Blastocyst Formation - Getting Ready to Stick
- Day 4: Morula enters the uterine cavity.
- Uterine fluid penetrates the zona pellucida, forming the blastocoel (cavity).
- This reorganizes the morula into a blastocyst, composed of:
- Trophectoderm: Outer cell layer; forms the placenta.
- Embryoblast (Inner Cell Mass): Becomes the embryo.
- Day 5-6: "Hatching" occurs. The blastocyst sheds the zona pellucida, a necessary step for implantation. Trophoblastic proteases degrade the zona.
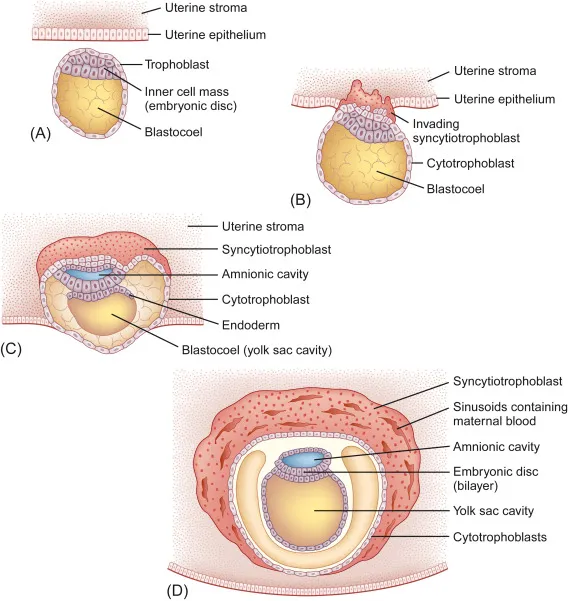
⭐ Initial adhesion of the blastocyst to the uterine wall is mediated by L-selectin on trophoblast cells binding to carbohydrate receptors on the uterine epithelium.
The Implantation Window - Perfect Timing
- A short receptive period in the mid-luteal phase, days 20-24 of a 28-day cycle (6-10 days post-ovulation).
- Driven by ↑ progesterone from the corpus luteum, priming the estrogen-prepared endometrium.
- Promotes secretion of glycogen-rich fluid.
- Induces stromal cell decidualization.
- Adhesion molecules are key for blastocyst capture:
- Trophoblast L-selectin binds endometrial carbohydrate ligands.
- Integrins (e.g., $α_vβ_3$) ensure stable attachment.
⭐ Pinopodes, progesterone-dependent endometrial protrusions, absorb uterine fluid, bringing the blastocyst closer to the endometrium for attachment.
Invasion & Decidualization - The Great Attachment
-
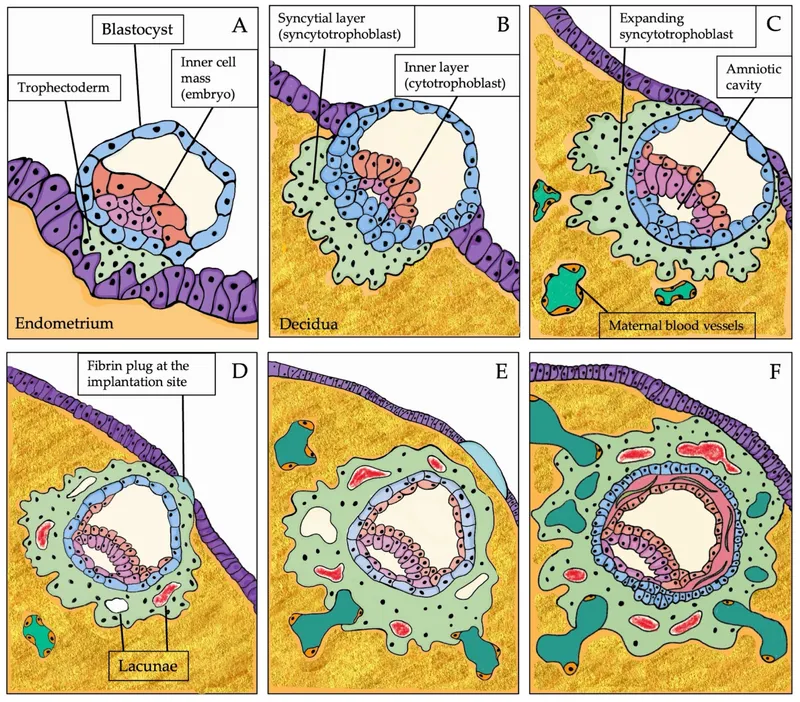
Syncytiotrophoblast Invasion:
- This aggressive, multinucleated outer layer secretes proteolytic enzymes (e.g., matrix metalloproteinases) to digest the endometrial stroma.
- It rapidly expands, forming lacunae that anastomose with maternal sinusoids, establishing primordial uteroplacental circulation.
- Secretes human chorionic gonadotropin (hCG).
-
Endometrial Decidualization:
- Under progesterone's influence, endometrial stromal cells swell, accumulating glycogen and lipids to become decidual cells.
- This reaction creates a nutrient-rich, immunologically privileged site for the conceptus.
- Forms the maternal component of the placenta (decidua basalis).
⭐ The decidual reaction is crucial for preventing excessive trophoblastic invasion into the myometrium. A defective decidual layer can lead to placenta accreta, increta, or percreta, causing severe postpartum hemorrhage.
Clinical Correlates - When Things Go Wrong
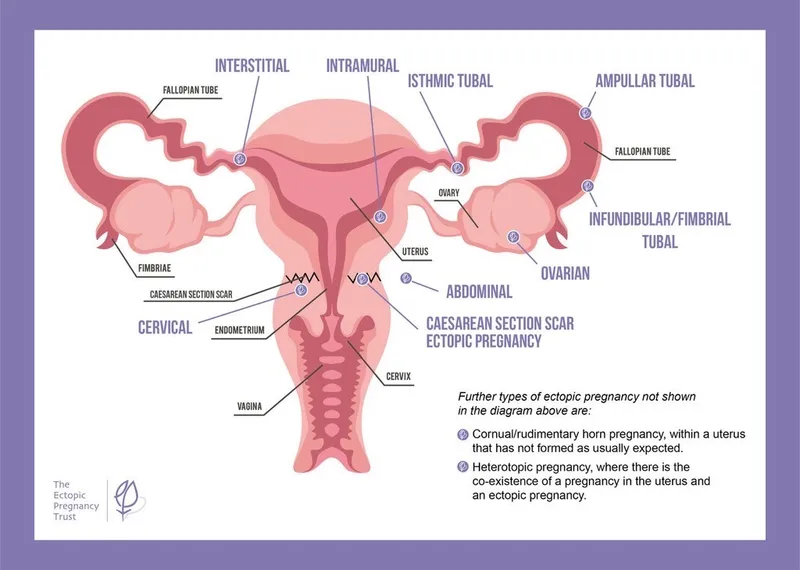
- Ectopic Pregnancy: Implantation outside the uterine cavity.
- Most common site: Ampulla of the fallopian tube.
- Presents as a surgical emergency (pain, bleeding).
- Placenta Previa: Implantation over or near the internal cervical os.
- Key symptom: painless third-trimester bleeding.
- Placenta Accreta Spectrum: Abnormal placental invasion into the uterine wall.
- Risk ↑ with prior C-sections, uterine surgery.
⭐ A history of cesarean delivery significantly increases the risk for both placenta previa and accreta.
- Implantation occurs ~6-12 days post-fertilization, most commonly on the posterior uterine wall.
- The blastocyst must hatch from the zona pellucida before embedding.
- Syncytiotrophoblast invades the endometrium and secretes hCG to maintain the corpus luteum.
- The endometrium transforms via the decidual reaction to support the pregnancy.
- Ectopic pregnancy most commonly occurs in the ampulla of the fallopian tube.
- Placenta previa is implantation over or near the internal cervical os.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

