Decision Framework - The First Cut
- Initial Triage: The first question is always stability. Is the patient hemodynamically stable or unstable?
- The Surgical Trigger: The presence of generalized peritonitis, visceral perforation, or refractory shock mandates surgical intervention.
⭐ In trauma, "hard signs" of vascular injury (e.g., pulsatile bleeding, expanding hematoma, bruit/thrill) are direct triggers for surgical exploration, bypassing extensive imaging.
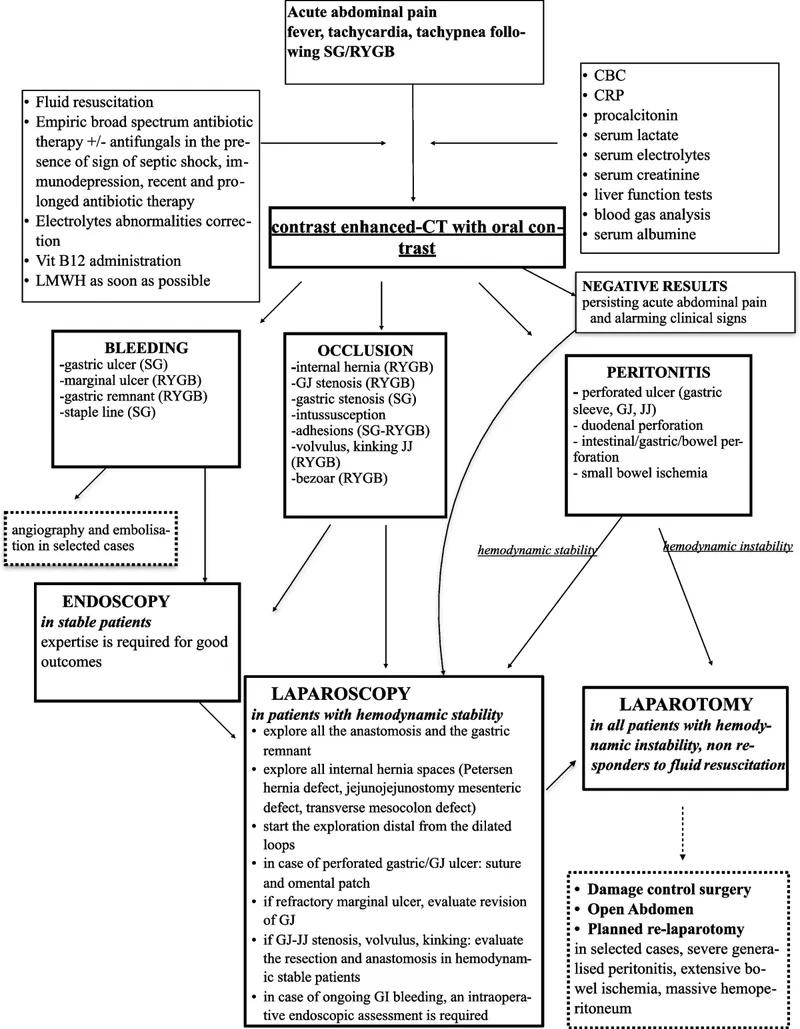
Trauma Triage - Red Flags & Green Lights
Initial assessment dictates the path: immediate surgery or watchful waiting. The decision hinges on hemodynamic stability and signs of peritoneal violation.
-
🔴 Red Flags (Surgical Emergency):
- Hemodynamic instability (SBP < 90 mmHg).
- Peritonitis, guarding, or rebound tenderness.
- Evisceration or impalement.
- Positive FAST scan in an unstable patient.
- Penetrating trauma with suspected peritoneal breach (e.g., gunshot).
-
🟢 Green Lights (Consider Non-Operative Management - NOM):
- Hemodynamically stable.
- No peritoneal signs.
- Isolated solid organ injury (low-grade) on CT without active bleeding.
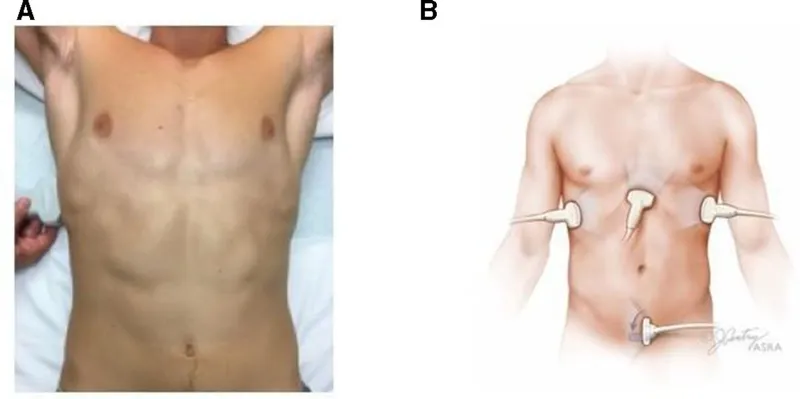
⭐ In profoundly unstable patients, Damage Control Surgery is key: an abbreviated laparotomy to control major hemorrhage and contamination, followed by ICU resuscitation before definitive repair.
Acute Abdomen - Gut Instincts
Deciding between surgical and non-surgical management hinges on identifying peritonitis and hemodynamic instability. Early and accurate assessment is key.
-
Surgical (Operative) Triggers:
- Peritonitis: Guarding, rigidity, rebound tenderness.
- Hemodynamic Instability: Persistent hypotension despite fluid resuscitation.
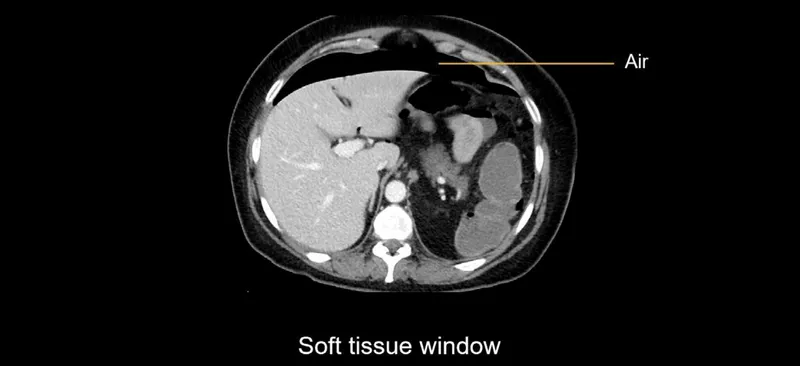
- Visceral Perforation: Free air under the diaphragm on imaging.
- Strangulated hernia, bowel ischemia, or complete obstruction.
-
Non-Surgical (Conservative) Management:
- Indicated for: Uncomplicated pancreatitis, diverticulitis, medical causes (e.g., DKA, porphyria).
- Core components: Nil per os (NPO), IV fluids, analgesia, antibiotics.
- Requires close monitoring for any deterioration.
⭐ Silent Abdomen: In elderly, diabetic, or immunosuppressed patients, classic signs of peritonitis may be absent. Maintain a high index of suspicion for perforation even without overt signs.
Vascular Crises - Time is Tissue
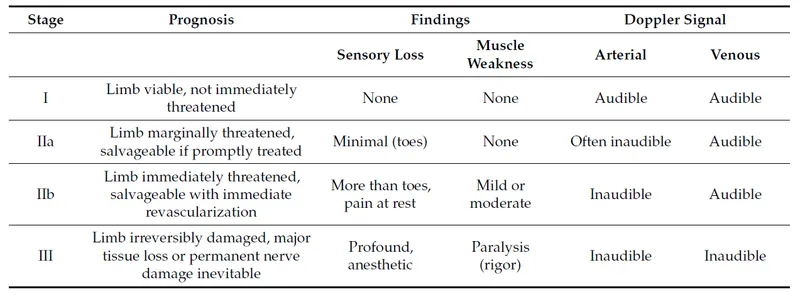
- Immediate Management: IV Heparin bolus, then continuous infusion.
- Diagnosis: Hand-held Doppler, confirmed with CT Angiography (CTA).
- 📌 6 P's of ALI: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia.
- Critical Window: Revascularization goal is <6 hours to maximize limb salvage.
⭐ The most common site for a peripheral arterial embolus is the common femoral artery bifurcation.
High‑Yield Points - ⚡ Biggest Takeaways
- Hemodynamic instability or generalized peritonitis are hard indications for immediate surgery.
- Failure of non-operative management (NOM), evidenced by clinical worsening, necessitates surgical intervention.
- Pneumoperitoneum on imaging is a classic sign of hollow viscus perforation requiring laparotomy.
- The primary surgical goal is source control: repair, drain, or resect.
- For high-risk surgical patients, prioritize less invasive options like percutaneous drainage when possible.
- Always weigh the pathology against the patient's physiological reserve and comorbidities.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

