Lipoprotein Structure - Greasy Little Packets
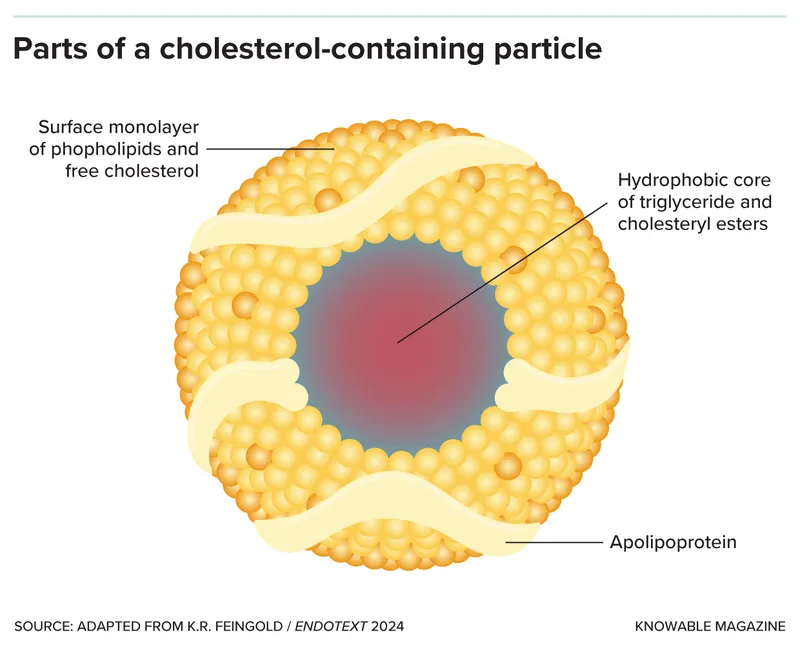
- General Structure: Spherical particles composed of a hydrophobic core and a hydrophilic shell, allowing transport of lipids in aqueous plasma.
- Core: Triglycerides & cholesteryl esters (nonpolar).
- Shell: Apolipoproteins, phospholipids, & free cholesterol (amphipathic).
- Apolipoproteins: Key surface proteins that function as enzyme cofactors (e.g., C-II for LPL) and receptor ligands (e.g., B-100 for LDL-R).
- Classification (by ↑ density): Chylomicron → VLDL → IDL → LDL → HDL.
⭐ LDL ("Lousy" cholesterol) is the primary transporter of cholesterol to peripheral tissues. Elevated levels are a major risk factor for atherosclerosis.
Exogenous Pathway - The Gut-to-Guts Route
📌 Mnemonic: 'Exogenous' = 'Eats' (dietary fat).
- Chylomicrons: Formed in intestines with ApoB-48 to transport dietary TGs/cholesterol.
- Maturation: HDL donates ApoC-II (LPL activator) & ApoE (hepatic uptake).
- Clearance: LPL releases FFAs to periphery; remnants cleared by liver via ApoE.
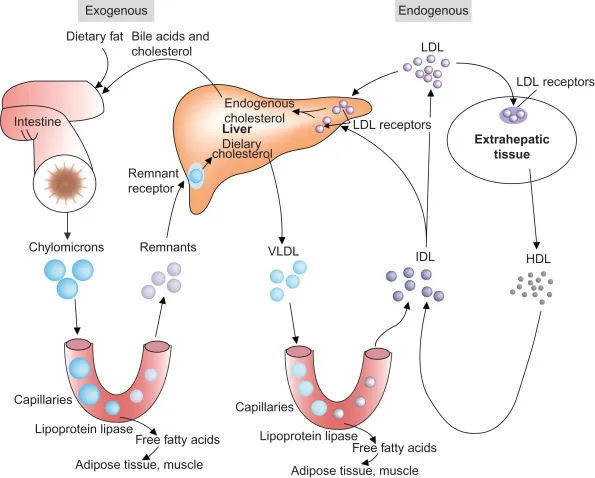
⭐ Deficiency in LPL or ApoC-II causes Type 1 hyperlipoproteinemia (Familial Chylomicronemia Syndrome), presenting with acute pancreatitis.
Endogenous Pathway - Liver's Delivery Service
- Origin: Liver synthesizes VLDL particles, which contain endogenous triglycerides and cholesterol, tagged with ApoB-100.
- Metabolism:
- VLDL is released into circulation.
- Lipoprotein Lipase (LPL) on endothelial cells hydrolyzes triglycerides, transforming VLDL → IDL.
- Hepatic Lipase (HL) in the liver removes more triglycerides, converting IDL → LDL.
- Destination: LDL delivers cholesterol to peripheral tissues and the liver via LDL-receptor binding (ApoB-100 mediated).
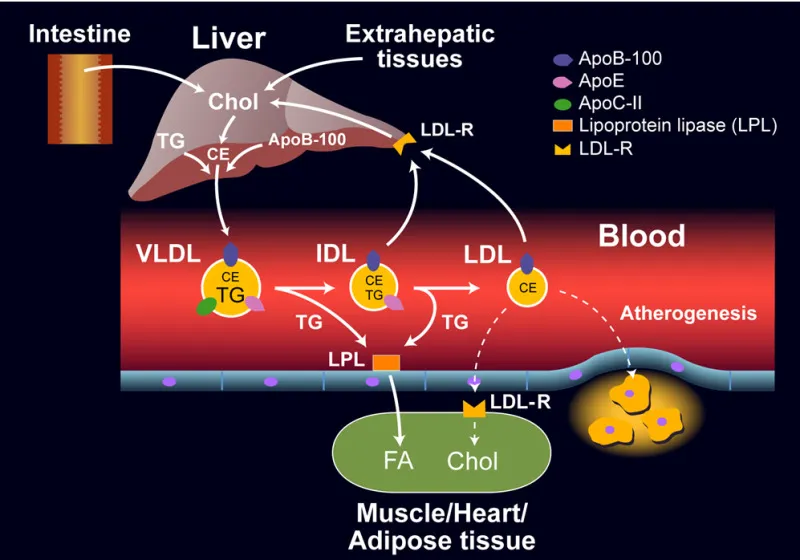
⭐ In Familial Hypercholesterolemia, defective LDL receptors (or ApoB-100) prevent LDL uptake, causing markedly elevated plasma LDL and premature cardiovascular disease.
Reverse Transport - The Cleanup Crew
- Nascent HDL: Secreted from the liver and intestine, containing ApoA-I. It extracts cholesterol from peripheral tissues.
- LCAT: Lecithin-cholesterol acyltransferase, activated by ApoA-I, esterifies cholesterol. This traps it within the HDL core, forming mature HDL.
- CETP: Cholesteryl ester transfer protein mediates the transfer of these cholesterol esters to VLDL/IDL in exchange for triglycerides.
⭐ Tangier Disease: A deficiency in the ABCA1 transporter prevents cholesterol loading onto nascent HDL. This leads to very low HDL levels, peripheral neuropathy, and pathognomonic orange-colored tonsils.

Dyslipidemias - When Lipids Go Rogue
Familial dyslipidemias are genetic disorders of lipoprotein metabolism. The Fredrickson classification categorizes them based on specific lipoprotein elevations.
| Type | Defect | ↑ Lipoprotein | Key Clinical Finding |
|---|---|---|---|
| I | LPL / ApoC-II | Chylomicrons | Acute pancreatitis, eruptive xanthomas |
| IIa | LDL-R | LDL | Tendon xanthomas, premature CAD |
| IIb | ↑ ApoB | LDL, VLDL | Increased risk of CAD |
| III | ApoE | IDL (Remnants) | Palmar/tuboeruptive xanthomas |
| IV | ↑ VLDL prod. | VLDL | Associated with insulin resistance |
High‑Yield Points - ⚡ Biggest Takeaways
- Chylomicrons transport dietary triglycerides from the intestine; VLDL transports hepatic triglycerides from the liver.
- Lipoprotein lipase (LPL), activated by ApoC-II, degrades triglycerides in chylomicrons and VLDL.
- LDL is the primary carrier of cholesterol to peripheral tissues; elevated levels are atherogenic.
- HDL facilitates reverse cholesterol transport from the periphery to the liver.
- ApoB-100 is the ligand for the LDL receptor; ApoA-I activates LCAT for HDL maturation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

