Pathophysiology - Plaque Attack
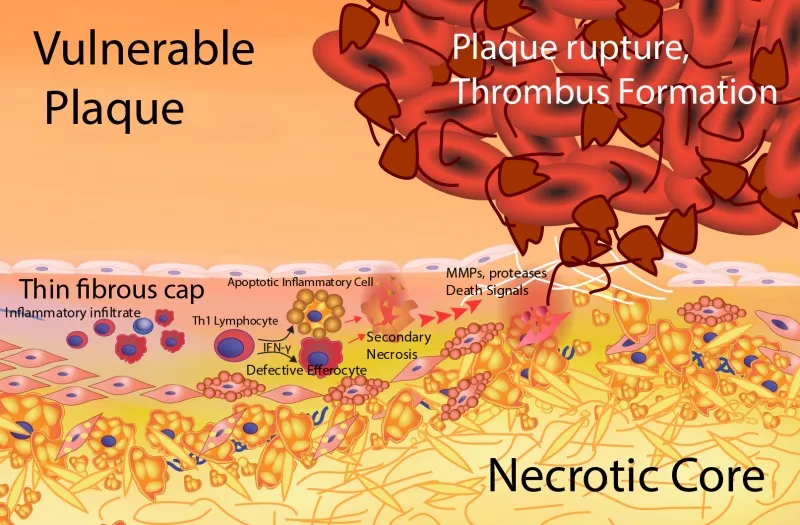
- Atherosclerosis builds vulnerable plaques: large lipid cores, thin fibrous caps, and active inflammation.
- Rupture is triggered by:
- Inflammation: Macrophages release matrix metalloproteinases (MMPs) that digest the fibrous cap.
- Shear Stress: Mechanical force from blood flow.
⭐ Macrophages are key culprits; they secrete matrix metalloproteinases (MMPs) that degrade the plaque's protective fibrous cap, making it prone to rupture.
- 📌 Mnemonic (Pathway): Rupture → Exposure → Adhesion → Coagulation → Thrombus (REACT).
Myocardial Ischemia - The Energy Crisis
- Pathogenesis: Imbalance between myocardial oxygen supply and demand, most often from coronary artery obstruction.
- Cellular Cascade:
- Switch from aerobic to anaerobic metabolism → $↓ATP$ & $↑Lactate$.
- Failure of ion pumps (e.g., $Na^+/K^+$ ATPase) → ion imbalance & cellular swelling.
- Injury Spectrum:
- Reversible: < 20 min of ischemia leads to stunned or hibernating myocardium.
- Irreversible: Ischemia lasting ~20-40 minutes or more results in coagulative necrosis.
⭐ Vulnerability Hotspot: The subendocardium is the most vulnerable region to ischemia due to its high oxygen demand and tenuous blood supply.
ACS Classification - The Great Divide
- ECG is the critical first step. It divides Acute Coronary Syndrome (ACS) into two main pathways: ST-Elevation Myocardial Infarction (STEMI) and Non-ST-Elevation ACS (NSTE-ACS), guiding immediate reperfusion strategy.
- STEMI: Caused by a fully occlusive thrombus leading to transmural ischemia. ECG shows persistent ST-segment elevation in ≥2 contiguous leads.
- NSTE-ACS (UA/NSTEMI): From a partially occlusive thrombus causing subendocardial ischemia. ECG may show ST-depression or T-wave inversions.
- Cardiac biomarkers are the tie-breaker:
- NSTEMI: Positive troponins (myocardial necrosis).
- Unstable Angina (UA): Negative troponins (ischemia without necrosis).
- Cardiac biomarkers are the tie-breaker:
⭐ A posterior wall STEMI may not show classic ST elevation; instead, look for ST depression in leads V1-V3 and consider posterior leads (V7-V9).
Cardiac Biomarkers - The Troponin Tale
- Troponin I & T: Most sensitive and specific markers for myocardial necrosis.
- Rises in 2-4 hrs, peaks at ~24-48 hrs, and remains elevated for 7-14 days.
- CK-MB: Useful for detecting re-infarction due to its shorter duration.
- Rises in 4-6 hrs, peaks at ~24 hrs, and normalizes within 48-72 hrs.
- Myoglobin: Earliest marker to rise, but lacks specificity.
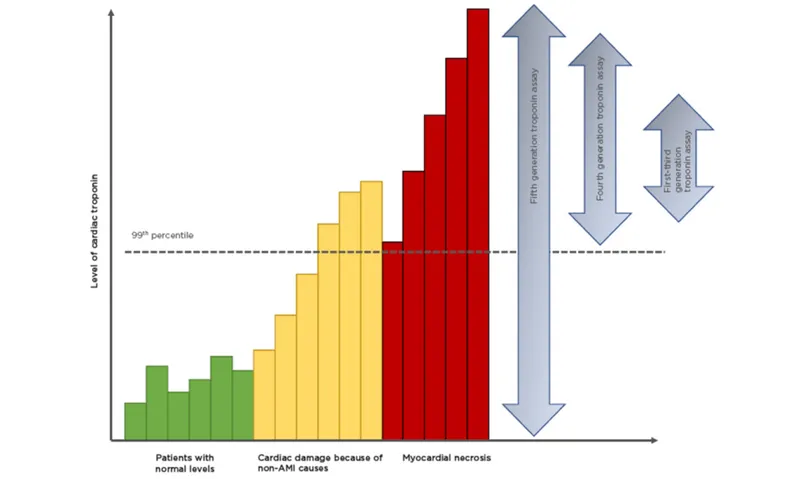
⭐ High-sensitivity troponin (hs-cTn) can detect myocardial injury earlier, but a negative result within the first few hours of symptom onset does not rule out ACS.
- ACS is a spectrum from unstable angina (UA) to MI, driven by plaque rupture and intracoronary thrombosis.
- UA vs. NSTEMI is distinguished by cardiac biomarkers; troponins are elevated only in NSTEMI.
- NSTEMI vs. STEMI is distinguished by ECG: NSTEMI has ST depression/T-wave inversion, while STEMI has ST-segment elevation.
- Complete coronary occlusion causes a STEMI, whereas partial occlusion leads to UA or NSTEMI.
- The fundamental problem is a mismatch in myocardial oxygen supply and demand.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

