Ovary - The Follicle Factory
- Anatomy: Simple cuboidal germinal epithelium covers the tunica albuginea. The cortex contains follicles; the medulla has vessels & nerves.
- Folliculogenesis Stages:
- Primordial: Primary oocyte arrested in prophase I, surrounded by a single layer of squamous follicular cells.
- Primary: Follicular cells become cuboidal (granulosa cells); zona pellucida appears.
- Secondary (Antral): Fluid-filled antrum forms. Theca interna (androgen-secreting) and externa (fibrous) layers develop.
- Graafian (Mature): Large, dominant follicle ready for ovulation.

⭐ Theca interna cells, stimulated by LH, produce androgens. Granulosa cells, stimulated by FSH, convert these androgens to estrogen via aromatase.
Uterine Tube & Uterus - Womb with a View
-
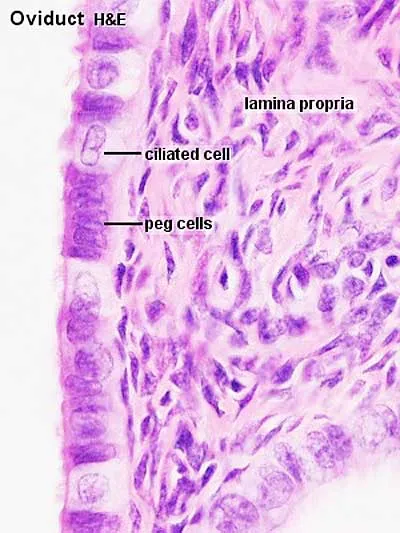
Uterine (Fallopian) Tube: Simple columnar epithelium.
- Ciliated cells: Beat synchronously towards the uterus.
- Peg (secretory) cells: Nourish the ovum/embryo.
- Muscularis externa creates peristaltic waves.
-
Uterus: Wall has three layers: endometrium, myometrium, perimetrium.
- Endometrium:
- Stratum functionalis: Proliferates and degenerates monthly; shed during menses.
- Stratum basalis: Regenerates the functionalis layer.
- Myometrium: Thick smooth muscle that undergoes hypertrophy and hyperplasia during pregnancy.
- Endometrium:
⭐ The ampulla of the uterine tube is the most common site of both fertilization and ectopic pregnancy.
Menstrual Cycle - Hormonal Tide Ride

- Follicular Phase (Estrogen-dominant): FSH stimulates follicular growth. Rising estrogen builds the endometrium (proliferative phase).
- Ovulation (~Day 14): Peak estrogen triggers a massive LH surge, causing follicle rupture.
- Luteal Phase (Progesterone-dominant): Corpus luteum produces progesterone, creating a secretory endometrium ready for implantation.
- Menses: Without hCG, the corpus luteum fails, progesterone drops, and the endometrium sheds.
⭐ The LH surge is the key trigger for ovulation, occurring 24-36 hours prior. Clinically, ovulation can be induced by administering hCG, which mimics LH action.
Cervix & Vagina - Gateway Guardians

- Cervix: A dual-epithelium gateway.
- Ectocervix: Protective non-keratinized stratified squamous epithelium.
- Endocervix: Secretory simple columnar epithelium.
- Transformation Zone: Squamocolumnar junction (SCJ); a dynamic area of metaplasia.
- Vagina: Resilient and acidic.
- Epithelium: Non-keratinized stratified squamous, rich in glycogen.
- Lactobacilli: Convert glycogen to lactic acid, creating a low pH environment hostile to pathogens.
⭐ The transformation zone is the most common site for Human Papillomavirus (HPV) infection and subsequent cervical intraepithelial neoplasia (CIN).
High‑Yield Points - ⚡ Biggest Takeaways
- The ovary's surface is covered by simple cuboidal germinal epithelium, a common source of tumors.
- The cervical transformation zone is a key site for HPV, marking the shift from simple columnar to stratified squamous epithelium.
- Uterine tubes contain ciliated columnar cells for transport and nutritive peg cells.
- The secretory phase endometrium shows coiled, saw-toothed glands due to progesterone.
- The corpus luteum features large, eosinophilic granulosa lutein cells.
- The vagina is lined by non-keratinized stratified squamous epithelium that stores glycogen.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

