Conducting Zone - The Air Superhighway

- Function: Warms, humidifies, and filters inspired air. Lined predominantly by respiratory epithelium (ciliated pseudostratified columnar) with mucus-producing goblet cells.
- Trachea & Bronchi:
- Supported by hyaline cartilage (C-rings in trachea, irregular plates in bronchi).
- Contain submucosal seromucous glands for mucus production.
- Bronchioles:
- Lack cartilage and glands; this is a key identifier.
- Feature a prominent circumferential layer of smooth muscle (muscularis mucosae).
- Epithelium transitions from ciliated columnar to simple cuboidal.
- Terminal Bronchioles:
- Final, smallest part of the conducting zone.
- Lined by simple cuboidal cells, including Club (Clara) cells which produce a surfactant component and act as stem cells.
⭐ Reid Index: The ratio of submucosal gland thickness to the bronchial wall thickness (measured from epithelium to cartilage). A normal index is < 0.4; it is characteristically increased in chronic bronchitis due to glandular hypertrophy.
Bronchioles & Club Cells - Tiny Tubes, Big Roles
-
Bronchioles: Airways <1 mm in diameter; transition from conducting to respiratory zones.
- Lack cartilage and submucosal glands.
- Lined by ciliated simple columnar to cuboidal epithelium.
- Prominent smooth muscle layer regulates airflow.
- Terminal bronchioles: Final segment of the conducting zone.
- Respiratory bronchioles: Have alveoli in their walls; begin the respiratory zone.
-
Club Cells (formerly Clara Cells): Non-ciliated, dome-shaped cells in terminal/respiratory bronchioles.
- Functions:
- Secretion: Surfactant components & Club Cell Secretory Protein (CCSP/CC16).
- Detoxification: Degrade inhaled toxins via cytochrome P450 enzymes.
- Progenitor cells: Regenerate bronchiolar epithelium after injury.
- Functions:
⭐ Inhaled toxins can deplete Club cells, impairing detoxification and repair mechanisms in the small airways, a key pathological feature in diseases like COPD.

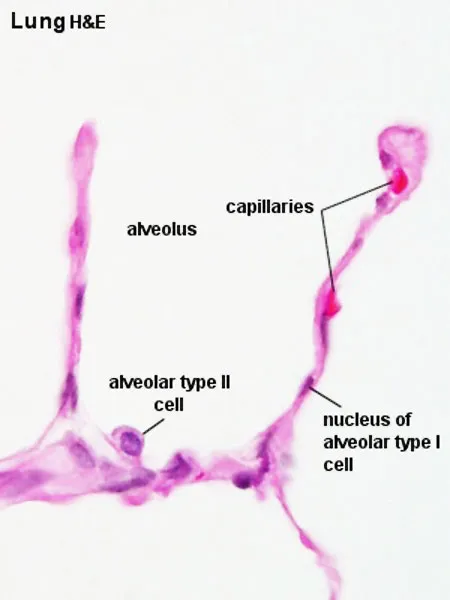
Alveoli - The Gas Exchange Hub
- Primary site of gas exchange; thin-walled, sac-like structures at the end of respiratory bronchioles.
- Cellular Components:
- Type I Pneumocytes (95%): Simple squamous epithelium. Extremely thin for optimal gas diffusion. Form the alveolar side of the blood-air barrier.
- Type II Pneumocytes (5%): Cuboidal cells.
- Synthesize & secrete pulmonary surfactant (dipalmitoylphosphatidylcholine), which ↓ surface tension.
- Act as stem cells, regenerating both Type I and Type II cells.
- Alveolar Macrophages (Dust Cells): Phagocytose inhaled particles & pathogens. In heart failure, they become hemosiderin-laden "heart failure cells".
- Pores of Kohn: Allow collateral ventilation between adjacent alveoli, preventing atelectasis.
⭐ Neonatal Respiratory Distress Syndrome (NRDS): Occurs in premature infants (< 35 weeks gestation) due to insufficient surfactant production. Leads to widespread alveolar collapse, requiring artificial surfactant and respiratory support.
High‑Yield Points - ⚡ Biggest Takeaways
- Respiratory epithelium transitions from pseudostratified ciliated columnar with goblet cells to simple cuboidal in terminal bronchioles.
- Bronchioles are defined by a lack of cartilage and glands and the presence of Club cells (secretory, protective).
- Type I pneumocytes are squamous cells covering 95% of the alveolar surface for gas exchange.
- Type II pneumocytes are cuboidal, produce pulmonary surfactant, and act as stem cells for the alveolar lining.
- Alveolar macrophages (dust cells) clear debris; they become hemosiderin-laden in heart failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

