid-rich necrotic core.
- The Event: Spontaneous or stress-induced rupture/erosion of the plaque exposes its highly thrombogenic contents (e.g., collagen, tissue factor) to the blood.
- Thrombus Formation: This triggers rapid platelet adhesion and aggregation, forming a non-occlusive, platelet-rich (white) thrombus.
- Result: The thrombus reduces coronary blood flow, causing myocardial ischemia and anginal symptoms, but without complete vessel blockage.
⭐ Unstable Angina (UA) and NSTEMI exist on a continuum, sharing the same pathophysiology. The key difference is the severity and duration of ischemia: in UA, it's insufficient to cause detectable myocyte necrosis (i.e., cardiac biomarkers are negative).
Clinical Presentation & Diagnosis - The Heart's Cry
- Chest Pain: Retrosternal, crushing/pressure, radiating to arm/jaw.
- New onset: Severe, limiting activity.
- Crescendo: ↑ frequency, duration, or intensity.
- At rest: Lasting > 20 minutes.
- Physical Exam: Often normal; may show diaphoresis, S4 gallop, or signs of heart failure.
⭐ Key Discriminator: Unstable Angina is defined by the absence of elevated cardiac enzymes (troponins). It represents myocardial ischemia without infarction.
Risk Stratification - Scoring Severity
-
TIMI Score: Estimates mortality for patients with UA/NSTEMI. One point for each risk factor.
-
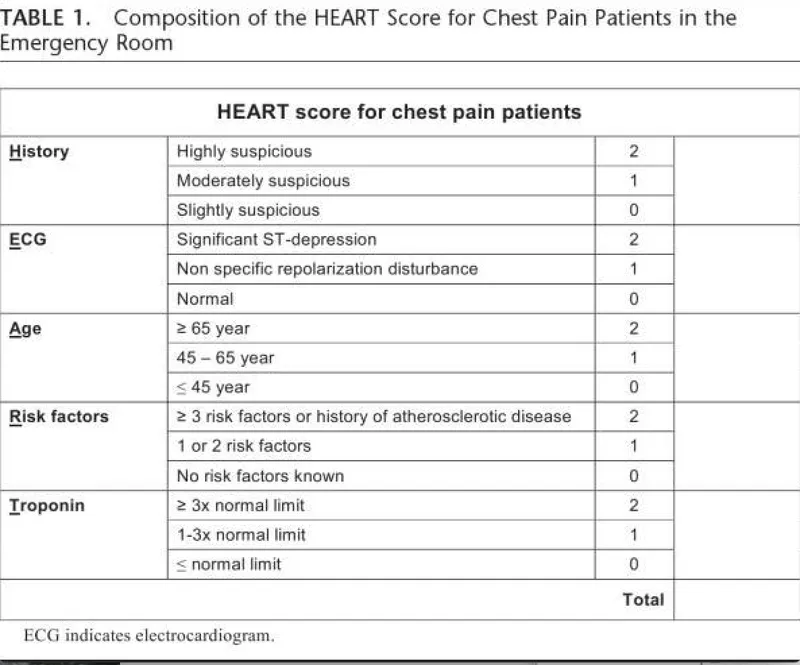
HEART Score: Predicts 6-week risk of Major Adverse Cardiac Events (MACE).
⭐ HEART Score Components: History, ECG, Age, Risk factors, Troponin. A score of 0-3 is low risk and supports discharge.
Management - Code Red Care
Initial therapy aims to stabilize the patient and prevent further thrombosis.
📌 MONA-BASH
- Morphine: For refractory angina.
- Oxygen: Supplemental, only if O₂ saturation < 90%.
- Nitrates: Sublingual or IV for active pain. ⚠️ Caution: Avoid in hypotension, RV infarction, or recent PDE5 inhibitor use.
- Antiplatelet Therapy:
- Aspirin (162-325 mg) chewed immediately, followed by daily 81 mg.
- P2Y12 inhibitor (e.g., clopidogrel, ticagrelor).
- Beta-blocker: Start within 24 hours if no signs of heart failure or shock.
- Anticoagulation: LMWH (enoxaparin) or UFH.
- Statin: High-intensity (e.g., Atorvastatin 80 mg) initiated early.
⭐ In cocaine-induced ACS, avoid beta-blockers due to the risk of unopposed alpha-stimulation. Use benzodiazepines for anxiety and sympathetic surge.
High‑Yield Points - ⚡ Biggest Takeaways
- Unstable Angina is new-onset, accelerating, or rest angina representing acute myocardial ischemia.
- It is distinguished from NSTEMI by normal cardiac biomarkers; there is no myocardial necrosis.
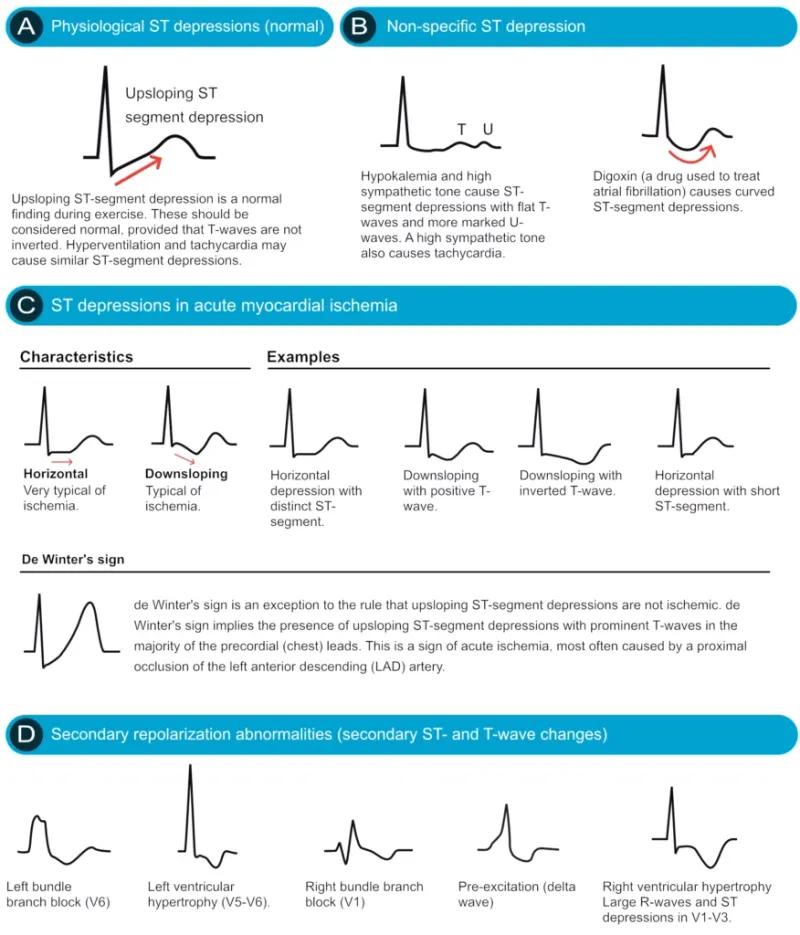
- EKG findings are often transient ST-segment depression or T-wave inversions, but can be normal.
- Caused by a non-occlusive thrombus over a disrupted atherosclerotic plaque.
- Management focuses on antiplatelet and anticoagulant therapy to prevent progression to MI.
- Risk stratification (e.g., TIMI score) is crucial to guide timing for angiography.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

