Antiplatelet MOA - Plugging the Problem
- Aspirin (ASA): Irreversibly inhibits COX-1, blocking Thromboxane A₂ ($TXA_2$) synthesis → ↓ platelet aggregation.
- $P2Y_{12}$ Receptor Blockers: Inhibit ADP-mediated platelet activation & aggregation.
- Clopidogrel/Prasugrel: Irreversible binding.
- Ticagrelor: Reversible binding.
- GPIIb/IIIa Inhibitors: (e.g., Abciximab) Directly block the final common pathway, preventing fibrinogen cross-linking.
⭐ Ticagrelor is a reversible allosteric inhibitor of $P2Y_{12}$, unlike the irreversible thienopyridines (Clopidogrel, Prasugrel). Its faster offset is crucial for patients needing urgent surgery.
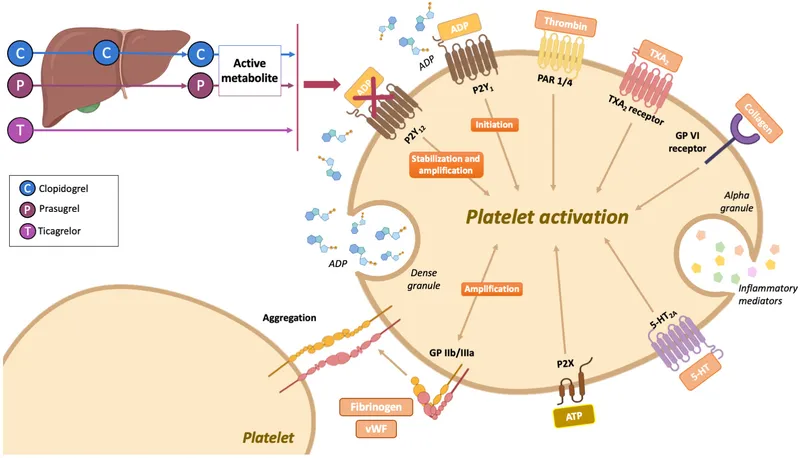
Drug Classes - The Antiplatelet Arsenal
-
Aspirin (ASA): Irreversibly inhibits COX-1, blocking thromboxane A₂ (TXA₂) synthesis. Crucial first-line agent.
- Loading dose: 162-325 mg (chewable).
-
P2Y₁₂ Receptor Blockers: Inhibit ADP-mediated platelet aggregation. 📌 Mnemonic: "TCP" for Ticagrelor, Clopidogrel, Prasugrel.
| Drug | Mechanism | Key Feature |
|---|---|---|
| Clopidogrel | Irreversible, Prodrug | Requires CYP2C19 activation |
| Prasugrel | Irreversible, Prodrug | More potent, rapid onset |
| Ticagrelor | Reversible | Not a prodrug, faster offset |
- Agents: Abciximab, Eptifibatide, Tirofiban.
- Use: Typically reserved for high-risk patients undergoing PCI.
⭐ Prasugrel is contraindicated in patients with a history of stroke or TIA due to an increased risk of significant bleeding.
DAPT Strategy - The ACS Battle Plan
- Core Principle: Combine Aspirin + a P2Y12 inhibitor to prevent stent thrombosis and recurrent ischemic events.
- Aspirin:
- Loading Dose: 162-325 mg (non-enteric coated, chewable) STAT.
- Maintenance Dose: 81 mg daily, lifelong.
- P2Y12 Inhibitors ("The Grels"):
- Ticagrelor (Brilinta): Preferred for most ACS (STEMI/NSTEMI). Reversible, faster onset.
- Prasugrel (Effient): Most potent. Use only in patients undergoing PCI. ⚠️ Contraindicated in prior TIA/stroke.
- Clopidogrel (Plavix): Used when others are contraindicated, in fibrinolysis, or high bleeding risk.
- Standard Duration: 12 months for most ACS patients. Duration may be tailored using the DAPT score (ischemic vs. bleeding risk).
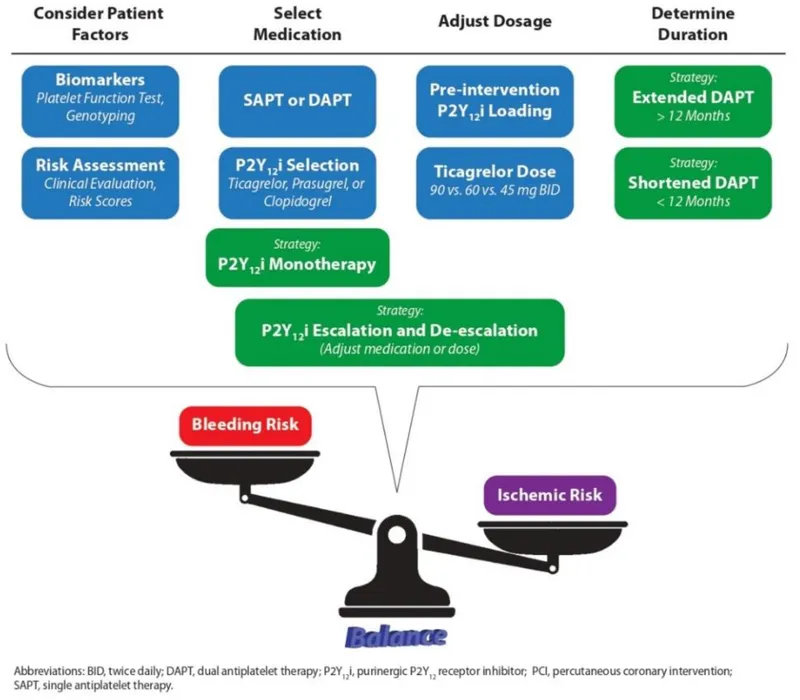
⭐ In patients managed with fibrinolysis for STEMI, clopidogrel is the only P2Y12 inhibitor with proven safety and efficacy in that specific setting.
Side Effects - The Bleeding Edge
- Primary Risk: Bleeding
- Major: Intracranial Hemorrhage (ICH), GI Bleed.
- Minor: Epistaxis, ecchymosis, hematuria.
- ⚠️ Assess bleed risk (e.g., prior history, age >75).
- Drug-Specific Effects:
- Aspirin: GI upset, peptic ulcers.
- Clopidogrel/Prasugrel: ⚠️ Thrombotic Thrombocytopenic Purpura (TTP).
- Ticagrelor: Dyspnea (common, often transient), ↑uric acid, bradyarrhythmias.
⭐ Prasugrel is contraindicated in patients with a history of stroke or TIA due to an increased risk of intracranial bleeding.
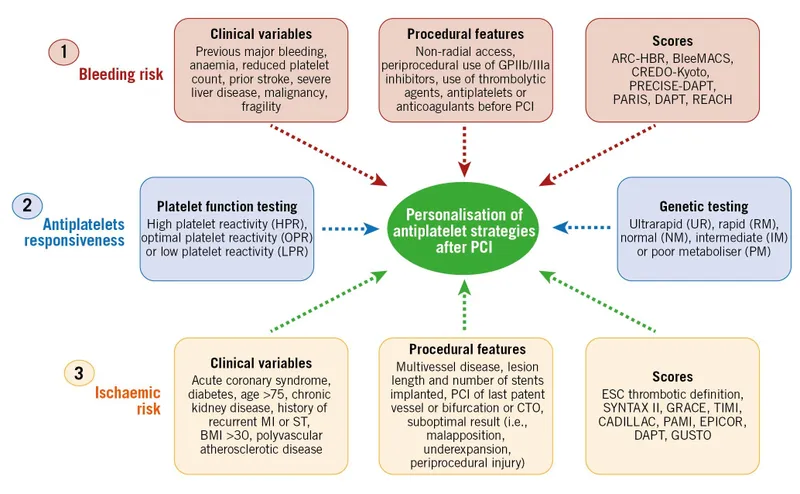
- Dual antiplatelet therapy (DAPT) with Aspirin and a P2Y12 inhibitor is the cornerstone of ACS management.
- Continue Aspirin indefinitely and a P2Y12 inhibitor for at least 12 months after the event.
- Prasugrel is contraindicated in patients with a history of stroke or TIA due to ↑ bleeding risk.
- A common side effect of Ticagrelor is dyspnea.
- GP IIb/IIIa inhibitors (e.g., Abciximab) are potent agents for high-risk PCI cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

