Genetic Counseling - The Family Compass
- Empowers families with information for making informed decisions about management and family planning.
- Core components:
- Discussing disease natural history, prognosis, and inheritance patterns (most are autosomal recessive).
- Calculating recurrence risk for future pregnancies.
- Genetic Testing Options:
- Carrier screening: To identify asymptomatic carriers in the family.
- Prenatal diagnosis: Via chorionic villus sampling (CVS) or amniocentesis.
- Newborn screening: For early diagnosis and intervention.
- Outlines available management like enzyme replacement therapy (ERT) and supportive care.

⭐ For autosomal recessive LSDs, if both parents are carriers, each pregnancy has a 25% risk of an affected child, a 50% risk of a carrier child, and a 25% risk of an unaffected, non-carrier child.
Inheritance Patterns - It's All Relative
- Majority: Most lysosomal storage diseases (LSDs) are inherited in an autosomal recessive (AR) pattern.
- Parents are typically asymptomatic carriers.
- Recurrence risk for offspring is 25%.
- X-Linked Exceptions: Two major LSDs are X-linked recessive.
- Fabry disease (GLA gene)
- Hunter syndrome (MPS II) (IDS gene)
- 📌 Mnemonic: "Hunters Find Xes": Hunter syndrome & Fabry disease are X-linked.
⭐ Fabry disease shows significant clinical variability in heterozygous females (carriers), ranging from asymptomatic to a severe classic phenotype. This is due to random X-inactivation (lyonization).
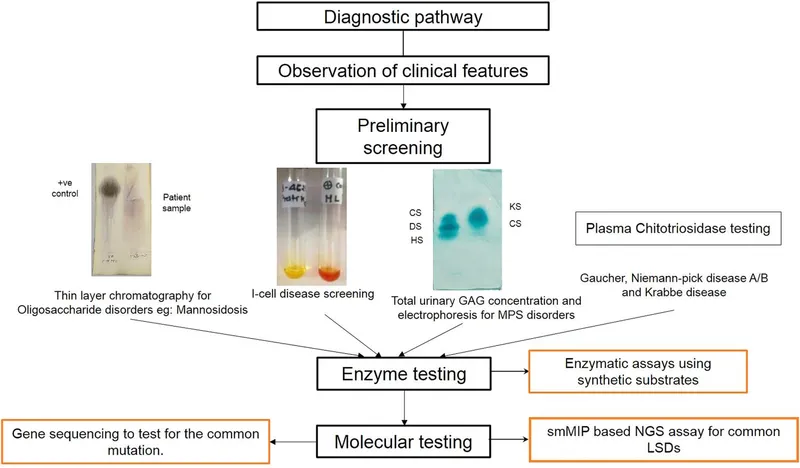
Diagnostic Testing - Decoding the Blueprint
-
Enzyme Activity Assays: The primary diagnostic step for most LSDs.
- Measures deficient enzyme activity in patient samples.
- Common samples: Leukocytes, cultured skin fibroblasts, plasma, or dried blood spots.
- Confirms the functional defect before genetic analysis.
-
Molecular Genetic Testing: The definitive confirmation.
- Identifies specific pathogenic mutations in the associated gene.
- Crucial for:
- Confirming diagnosis, especially in ambiguous cases.
- Carrier detection in at-risk family members.
- Prenatal diagnosis (via amniocentesis or CVS).
-
Newborn Screening (NBS):
- Available for select LSDs (e.g., Pompe, Krabbe, Fabry disease).
⭐ Pseudodeficiency Alert: Low enzyme activity on an assay doesn't always equate to clinical disease. Benign "pseudodeficiency" alleles can exist, making molecular genetic testing essential to confirm a true pathogenic mutation and prevent misdiagnosis.
Counseling & Management - The Support System
-
Genetic Counseling: Essential for families to understand inheritance, recurrence risk, and make informed reproductive decisions.
- Most LSDs are autosomal recessive (exceptions: Fabry, Hunter, Danon are X-linked).
- Options include carrier screening, prenatal diagnosis (CVS, amniocentesis), and preimplantation genetic testing (PGT).
-
Multidisciplinary Care: A team-based approach is critical for managing complex, multi-systemic symptoms.
- Involves specialists in genetics, neurology, cardiology, and rehabilitation medicine.
- Supportive therapies (physical, occupational, speech) are vital for maintaining function.
⭐ Enzyme replacement therapy (ERT) is a cornerstone treatment for many LSDs, but its inability to cross the blood-brain barrier limits efficacy for CNS manifestations.

- Most lysosomal storage diseases (LSDs) are autosomal recessive, with key exceptions like Fabry disease (X-linked) and Hunter syndrome (X-linked).
- Genetic counseling is essential to explain inheritance patterns, recurrence risks (typically 25% for AR), and the importance of carrier screening for family members.
- Prenatal diagnosis is possible through amniocentesis or chorionic villus sampling (CVS) by measuring enzyme activity or genetic testing.
- Newborn screening is expanding for treatable LSDs like Pompe and Gaucher disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

