Static Lung Volumes - Building Block Breaths
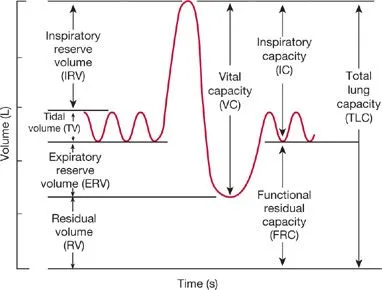
- Four non-overlapping volumes; these are the fundamental units from which lung capacities are derived.
- Tidal Volume (TV): Air in a normal, quiet breath. (~500 mL)
- Inspiratory Reserve Volume (IRV): Max air inhaled beyond normal TV inspiration. (~3000 mL)
- Expiratory Reserve Volume (ERV): Max air exhaled beyond normal TV expiration. (~1200 mL)
- Residual Volume (RV): Air left after maximal exhalation; prevents alveolar collapse. (~1200 mL)
⭐ Residual Volume (RV) cannot be measured by simple spirometry. Measurement requires helium dilution or body plethysmography.
Static Lung Capacities - Power-Up Combos

-
Inspiratory Capacity (IC)
- Max air inhaled after a normal tidal expiration.
- $IC = TV + IRV$
-
Functional Residual Capacity (FRC)
- Air in lungs after normal expiration; represents the equilibrium point for the respiratory system.
- $FRC = ERV + RV$
-
Vital Capacity (VC)
- Max air exhaled after a maximal inspiration. A measure of usable lung volume.
- $VC = IRV + TV + ERV$
-
Total Lung Capacity (TLC)
- Total air in lungs after a maximal inspiration.
- $TLC = VC + RV$
⭐ FRC cannot be measured by simple spirometry because it includes Residual Volume (RV). It requires helium dilution or body plethysmography. It is the volume at which lung inward recoil is balanced by chest wall outward spring.
Dynamic Flow Metrics - The Need for Speed
- Forced Vital Capacity (FVC): Total air exhaled forcefully after a maximal inspiration. In restrictive diseases, FVC is significantly ↓.
- Forced Expiratory Volume in 1 second (FEV₁): Volume exhaled in the first second. Reflects airflow rate; significantly ↓ in obstructive diseases.
- FEV₁/FVC Ratio: The percentage of FVC exhaled in the first second. This is the key metric to differentiate obstructive from restrictive lung diseases.
- Normal ratio is typically ≥ 75%.

⭐ In obstructive lung disease (e.g., COPD, asthma), both FEV₁ and FVC decrease, but FEV₁ decreases more, leading to a scooped-out spirometry curve and a hallmark $FEV_1/FVC$ ratio < 70%. Restrictive diseases show a normal or ↑ ratio.
Clinical Patterns - Obstructive vs. Restrictive
- Obstructive: Difficulty exhaling air due to increased airway resistance. Think "Outflow" problem.
- Restrictive: Difficulty expanding lungs, leading to reduced lung volumes. Think "Inflow" problem.
| PFT Parameter | Obstructive Pattern | Restrictive Pattern |
|---|---|---|
| FEV₁ | ↓↓ | ↓ |
| FVC | ↓ | ↓↓ |
| FEV₁/FVC Ratio | < 0.7 (Diagnostic) | Normal or ↑ (≥ 0.7) |
| Total Lung Capacity (TLC) | Normal or ↑ | ↓↓ |
| Examples | COPD, Asthma | Interstitial lung disease, fibrosis |
High‑Yield Points - ⚡ Biggest Takeaways
- Residual Volume (RV) is the air remaining after maximal exhalation and cannot be measured by spirometry.
- Functional Residual Capacity (FRC), the volume at rest, is where inward lung recoil balances outward chest wall recoil.
- Vital Capacity (VC) is the maximum volume of air that can be expired after a maximal inspiration.
- In obstructive diseases, TLC and RV are ↑ due to air trapping.
- In restrictive diseases, all lung volumes and capacities are ↓.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

