Angiography 101 - The Vessel Roadmap
- Definition: An invasive diagnostic procedure using iodinated contrast and fluoroscopy (real-time X-ray) to visualize the lumen of blood vessels. Considered the gold standard for vessel mapping and intervention.
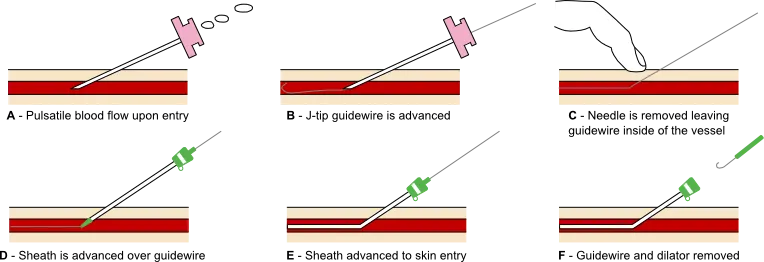
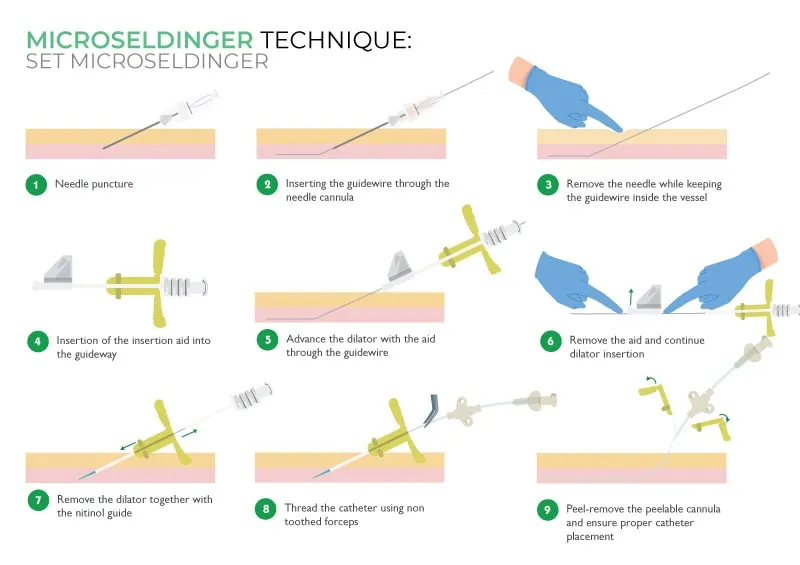
- Core Principle (Seldinger Technique): The foundational method for safe, percutaneous vascular access. A needle punctures the vessel, a guidewire is passed through the needle, the needle is removed, and a catheter is fed over the wire.
- Contrast Agents: Typically iodine-based solutions that are radiopaque (appear white on X-ray). ⚠️ Major risks include Contrast-Induced Nephropathy (CIN) and anaphylactoid reactions.
- Common Access Sites:
- Common Femoral Artery (CFA): Traditional choice, large diameter, easy to access.
- Radial Artery: Increasingly preferred due to ↑ patient comfort post-procedure and significantly ↓ risk of bleeding complications.
⭐ For patients with chronic kidney disease (CKD) or diabetes, the risk of Contrast-Induced Nephropathy (CIN) is significantly elevated. Pre-procedural IV hydration is the most effective preventative measure.
Technique & Access - Getting In
- Core Method: Modified Seldinger Technique
- 1. Needle Access: Puncture the target vessel with a hollow needle.
- 2. Guidewire: Pass a flexible guidewire through the needle into the vessel lumen.
- 3. Needle Removal: Withdraw the needle, leaving the guidewire in place.
- 4. Sheath/Catheter: Thread an introducer sheath or catheter over the guidewire.
- 5. Guidewire Removal: Remove the guidewire, leaving the sheath/catheter for access.
- Common Arterial Access Sites
- Common Femoral Artery (CFA): Traditional workhorse. Puncture below the inguinal ligament to avoid retroperitoneal hemorrhage.
- Radial Artery: Preferred for cardiac catheterization (↓bleeding, ↑patient comfort).
- Brachial Artery: Alternative; higher risk of nerve injury and thrombosis.
⭐ Pre-procedure Check: The Allen test must be performed to confirm adequate collateral circulation from the ulnar artery before radial artery cannulation. This mitigates the risk of hand ischemia.
Contrast & Complications - The Aftermath
-
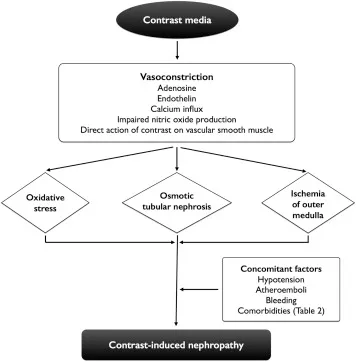
Contrast-Induced Nephropathy (CIN)
- ⚠️ Highest risk: Pre-existing CKD (eGFR <60), diabetes, dehydration, concurrent nephrotoxins.
- Pathophysiology: Direct tubular toxicity & renal vasoconstriction.
- Prevention: IV hydration (isotonic saline) is key. Consider N-acetylcysteine (antioxidant).
- Course: Serum creatinine (SCr) rises within 24-48 hrs, peaks at 3-5 days, resolves in 7-10 days.
-
Anaphylactoid/Allergic Reactions
- Acute hypersensitivity; not a true IgE-mediated allergy.
- Symptoms: Urticaria, angioedema, bronchospasm, shock.
- Management: Pre-medicate high-risk patients (prior reaction) with corticosteroids + H1/H2 blockers.
-
Gadolinium Contrast (MRA)
- ⚠️ Nephrogenic Systemic Fibrosis (NSF): Rare but severe fibrosing disease in patients with GFR <30 mL/min. Avoid gadolinium in this group.
⭐ Metformin & Contrast: Hold metformin on the day of contrast and for 48 hours after. Resume only after re-checking renal function. Risk of lactic acidosis if CIN develops.
High‑Yield Points - ⚡ Biggest Takeaways
- Seldinger technique is the fundamental method for percutaneous vascular access.
- Digital Subtraction Angiography (DSA) provides the clearest images by subtracting pre-contrast bone and soft tissue.
- Iodinated contrast is standard; be cautious of contrast-induced nephropathy (CIN), especially in patients with renal disease.
- The most common complication is an access site hematoma or bleeding.
- Gold standard for diagnosing conditions like vasculitis, aneurysms, and AVMs.
- Catheter shape is crucial; Judkins for coronaries, Simmons for tortuous vessels.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

