Arachidonic Acid Metabolism - The Inflammatory Cascade
- Source: Arachidonic Acid (AA) is released from membrane phospholipids by Phospholipase A₂ (inhibited by corticosteroids).
- Pathways: AA is metabolized via two main pathways: Cyclooxygenase (COX) and Lipooxygenase (LOX).
- COX Pathway (Prostanoids)
- Prostaglandins (PGI₂, PGE₂): ↑ Vascular permeability & vasodilation, pain, fever.
- Thromboxane A₂ (TXA₂): ↑ Platelet aggregation & vasoconstriction.
- Inhibited by NSAIDs, Celecoxib.
- LOX Pathway (Leukotrienes)
- LTB₄: Neutrophil chemotaxis. (📌 Brings neutrophils to site).
- Cysteinyl-LTs (LTC₄, LTD₄, LTE₄): Bronchoconstriction, ↑ vascular permeability.
- Inhibited by Zileuton, Montelukast.
⭐ Aspirin irreversibly inhibits COX-1 and COX-2 via covalent acetylation, unlike other NSAIDs which are reversible inhibitors.
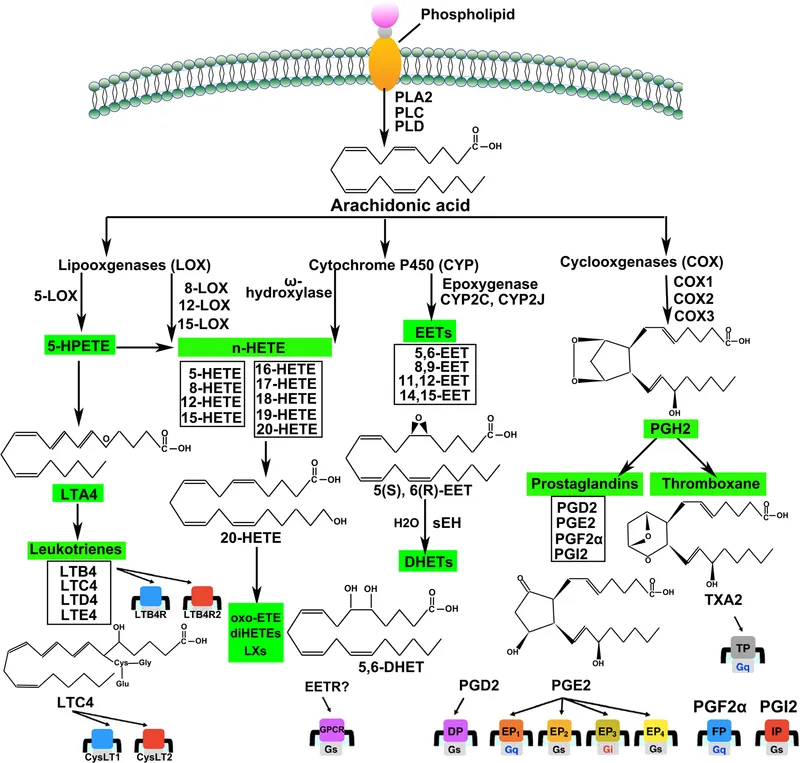
Cyclooxygenase (COX) Pathway - Prostanoid Production

- Precursor: Arachidonic Acid, released from cell membranes via Phospholipase A₂.
- Key Enzyme: Cyclooxygenase (COX) converts Arachidonic Acid to Prostaglandin H₂ (PGH₂).
- COX-1 (Constitutive): "Housekeeping" roles like gastric protection, renal blood flow, and platelet aggregation.
- COX-2 (Inducible): Upregulated by inflammatory stimuli to produce prostaglandins that mediate pain, fever, and inflammation.
- Products from PGH₂:
- Prostacyclin (PGI₂): Causes vasodilation and inhibits platelet aggregation.
- Thromboxane A₂ (TXA₂): Causes vasoconstriction and promotes platelet aggregation. 📌 Thromboxane Aggregates.
- Prostaglandins (PGE₂, PGD₂): Mediate inflammation, pain, and fever. PGE₂ maintains a patent ductus arteriosus (PDA).
⭐ Aspirin causes irreversible inhibition of COX-1 in platelets, thus blocking TXA₂ synthesis for the entire platelet lifespan (~7-10 days).
Lipoxygenase (LOX) Pathway - Leukotriene Lineage
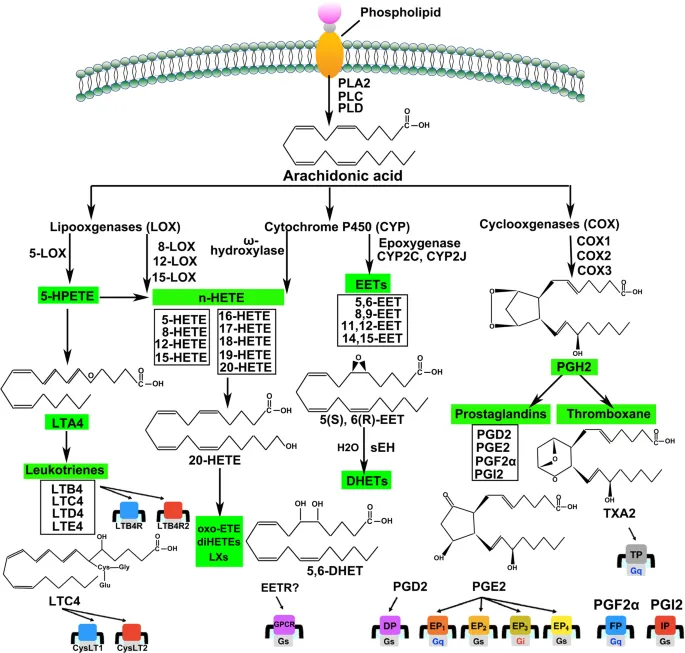
- Initiating Enzyme: 5-Lipoxygenase (5-LOX) acts on Arachidonic Acid.
- Pathway Inhibitor: Zileuton blocks 5-LOX.
- Key Products & Functions:
- LTB4: Neutrophil chemotaxis, adhesion, and activation. 📌 LTB4 is for Neutrophils (Brings them 4ward).
- Cysteinyl-LTs (LTC4, LTD4, LTE4):
- Intense bronchoconstriction (asthma).
- ↑ Vascular permeability & vasoconstriction.
⭐ Cysteinyl-leukotriene receptor antagonists (e.g., Montelukast, Zafirlukast) are mainstays in asthma therapy, specifically blocking the effects of LTC4, D4, and E4 on bronchial smooth muscle.
Pharmacologic Modulation - Taming the Flames
- Corticosteroids (e.g., Prednisone): Inhibit Phospholipase A₂, blocking the entire cascade upstream. Halts all prostaglandin and leukotriene production.
- NSAIDs: Inhibit cyclooxygenase (COX) enzymes.
- Non-selective (Aspirin, Ibuprofen): Block both COX-1 and COX-2.
- COX-2 Selective (Celecoxib): Target inflammation with less risk of gastric ulcers.
- Leukotriene Pathway Inhibitors: Primarily for asthma & allergic rhinitis.
- Zileuton: Inhibits 5-Lipoxygenase enzyme.
- Montelukast, Zafirlukast: Block CysLT1 leukotriene receptors.
⭐ Aspirin irreversibly acetylates COX-1 and COX-2. Its effect on platelets is permanent for the platelet's lifespan (~7-10 days), crucial for its cardioprotective role.
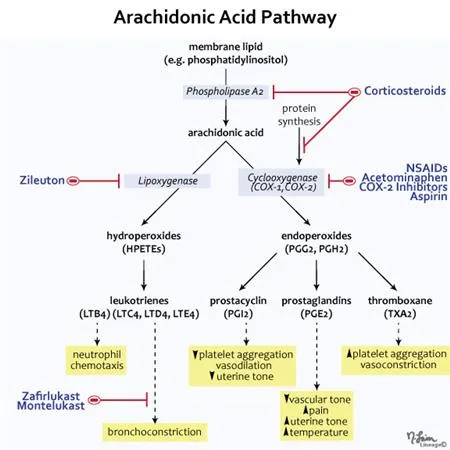
High‑Yield Points - ⚡ Biggest Takeaways
- Eicosanoids are signaling molecules derived from arachidonic acid, released from membranes by Phospholipase A2.
- The cyclooxygenase (COX) pathway produces prostaglandins (inflammation, gastric protection) and thromboxanes (platelet aggregation).
- The lipoxygenase (LOX) pathway yields leukotrienes (bronchoconstriction, chemotaxis) and anti-inflammatory lipoxins.
- NSAIDs inhibit COX enzymes; corticosteroids block Phospholipase A2 upstream, hitting both pathways.
- Aspirin causes irreversible COX inhibition, crucial for its antiplatelet effect.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

