Nitrogen Disposal - The Backup Plan
- When the urea cycle fails, the body uses backup systems to handle toxic ammonia (NH₃), primarily involving glutamine.
- Glutamine Synthesis (Peripheral Tissues):
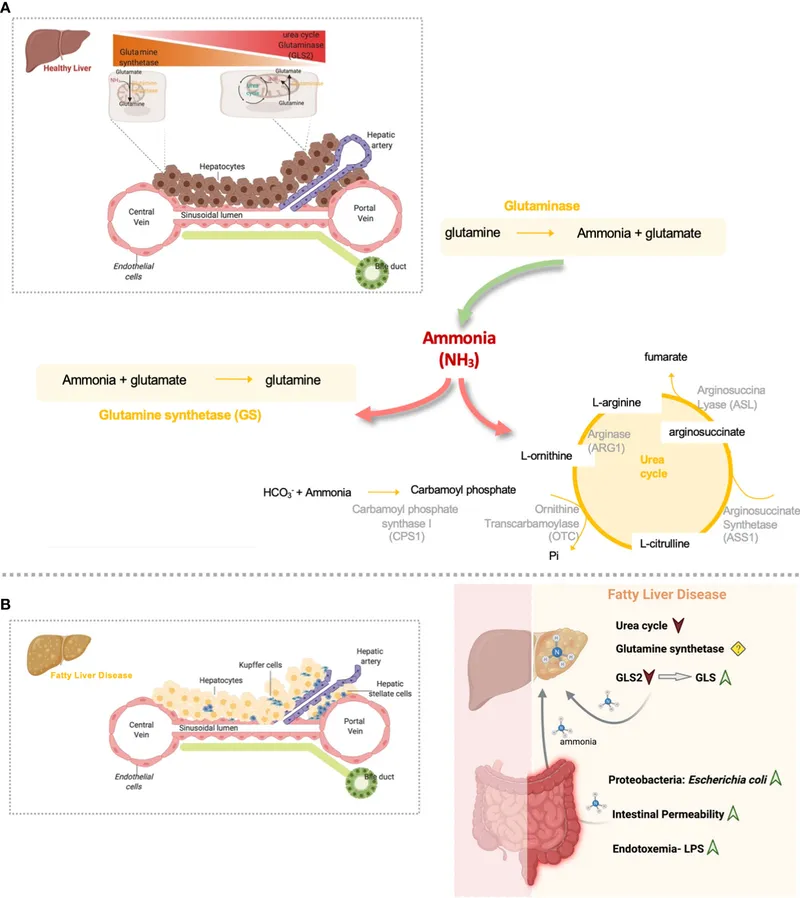
- Glutamine Synthetase combines ammonia with glutamate to form glutamine, a non-toxic nitrogen carrier.
- Reaction: $Glutamate + NH_4^+ + ATP \rightarrow Glutamine + ADP + P_i$
- Glutamine is then safely transported via the blood to the kidneys.
- Renal Ammoniagenesis (Kidneys):
- Glutaminase in renal tubular cells cleaves glutamine back into glutamate and ammonia.
- The liberated NH₃ is protonated to ammonium ($NH_4^+$) and excreted in the urine.
- This process is crucial during acidosis, as $H^+$ excretion is coupled with bicarbonate ($HCO_3^−$) generation.
⭐ Treatment for hyperammonemia (e.g., urea cycle defects) often involves sodium phenylbutyrate or sodium benzoate. These drugs conjugate with glutamine and glycine, creating alternative nitrogen excretion products.
Muscle-Liver Shuttle - The Alanine Circuit

-
A crucial, non-toxic method for transporting excess nitrogen from muscle to the liver for conversion into urea, while recycling carbon skeletons.
-
In Muscle (Fasting State):
- Muscle protein is broken down for energy, producing amino groups ($NH_3$).
- Pyruvate (from glycolysis) accepts an amino group to form Alanine.
- This reaction is catalyzed by Alanine Aminotransferase (ALT), which requires Vitamin B6.
- Alanine is then released into the bloodstream.
-
In Liver:
- ALT converts Alanine back to Pyruvate and releases the amino group.
- The amino group enters the Urea Cycle.
- Pyruvate is used as a substrate for gluconeogenesis to produce new glucose.
- This glucose is released into the blood and can be used by tissues like muscle.
⭐ High-Yield: The Alanine cycle is essentially an inter-organ loop that moves both nitrogen and the carbon skeleton of pyruvate from muscle to the liver. The liver bears the metabolic cost of gluconeogenesis, sparing muscle glucose.
Kidney's Role - Acidosis & Ammonia
- Primary Function: Kidneys excrete the daily metabolic acid load (~1 mEq/kg/day), primarily as ammonium ($NH_4^+$).
- Key Adaptation in Acidosis: In metabolic acidosis, renal ammoniagenesis is the principal adaptive response to increase acid excretion.
- Mechanism:
- Proximal tubule cells metabolize glutamine using glutaminase.
- Pathway: $Glutamine \rightarrow Glutamate \rightarrow \alpha-Ketoglutarate + 2 NH_4^+$
- $NH_4^+$ is secreted into the tubular lumen for excretion.
- This process simultaneously generates new bicarbonate ($HCO_3^-$), which is reabsorbed to help buffer systemic acidosis.

⭐ High-Yield: Hypokalemia stimulates, while hyperkalemia inhibits, renal ammonia synthesis. This is a crucial link between potassium balance and acid-base regulation, as acidosis-induced hyperkalemia can paradoxically limit the compensatory renal response.
High‑Yield Points - ⚡ Biggest Takeaways
- In urea cycle defects, the body uses alternative pathways to excrete nitrogen and reduce hyperammonemia.
- Ammonia scavengers are key drugs. Sodium benzoate combines with glycine to form hippurate, which is then excreted.
- Sodium phenylbutyrate is converted to phenylacetate, which conjugates with glutamine to form phenylacetylglutamine for excretion.
- These pathways provide a "nitrogen sink," bypassing the deficient urea cycle and removing toxic ammonia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

