CCS Time Advancement - The Clock is Ticking
- Advance time only when the patient is stable and you are awaiting results or treatment effects.
- Key triggers: Post-ordering labs/imaging, after initiating treatment.
- Common intervals: 2, 5, 10, 15, 30 mins, matching test/drug onset time.
- ⚠️ Never advance time on an unstable patient. Address acute changes (e.g., ↓BP, ↑HR) immediately.
- On time return: ALWAYS re-check vitals & perform a relevant physical exam before proceeding.
⭐ The most common error is advancing the clock when a patient's condition worsens. Always stabilize first!
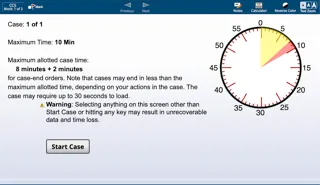
Decision Triggers - Green Light, Red Light
Deciding when to advance the clock is critical. Use this simple framework to guide your actions and maximize your score.
-
Green Light Conditions (Advance Time):
- Patient is stable or improving.
- All immediate diagnostic and therapeutic orders are in.
- You are waiting for non-critical results or consults.
-
Red Light Conditions (Hold Time):
- Unstable vitals (e.g., ↓BP, ↑HR, ↓SpO₂).
- An acute event occurs (e.g., seizure, chest pain).
- A critical result returns (e.g., K⁺ >6.0 mEq/L).
⭐ The 2-Minute Drill: In the final 2 minutes, stop advancing time. Perform a final check of vitals, review all orders, and complete health maintenance/counseling tasks (e.g., vaccinations, smoking cessation) to close the case completely.
Advancement Intervals - Hops, Skips, and Leaps
-
Your choice of time advancement reflects clinical judgment. Match the interval to the patient's stability and the clinical setting.
-
Hops (Minutes): 🐇
- When: Unstable patients, acute events, or awaiting STAT results/medication effects.
- Action: Advance 2-5 minutes to re-evaluate vitals, check response to an IV drug, or get a critical lab result.
- Example: Post-intubation check, response to IV furosemide.
-
Skips (Hours to Days): 🏃
- When: Stable inpatients or for outpatient follow-up.
- Action: Advance 2-6 hours for ward patients, or 1-3 days for clinic follow-up.
- Example: Awaiting routine culture results, next-day ward round.
-
Leaps (Weeks to Months): 🚀
- When: Chronic disease management, health maintenance in stable outpatients.
- Action: Advance 2-4 weeks or 3-6 months for long-term follow-up.
- Example: HbA1c check in a controlled diabetic, annual wellness visit.
⭐ Exam Tip: Never leap forward with a new, undiagnosed complaint or an unstable patient. Always re-evaluate after any intervention before a significant time jump.
Common Pitfalls - Time-Travel Traps
- Premature Advancement: Jumping forward without sufficient data, leading to missed diagnoses and management errors.
- Post-Intervention Neglect: Failing to re-assess patient stability and response before advancing time. This is a critical, frequently penalized error.
- Ignoring Case Rhythm: Rushing a critical patient or dawdling with a stable one. Match your pace to the patient's acuity.
- Missing Critical Windows: Forgetting time-sensitive treatments (e.g., thrombolysis, antibiotics in sepsis).
⭐ A classic error is advancing time immediately after ordering a treatment, without first confirming the patient's response or any adverse effects.
High‑Yield Points - ⚡ Biggest Takeaways
- Advance time primarily when awaiting test results in a stable patient.
- The goal is to efficiently simulate waiting periods without missing key events.
- Advance only by the time needed for the slowest test result to become available.
- Never advance time on an unstable or actively deteriorating patient.
- Always re-evaluate the patient immediately after a time jump for any changes.
- Incorrect advancement risks missing critical deteriorations, leading to case failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

