Pathophysiology - Sugar Stuck Inside
- Primary Defect: Deficiency of Glucose-6-phosphatase in the liver, kidneys, and intestinal mucosa.
- Metabolic Block: The final step of gluconeogenesis & glycogenolysis is blocked: $G6P \nrightarrow Glucose$.
- Consequences: Glucose-6-phosphate gets "stuck" inside hepatocytes, leading to:
- Severe fasting hypoglycemia.
- G6P accumulation and shunting into other pathways.
⭐ Severe fasting hypoglycemia is the hallmark, often presenting within the first few months of life with seizures.

Clinical Features - Big Liver, Hangry Baby
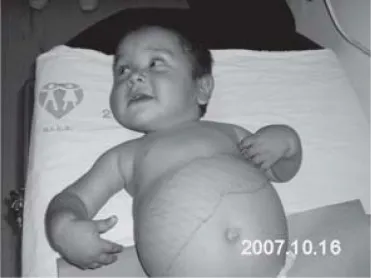
- Presentation (3-6 months): Doll-like facies (fat cheeks, thin extremities), short stature, and a protuberant abdomen from massive hepatomegaly (glycogen buildup).
- Severe Fasting Hypoglycemia: Central, life-threatening feature. Leads to irritability, seizures, and lethargy if feedings are spaced.
- Blood glucose often < 60 mg/dL.
- Key Metabolic Derangements:
- ↑ Lactic acidosis (shunting of G6P).
- ↑ Hyperuricemia → Gout in adolescence/adulthood.
- ↑ Hyperlipidemia (milky/lipemic serum).
- Renal: Nephromegaly due to glycogen deposition, risking dysfunction over time.
- Hematologic: Impaired platelet function → bleeding tendency (e.g., epistaxis).
⭐ Patients often present with seizures due to profound hypoglycemia, a key feature distinguishing it from GSDs with milder hypoglycemia.
Diagnosis - The Proof is in the Labs
-
Blood & Urine Panel:
- ↓↓ Severe fasting hypoglycemia
- ↑↑ Lactic acidosis
- ↑↑ Hyperuricemia
- ↑↑ Hyperlipidemia (esp. triglycerides)
- Ketones are notably absent or low in urine/blood.
-
Diagnostic Flow:
⭐ Glucagon Challenge Test: A hallmark finding is the failure of blood glucose to rise after glucagon administration, coupled with a paradoxical, sharp increase in blood lactate levels. This confirms a block in the final steps of gluconeogenesis and glycogenolysis.
Management - The Cornstarch Cure
- Primary Goal: Maintain normoglycemia (blood glucose >70 mg/dL) to prevent acute crises and support normal growth.
- Dietary Regimen:
- Frequent daytime meals + continuous nocturnal glucose infusion (e.g., via NG tube) in infants.
- Uncooked Cornstarch: Administered every 4-6 hours; acts as a slow-release glucose source, bypassing the enzyme defect.
- Dietary Restrictions:
- Avoid fructose, sucrose, and galactose (lactose). These sugars are metabolized to glucose-6-phosphate, exacerbating intracellular accumulation.
- Pharmacotherapy:
- Allopurinol: To control hyperuricemia and prevent gout.
⭐ The core principle is providing a constant exogenous source of glucose, like uncooked cornstarch, to bypass the defective endogenous glucose production (both glycogenolysis and gluconeogenesis).
High‑Yield Points - ⚡ Biggest Takeaways
- Deficiency in glucose-6-phosphatase, the final step of gluconeogenesis & glycogenolysis.
- Presents at 3-4 months with severe fasting hypoglycemia, lactic acidosis, and seizures.
- Classic findings include a protuberant abdomen (massive hepatomegaly), doll-like facies, and thin extremities.
- Lab results show hyperuricemia, hyperlipidemia (↑ triglycerides), and ↑ blood lactate.
- Treatment involves frequent oral glucose/cornstarch and avoiding fructose and galactose.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

