Pathophysiology - The Pressure Cooker
- Initiating Event: Trauma (e.g., fractures, crush injury), burns, or post-ischemic swelling leads to bleeding and edema within a closed fascial space.
- Vicious Cycle:
- The inelastic fascia prevents expansion, causing intracompartmental pressure (ICP) to rise (↑).
- As ICP exceeds venous and capillary pressure, vessels are compressed.
- This leads to ↓ venous outflow and ↓ arterial inflow, causing tissue hypoxia.
- Ischemia increases capillary permeability, worsening edema and further ↑ ICP.
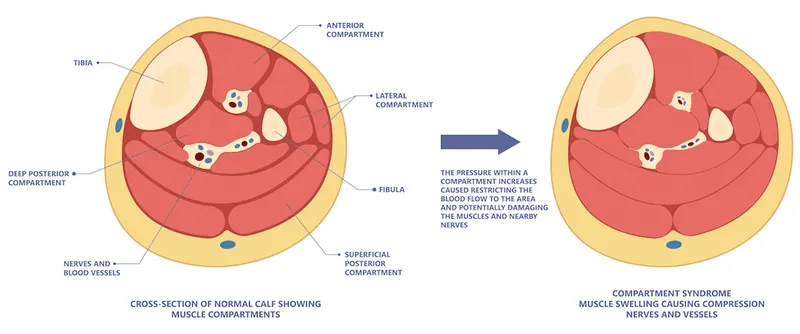
⭐ Fasciotomy is typically considered when the intracompartmental pressure rises to >30 mmHg, or when the difference between diastolic blood pressure and the compartment pressure is <20-30 mmHg.
Etiology - The Triggers
- ↓ Decreased Compartment Volume
- External Compression: Tight casts, splints, circumferential burns.
- Closure of fascial defects.
- ↑ Increased Compartment Content
- Bleeding or Edema:
- Fractures (esp. tibial shaft), crush injuries.
- Arterial injury, coagulopathy.
- Reperfusion injury after ischemia.
- Burns, nephrotic syndrome.
- Iatrogenic (e.g., infiltrated infusion).
- Other:
- Intense muscle exertion (exertional compartment syndrome).
- Bleeding or Edema:
⭐ Tibial fractures are the most frequent cause of acute compartment syndrome.
Clinical Features - The 6 P's
📌 Mnemonic: The 6 P's
- Pain: Severe, deep, and out of proportion to the apparent injury.
- Worsened by passive stretching of the affected muscles.
- Often the earliest and most sensitive symptom.
- Paresthesia: Numbness and tingling (pins-and-needles sensation) in the distribution of the affected nerve.
- Develops within 30 minutes to 2 hours of onset.
- Pallor: Pale and shiny skin, indicating poor perfusion.
- Poikilothermia: The affected limb is cool to the touch compared to the unaffected side.
- Paralysis / Paresis: Weakness or complete loss of motor function. A late and worrying sign.
- Pulselessness: Diminished or absent distal pulses.
- A very late finding, often heralding irreversible tissue damage.
⭐ Pain on passive stretch of the muscles in the affected compartment is considered the most sensitive and specific early physical finding for compartment syndrome.
Diagnosis & Complications - The Verdict & Damage
- Diagnosis of Exclusion: Primarily a clinical diagnosis; do not wait for all signs.
- Confirmatory Test: Direct needle manometry (e.g., Stryker device).
- Absolute intracompartmental pressure >30 mmHg.
- Delta pressure (ΔP) <20-30 mmHg is highly indicative.
- $ΔP = Diastolic BP - Intracompartmental Pressure$

- Complications (Time-sensitive):
- Irreversible muscle/nerve damage begins at 4-8 hours.
- Rhabdomyolysis: Leads to myoglobinuria & Acute Kidney Injury (AKI).
- Volkmann's Ischemic Contracture: Final stage of forearm compartment syndrome; claw-like deformity.
- Amputation.
⭐ Clinical Pearl: The classic "6 P's" are unreliable. Pulselessness and Pallor are very late findings, often signifying irreversible damage. Pain out of proportion is the earliest and most sensitive sign.
High‑Yield Points - ⚡ Biggest Takeaways
- Increased intracompartmental pressure in a non-expandable fascial space is the core pathology.
- Triggered by trauma (especially fractures), crush injuries, burns, or reperfusion injury.
- Elevated pressure first compresses veins, obstructing outflow and causing edema.
- This creates a vicious cycle, further increasing pressure and compromising capillary blood flow.
- Ultimately, arterial flow ceases, leading to tissue ischemia and infarction.
- Irreversible nerve and muscle damage occurs within 4-8 hours.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

