Core Pathway - The Sobering Process
Ethanol is metabolized primarily in the liver through a two-step oxidation process. The pathway relies on two key enzymes and the cofactor $NAD^+$. The accumulation of products and cofactors has significant metabolic consequences, with the rate-limiting step being Alcohol Dehydrogenase.
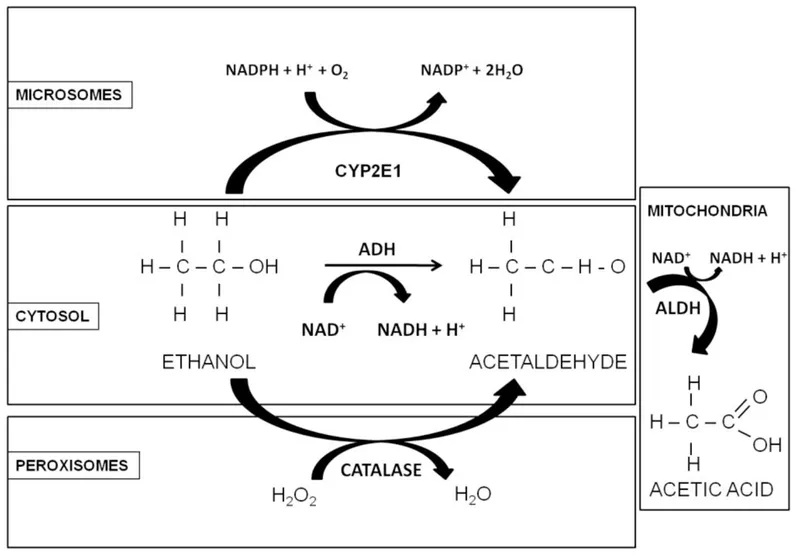
- Step 1 (Cytosol): Ethanol is oxidized to acetaldehyde by Alcohol Dehydrogenase (ADH).
- Step 2 (Mitochondria): Toxic acetaldehyde is oxidized to acetate by Acetaldehyde Dehydrogenase (ALDH).
- Cofactor Impact: Both steps require $NAD^+$ as an electron acceptor, converting it to $NADH$. This drastically increases the $NADH/NAD^+$ ratio, impacting other metabolic pathways.
⭐ Fomepizole competitively inhibits Alcohol Dehydrogenase. It is a crucial antidote for methanol or ethylene glycol poisoning, preventing their conversion to toxic metabolites.
MEOS Pathway - The Chronic Route
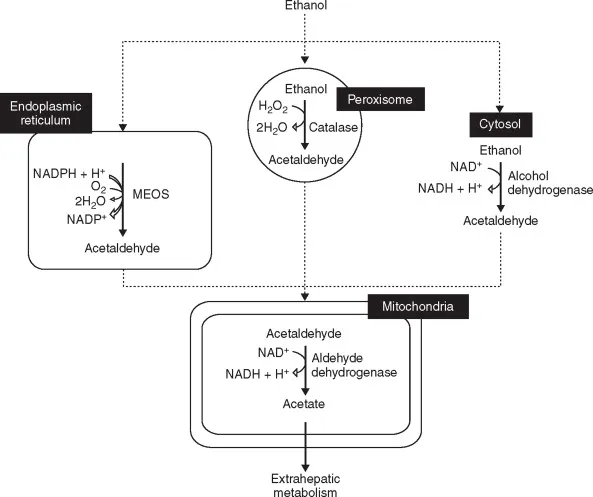
- Location & Enzyme: Smooth Endoplasmic Reticulum; key enzyme is Cytochrome P450 2E1 (CYP2E1).
- Activation: An inducible pathway activated during chronic alcohol consumption.
- Reaction: Converts ethanol to acetaldehyde, consuming NADPH and oxygen.
- Induction: Chronic alcohol use upregulates CYP2E1, leading to ↑ alcohol tolerance and ↑ metabolic rate of other drugs.
⭐ MEOS induction by chronic alcohol use increases the metabolism of other drugs (e.g., acetaminophen), raising the risk of toxicity from their metabolites.
Metabolic Mayhem - The NADH Hangover
- Alcohol metabolism via alcohol & aldehyde dehydrogenase massively ↑ the NADH/NAD+ ratio. This redox state shift is central to alcohol-induced metabolic derangements, inhibiting all NAD+ requiring steps.
- Lactic Acidosis: Pyruvate is diverted to lactate ($Pyruvate + NADH \leftrightarrow Lactate + NAD^+$), causing metabolic acidosis.
- Fasting Hypoglycemia: Oxaloacetate is shunted to malate, inhibiting its use for gluconeogenesis.
- Ketoacidosis: TCA cycle stalls from ↑ NADH, shunting excess acetyl-CoA towards ketone body production.
- Hepatosteatosis: ↑ Glycerol-3-P (from DHAP) and fatty acids promote triglyceride synthesis and accumulation in the liver.
⭐ The high NADH/NAD+ ratio inhibits gluconeogenesis (by shunting pyruvate to lactate and oxaloacetate to malate), leading to fasting hypoglycemia.
Clinical Pharmacology - Drugs & Genes
- Fomepizole: Inhibits alcohol dehydrogenase (ADH).
- Use: Antidote for methanol or ethylene glycol poisoning.
- Disulfiram: Inhibits aldehyde dehydrogenase (ALDH).
- Use: Aversive therapy for alcohol use disorder; causes acetaldehyde buildup.
- ALDH2 Gene Deficiency: Common in East Asian populations (~40%).
- Leads to “Asian flush” (tachycardia, facial flushing, nausea) after alcohol consumption due to ↑ acetaldehyde.
⭐ Disulfiram works by inhibiting Aldehyde Dehydrogenase (ALDH), causing an accumulation of toxic acetaldehyde and leading to unpleasant symptoms like flushing, tachycardia, and nausea.
High‑Yield Points - ⚡ Biggest Takeaways
- Ethanol metabolism occurs in the liver via Alcohol Dehydrogenase (ADH) and the Microsomal Ethanol-Oxidizing System (MEOS).
- The process generates excess NADH, leading to an increased NADH/NAD+ ratio.
- This high ratio inhibits gluconeogenesis (causing fasting hypoglycemia) and β-oxidation (causing hepatic steatosis).
- Fomepizole blocks ADH and is the antidote for methanol or ethylene glycol poisoning.
- Disulfiram inhibits ALDH, causing accumulation of toxic acetaldehyde.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

