Red Flags in Headache - SNOOPy's on the Case
📌 SNOOPy mnemonic for serious underlying causes:
- Systemic symptoms: Fever, weight loss, history of malignancy.
- Neurologic signs: Focal deficits, papilledema, altered mental status.
- Onset: Sudden, abrupt, "thunderclap" headache (peaks within 1 minute).
- Older age: New headache in a patient > 50 years (risk of giant cell arteritis).
- Pattern change: Change in frequency, severity, or clinical features.
- yardstick: Precipitated by Valsalva maneuver (coughing, sneezing), suggesting ↑ ICP.
⭐ A thunderclap headache requires immediate investigation for subarachnoid hemorrhage (SAH), typically starting with a non-contrast head CT.

SNOOP Mnemonic - The Red Flag Framework
📌 SNOOP helps identify secondary causes of headache requiring urgent investigation.
- Systemic Symptoms or Secondary Risk Factors:
- Fever, chills, night sweats, weight loss
- History of malignancy, HIV, or immunosuppression
- Neurologic Signs or Symptoms:
- Focal neurologic deficits (e.g., weakness, sensory loss)
- Papilledema, cranial nerve palsies
- Altered mental status or seizures
- Onset:
- Sudden, abrupt, or "thunderclap" onset (peak intensity < 1 minute)
- Older Age of Onset:
- New headache onset after age 50
- Pattern Change:
- Progressive headache with ↑ frequency or severity
- Change in attack characteristics or quality
⭐ A "thunderclap headache" is a classic presentation of subarachnoid hemorrhage (SAH) and warrants immediate neuroimaging (non-contrast head CT).
Neurologic Signs - Alarming Exam Findings
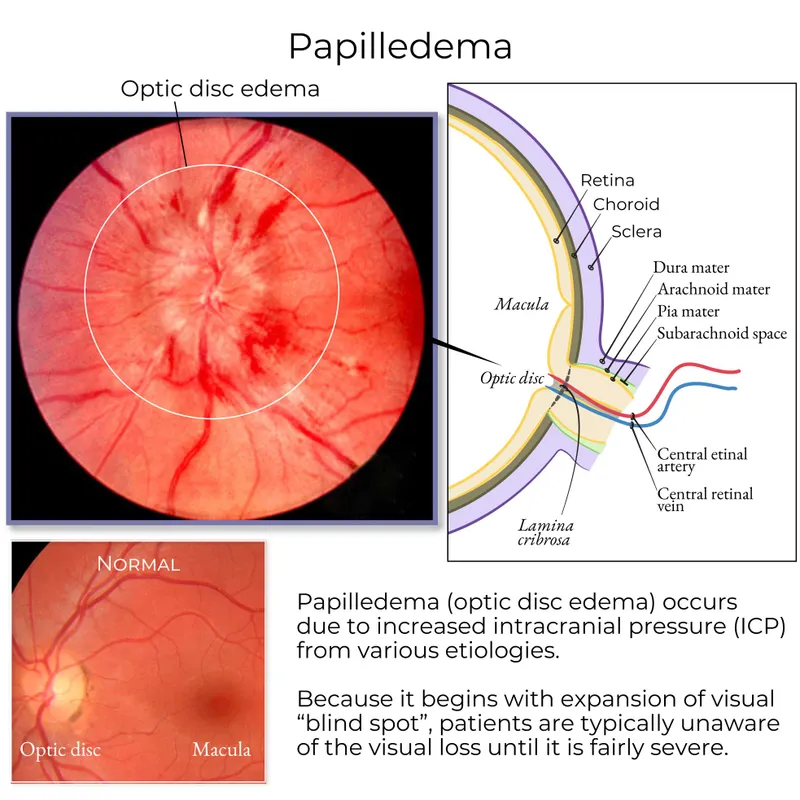
- Papilledema:
- Optic disc swelling with blurred margins on fundoscopy.
- A key sign of ↑ intracranial pressure (ICP).
- Mandates urgent neuroimaging (CT/MRI) to investigate for mass lesions, hydrocephalus, or cerebral venous thrombosis.

- Focal Neurological Deficits (FNDs):
- New, objective weakness, sensory loss, reflex changes (e.g., Babinski sign), or coordination difficulties (e.g., ataxia).
- Suggests a structural brain lesion (e.g., stroke, tumor, abscess).
- Altered Mental Status (AMS):
- Confusion, drowsiness, lethargy, or a decline in consciousness (Glasgow Coma Scale < 15).
- Indicates diffuse brain dysfunction or impending herniation.
⭐ A unilateral, fixed, and dilated pupil ("blown pupil") suggests compression of the oculomotor nerve (CN III), often from uncal herniation-a neurosurgical emergency.
Onset & History - Timing is Everything
- "Worst headache of life": A classic red flag, demanding immediate attention.
- Thunderclap Onset: ⚠️ Reaches maximum intensity in < 1 minute.
- Strongly suggests Subarachnoid Hemorrhage (SAH).
- Requires emergent non-contrast head CT.
- Concerning Temporal Patterns:
- New-onset headache in patients > 50 years (risk for Giant Cell Arteritis).
- Headache that progressively worsens or changes character.
- Precipitated by Valsalva (coughing, bending) or exertion; suggests ↑ ICP.
- Wakes a patient from sleep.
⭐ If an initial non-contrast head CT is negative in a patient with a thunderclap headache, a lumbar puncture is mandatory to rule out SAH by checking for xanthochromia.

High-Yield Points - ⚡ Biggest Takeaways
- "Worst headache of life" is a classic sign of subarachnoid hemorrhage (SAH).
- New-onset headache in patients >50 should raise suspicion for giant cell arteritis.
- Fever and nuchal rigidity accompanying a headache strongly suggest meningitis.
- Focal neurologic deficits or seizures point to a structural brain lesion like a tumor or abscess.
- Papilledema on exam indicates increased intracranial pressure (ICP).
- Headaches that worsen with exertion or are positional also suggest ↑ ICP.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

