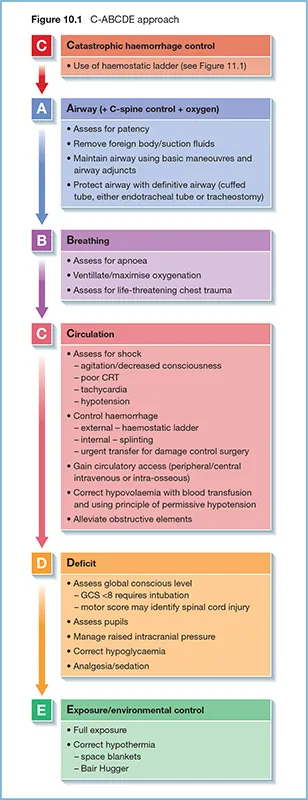
Primary Survey - The ABCDE Drill
A sequential, systematic approach for managing critically ill patients. Treat life-threats at each step before proceeding to the next.
-
A - Airway with C-Spine Protection:
- Assess: Patency, stridor, foreign body.
- Intervene: Jaw thrust, suction, Oropharyngeal/Nasopharyngeal Airway (OPA/NPA), intubation. Maintain C-spine immobilisation.
-
B - Breathing & Ventilation:
- Assess: Respiratory Rate (RR), SpO₂, chest expansion, air entry.
- Intervene: High-flow O₂, bag-mask ventilation, needle decompression.
-
C - Circulation & Hemorrhage Control:
- Assess: Heart Rate (HR), Blood Pressure (BP), Capillary Refill Time (CRT), active bleeding.
- Intervene: Stop external bleeding, secure 2 large-bore IV lines, start crystalloid infusion.
-
D - Disability (Neurological Status):
- Assess: GCS/AVPU score, pupillary size & reaction, blood glucose.
-
E - Exposure & Environment:
- Assess: Fully expose patient to check for injuries.
- Intervene: Prevent hypothermia (warm blankets, warmed fluids).
⭐ In trauma, altered sensorium is due to head injury, hypoxia, or shock until proven otherwise. Always check blood glucose.
Shock Management - Classify & Conquer
- Goal: Restore perfusion; MAP > 65 mmHg, normalize lactate.
- Initial Approach: ABCs, secure IV access (2 large-bore cannulas), start fluid resuscitation with crystalloids (e.g., 30 ml/kg in sepsis), and identify the cause.
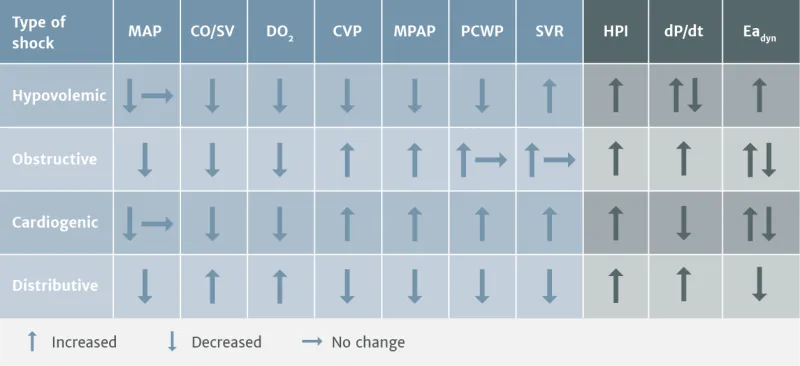
Classification & Hemodynamics:
- Hypovolemic: ↓ Preload (hemorrhage, dehydration). Tx: Fluids/blood.
- Cardiogenic: ↓ Cardiac Output (MI, HF). Tx: Inotropes (Dobutamine), cautious fluids.
- Distributive: ↓ SVR (sepsis, anaphylaxis). Tx: Vasopressors (Norepinephrine), fluids.
- Obstructive: Extracardiac obstruction (tamponade, PE). Tx: Relieve obstruction (e.g., pericardiocentesis).
⭐ Exam Favourite: In septic shock, Norepinephrine is the first-choice vasopressor to maintain MAP ≥ 65 mmHg. If MAP remains low despite Norepinephrine, consider adding Vasopressin.
ICU Interventions - Vents, Lines & Drugs
-
Mechanical Ventilation:
- Modes: Assist-Control (ACV), SIMV, Pressure Support (PSV).
- Key Settings:
- Tidal Volume (Vt): 6-8 mL/kg IBW (lower in ARDS).
- PEEP: Start 5-8 cm H₂O; titrate for oxygenation.
- FiO₂: Titrate for SpO₂ >92%.
-
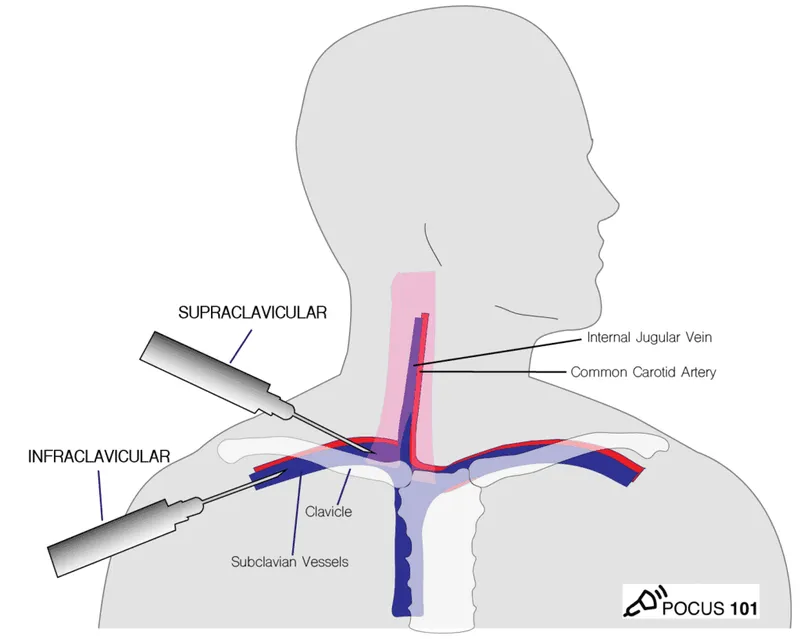
Central Venous Access:
- Sites: Internal Jugular (IJV) preferred > Subclavian > Femoral (↑ infection/DVT risk).
- Confirmation: CXR (tip at cavo-atrial junction).
-
Vasoactive Drugs:
- Vasopressors: Noradrenaline (1st line, septic shock), Adrenaline.
- Inotropes: Dobutamine (cardiogenic shock), Milrinone.
⭐ Propofol Infusion Syndrome (PRIS): A lethal complication of high-dose (>4 mg/kg/hr) or prolonged (>48 hrs) infusion. Features: metabolic acidosis, rhabdomyolysis, arrhythmias, and cardiac failure.
High‑Yield Points - ⚡ Biggest Takeaways
- Airway first, always: Intubate for GCS < 8, impending airway compromise, or inability to clear secretions.
- Breathing: Provide high-flow O₂. Perform needle thoracostomy for a tension pneumothorax before getting a chest X-ray.
- Circulation: Secure 2 large-bore IV lines. Start crystalloid bolus for hypotension; add vasopressors (like norepinephrine) if refractory.
- Disability: Check GCS and pupils. Always check a blood glucose level in any patient with altered mental status.
- Sepsis: Administer broad-spectrum antibiotics within the first hour of recognition.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

