Heart & Vessel Walls - Layer by Layer
- Heart Wall: Endocardium → Myocardium → Epicardium (visceral pericardium).
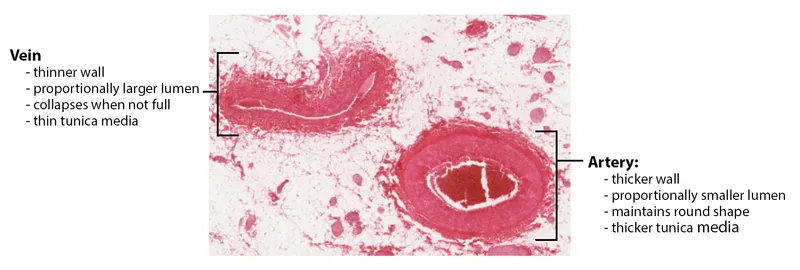
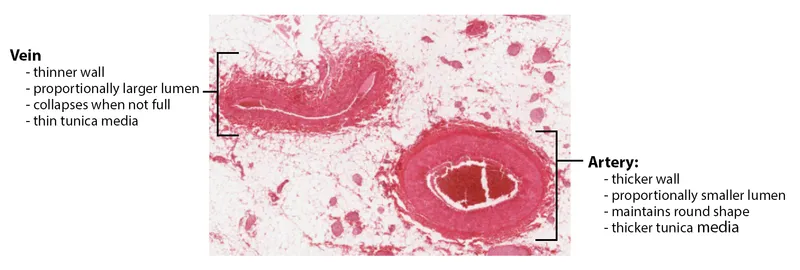
- Vessel Wall: Tunica Intima → Tunica Media → Tunica Adventitia.
- 📌 Mnemonic: In My Aorta (Intima, Media, Adventitia).
| Layer | Heart Component | Vessel Component | Key Features |
|---|---|---|---|
| Inner | Endocardium | Tunica Intima | Simple squamous endothelium. Site of atherosclerosis. |
| Middle | Myocardium | Tunica Media | Muscle layer. Thickest in arteries & ventricles. |
| Outer | Epicardium | Tunica Adventitia | Connective tissue, nerves, & vessels (vasa vasorum). |
Cardiac Conduction - The Sparky Bits
- Sinoatrial (SA) Node: The heart's primary pacemaker, located in the right atrium. Initiates impulse.
- Atrioventricular (AV) Node: Located at the interatrial septum. Creates a crucial ~100 ms delay.
- Bundle of His: Transmits signal from AV node to interventricular septum.
- Right & Left Bundle Branches: Carry impulse towards the apex.
- Purkinje Fibers: Large, specialized cells with abundant glycogen and mitochondria; distribute impulse rapidly through ventricles for coordinated contraction.
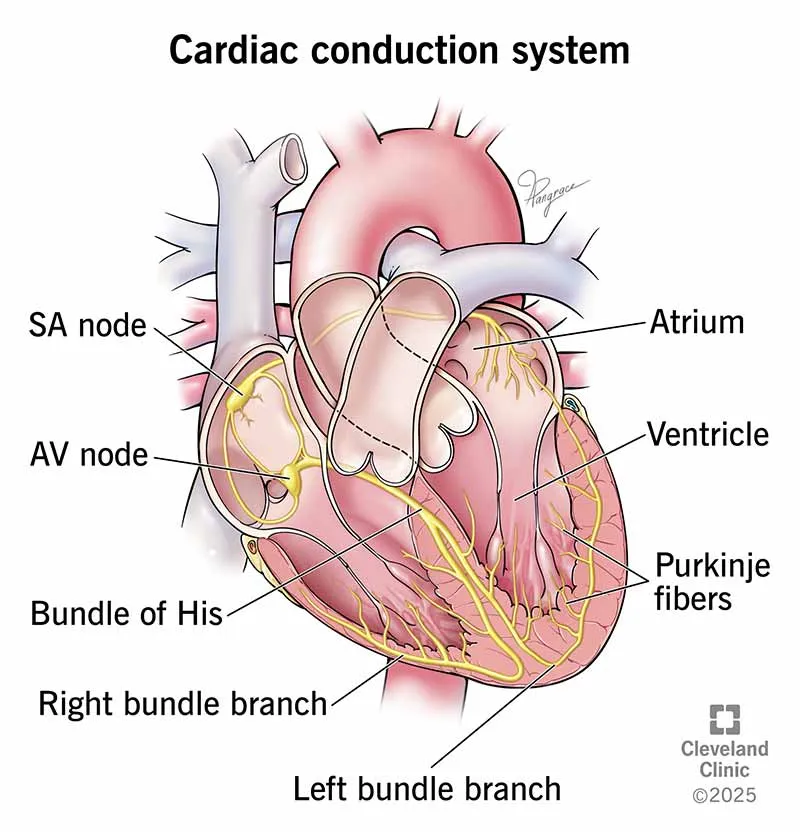
⭐ High-Yield: The AV nodal delay is essential. It allows time for atrial contraction (atrial kick) to complete, ensuring ventricles are adequately filled before they contract.
Valves & Vessels - Gates and Pipes
-
Heart Valves
- Avascular structures composed of layered fibro-elastic tissue.
- Layers (from outflow to inflow): Fibrosa (dense collagen), Spongiosa (loose CT, shock absorber), and Ventricularis/Atrialis (elastin).
-
Blood Vessels
- Three layers (tunics): Intima, Media, and Adventitia.
- Arteries: Thick, muscular/elastic media to handle high pressure.
- Veins: Thinner walls, larger lumens, and may contain valves to prevent backflow.
- Arterioles: Primary site of peripheral resistance.
⭐ The vasa vasorum ("vessels of the vessels") are small arteries that supply blood to the outer walls (tunica adventitia & outer media) of large vessels like the aorta.
Clinical Histology - When Tissues Fail
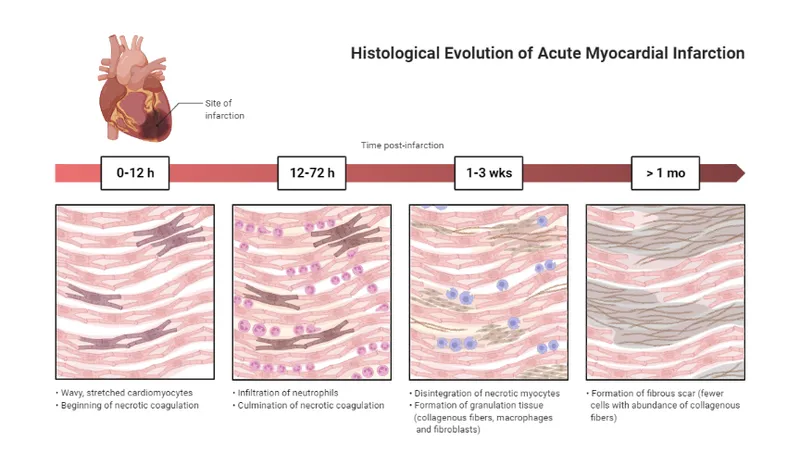
- Myocardial Infarction (MI): Progression of changes.
- <24 hrs: Coagulation necrosis, wavy fibers, edema.
- 1-3 days: Dense neutrophilic infiltrate.
- 4-7 days: Macrophage infiltration begins.
- >2 wks: Granulation tissue forms, replaced by a fibrous scar.
- Myocarditis: Diffuse lymphocytic and mononuclear cell infiltrate in the myocardium.
- Atherosclerosis: Fibrous cap covers a necrotic core with cholesterol clefts and foam cells (lipid-laden macrophages).
- Rheumatic Heart Disease: Pathognomonic Aschoff bodies (foci of fibrinoid necrosis) with Anitschkow "caterpillar" cells.
⭐ In MI, contraction band necrosis is a key feature of reperfusion injury, seen as intensely eosinophilic transverse bands in myocytes.
High‑Yield Points - ⚡ Biggest Takeaways
- Arteries have a thick tunica media; veins possess a larger tunica externa and may contain valves.
- Myocardium contains cardiac myocytes joined by intercalated discs, ensuring functional syncytium.
- Purkinje fibers are large, pale cells rich in glycogen, specialized for rapid impulse conduction.
- Atherosclerosis is a disease of the tunica intima, initiated by endothelial dysfunction and involving foam cells.
- The entire cardiovascular system is lined by a simple squamous endothelium.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

