Breast Cancer Screening - Mammo Mission
- USPSTF: Biennial mammography for women 50-74 years. Individualize for ages 40-49.
- ACS: Annual mammography for women 45-54, then biennial for ≥55. Option to start at 40.
- High-Risk Screening: For patients with >20-25% lifetime risk (e.g., BRCA carriers, prior mantle radiation).
- Start annual Breast MRI + mammogram at age 30.
⭐ The Gail model assesses a woman's risk of developing invasive breast cancer over the next 5 years.
Cervical Cancer Screening - Pap Power Play
- Ages 21-29: Pap smear (cytology) alone every 3 years.
- Ages 30-65: Choice of:
-
- Pap smear every 3 years.
-
- High-risk HPV (hrHPV) testing every 5 years.
-
- Co-testing (Pap + hrHPV) every 5 years.
-
- Age >65: Stop screening if prior results negative & no history of CIN2+.
⭐ HPV types 16 and 18 are the culprits in ~70% of cervical cancers and high-grade cervical intraepithelial neoplasia (CIN).
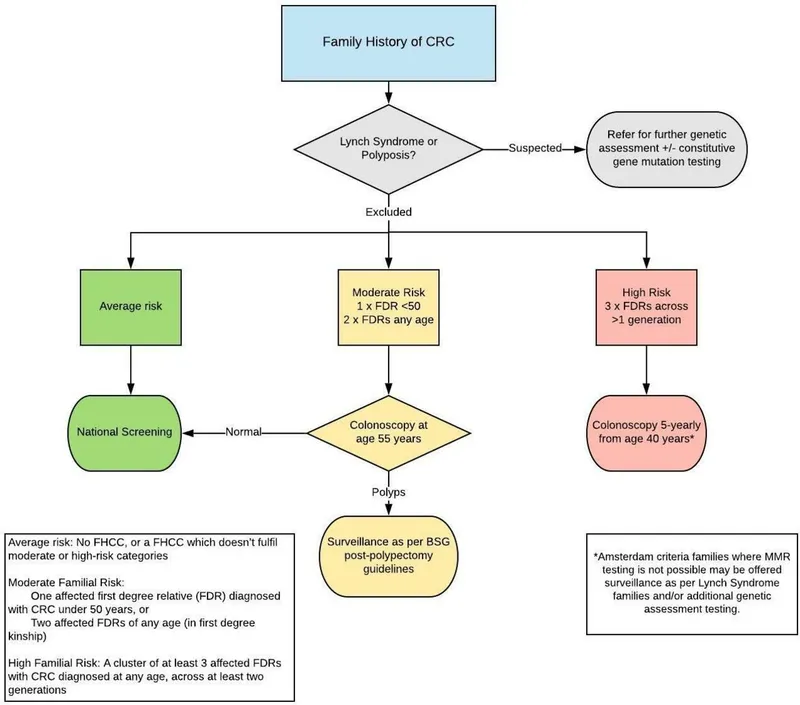
Colorectal Cancer Screening - Colonoscopy Countdown
- Average-Risk: Start at age 45, continue to 75. Decision to screen from 76-85 is individualized.
- Primary Options:
- Colonoscopy: every 10 years.
- FIT (Fecal Immunochemical Test): annually.
- sDNA-FIT (e.g., Cologuard): every 3 years.
- 1st-Degree Relative w/ CRC: Start at age 40 or 10 years before relative's diagnosis; repeat colonoscopy every 5 years.
⭐ Lynch Syndrome (HNPCC): Start colonoscopy at 20-25 years; repeat every 1-2 years.
Lung Cancer Screening - Smoker's Scan
- Indication: Screen high-risk individuals to reduce lung cancer mortality.
- Criteria (USPSTF):
- Age 50-80 years
- ≥20 pack-year smoking history
- Current smoker or have quit within the past 15 years
- Method: Annual screening with low-dose computed tomography (LDCT).
- Discontinuation:
- Quit smoking for >15 years
- Develops a life-limiting illness
- Reaches age 81
⭐ Annual screening with LDCT in high-risk patients is proven to reduce mortality from lung cancer, making it a critical preventive measure.
Prostate Cancer Screening - PSA Predicament
- USPSTF Grade C for men aged 55-69 years; decision is individualized.
- Screening not routinely recommended for average-risk men <'''55''' or >70 years.
- Shared Decision-Making is Key: Discuss pros and cons before testing.
- Benefits: Potential ↓ in mortality.
- Harms: False positives (e.g., BPH, prostatitis), overdiagnosis, and treatment complications (incontinence, erectile dysfunction).
- Consider earlier screening (40-45 yrs) for high-risk groups (African American, strong family history).

⭐ To prevent one death from prostate cancer, ~1,000 men must be screened and ~48 treated, highlighting the significant risk of overtreatment.
- Cervical Cancer: Screen women 21-65. Pap smear every 3 years or, for ages 30-65, Pap + HPV co-testing every 5 years.
- Breast Cancer: Biennial mammography for women aged 50-74. Start at age 40 for high-risk individuals.
- Colorectal Cancer: Start screening at age 45. Colonoscopy every 10 years is a primary option.
- Lung Cancer: Annual low-dose CT for adults 50-80 with a 20 pack-year smoking history.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

