Lymphatic System Review - The Body's Sewer System
- Core Function: A one-way drainage network returning interstitial fluid (lymph) and proteins to the venous circulation. Essential for fluid balance, immune cell trafficking, and chylomicron transport from the gut.
- Driving Force: Primarily driven by intrinsic lymphatic vessel contraction and surrounding skeletal muscle pump action.
⭐ High-Yield: Lymphedema is a protein-rich edema. This high protein content incites chronic inflammation, leading to subcutaneous fibrosis and adipose tissue deposition, which is why it often becomes non-pitting over time.
Lymphedema Defined - When the Drains Clog
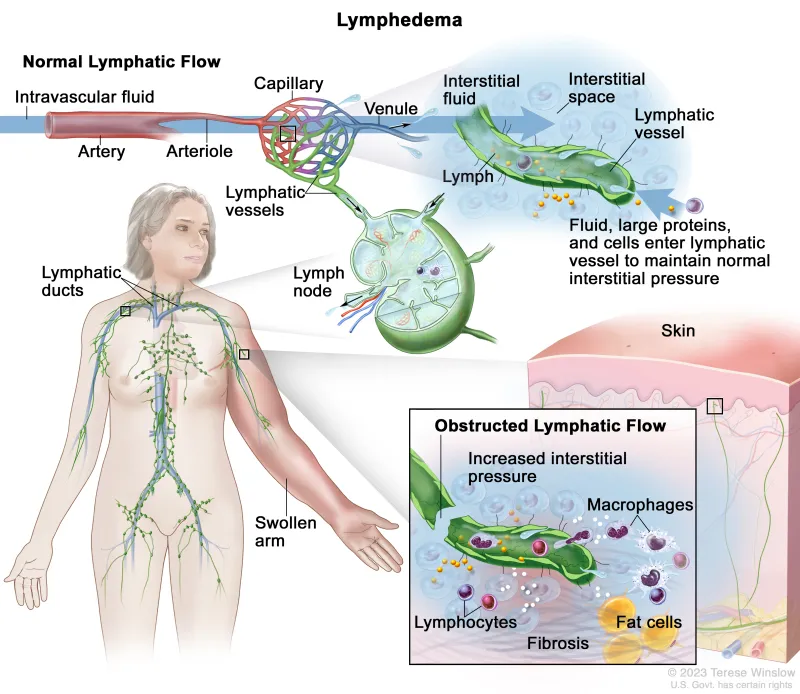
- Core Defect: Imbalance between lymphatic load & transport capacity, leading to accumulation of protein-rich interstitial fluid.
- Pathophysiology: Stagnant lymph proteins trigger chronic inflammation, stimulating fibroblasts and adipocytes.
- Leads to progressive subcutaneous fibrosis and adipose tissue deposition.
- Results in non-pitting edema over time and ↑ risk of cellulitis.
⭐ High-Yield: Chronic lymphedema is characteristically non-pitting due to significant subcutaneous protein deposition and fibrosis. A positive Stemmer sign (inability to pinch the skin at the base of the second toe) is pathognomonic.
Pathophysiology Cascade - The Protein Party Crash
- Initial Stage: Lymphatic obstruction leads to accumulation of protein-rich interstitial fluid, resulting in soft, pitting edema.
- Chronic Stage: Stagnant, high-protein fluid incites a chronic inflammatory response.
- Macrophages release cytokines and growth factors.
- Fibroblasts and adipocytes are stimulated.
- Irreversible Changes: Progressive fibrosis (collagen) and adipose tissue deposition occur.
- Tissue becomes hard, indurated, and non-pitting (brawny edema).
- ↑ Risk of cellulitis & lymphangitis.
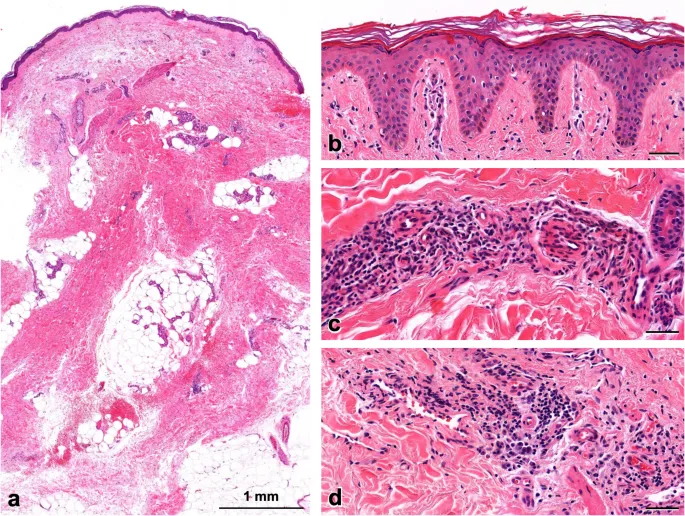
⭐ Stewart-Treves Syndrome: A rare but classic complication of chronic lymphedema (e.g., post-mastectomy) is lymphangiosarcoma, an aggressive cutaneous angiosarcoma.
Clinical Presentation & Staging - Spotting the Swelling

- Presentation: Insidious onset of painless, progressive swelling.
- Early stage: Soft, pitting edema that resolves with limb elevation.
- Late stage: Firm, non-pitting (brawny) edema due to fibrosis and adipose tissue deposition.
- Key Sign:
- Positive Stemmer's sign: Inability to pinch or tent the skin on the dorsum of the second toe (or finger).
- ISL Staging (0-3):
- Stage 0: Latent/subclinical; impaired transport, no visible swelling.
- Stage 1: Reversible; pitting edema, resolves with elevation.
- Stage 2: Spontaneously irreversible; non-pitting edema, fibrosis present.
- Stage 3: Lymphostatic elephantiasis; significant skin changes (e.g., papillomas, hyperkeratosis).
⭐ Chronic lymphedema is a major risk factor for Stewart-Treves syndrome, a rare but aggressive cutaneous angiosarcoma. Look for a new purple nodule or plaque on the affected limb.
High‑Yield Points - ⚡ Biggest Takeaways
- Lymphedema is the accumulation of protein-rich interstitial fluid from lymphatic system failure.
- Primary lymphedema arises from congenital abnormalities like lymphatic aplasia or hypoplasia (e.g., Milroy disease).
- Secondary lymphedema follows lymphatic obstruction or disruption, commonly from surgery, radiation, or tumors.
- Worldwide, the most common cause is filariasis (Wuchereria bancrofti).
- Chronic cases progress to non-pitting edema with subcutaneous fibrosis and hyperkeratosis.
- Complications include recurrent cellulitis and lymphangiosarcoma (Stewart-Treves syndrome).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

