Structure & Overview - The Kidney's U‑Turn
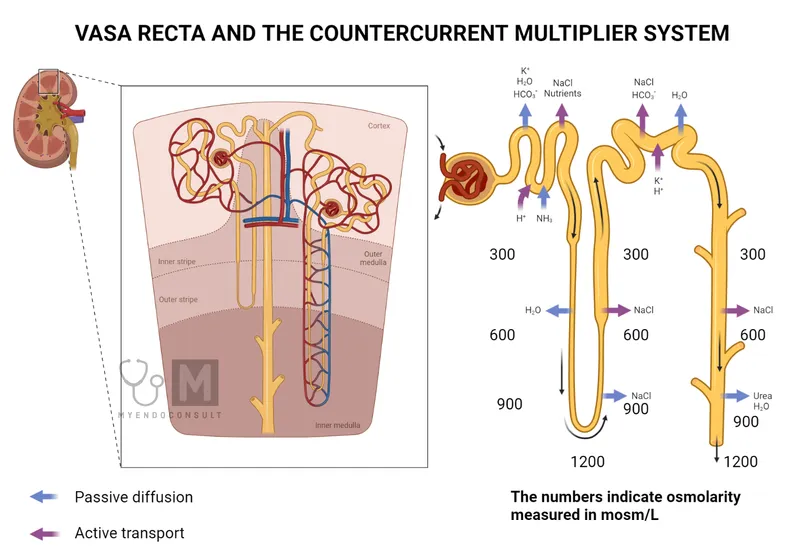
- Primary Function: Countercurrent multiplication. Establishes a hypertonic medullary interstitium, crucial for concentrating urine.
- Segments & Permeability:
- Descending Limb: Highly permeable to $H_2O$, impermeable to solutes. Water moves out, concentrating the filtrate.
- Ascending Limb: Impermeable to $H_2O$. Actively reabsorbs $Na^+$, $K^+$, and $Cl^-$, diluting the filtrate.
⭐ The vasa recta, the capillary network paralleling the loop, utilizes this gradient via countercurrent exchange to supply the medulla with blood without washing out the osmotic gradient.
Descending Limb - The Water Slide
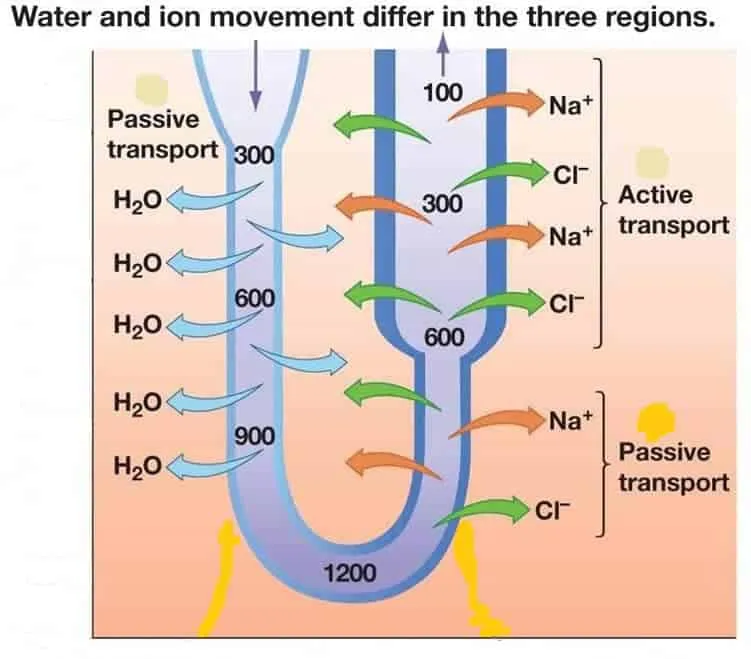
- Primary function: Passive H₂O reabsorption (osmosis).
- Driven by the hypertonic medullary interstitium.
- Mediated by Aquaporin-1 (AQP1) channels.
- Impermeable to solutes: Na⁺, K⁺, Cl⁻ are trapped in the tubule.
- Filtrate effect: Tubular fluid becomes progressively concentrated (hyperosmotic).
- Osmolarity ↑ from ~300 to 1200 mOsm/L at the hairpin turn.
⭐ High-Yield: This segment is often called the "concentrating segment" because as water leaves, the solutes left behind become highly concentrated, setting the stage for the ascending limb.
Ascending Limb - The Salt Pump
- Primary Function: Impermeable to water. Actively reabsorbs salts, diluting the tubular fluid.
- Key Transporter: The apical Na-K-2Cl (NKCC2) cotransporter is the main driver.
- Pumps $Na^+$, $K^+$, and $2Cl^-$ from the lumen into the cell.
- The basolateral $Na^+/K^+$-ATPase maintains the sodium gradient.
- Ion Movement:
- Creates a lumen-positive electrical potential.
- This charge drives the paracellular reabsorption of cations: $Mg^{2+}$ and $Ca^{2+}$.
- Result:
- Produces a hypotonic filtrate (as low as 100 mOsm/L).
- Contributes to a hypertonic medullary interstitium, crucial for concentrating urine.
⭐ Loop diuretics (e.g., Furosemide, Bumetanide) are potent inhibitors of the NKCC2 transporter. This action significantly impairs the concentrating ability of the kidney, leading to strong diuresis.
📌 Mnemonic: Loops Lose Calcium.
Countercurrent Multiplication - Gradient Powerhouse
This mechanism uses energy to generate a cortico-medullary osmotic gradient, essential for concentrating urine. The opposing flows and differing permeabilities of the Loop of Henle limbs create a powerful multiplier effect.
- Single Effect: The thick ascending limb (TAL) actively pumps NaCl into the interstitium, creating a horizontal gradient of ~200 mOsm/kg.
- Fluid Flow: The continuous flow of tubular fluid multiplies this single effect, establishing a large vertical gradient from cortex (300 mOsm/kg) to deep medulla (1200 mOsm/kg).
- Vasa Recta: Preserves the gradient via countercurrent exchange, preventing solute washout.
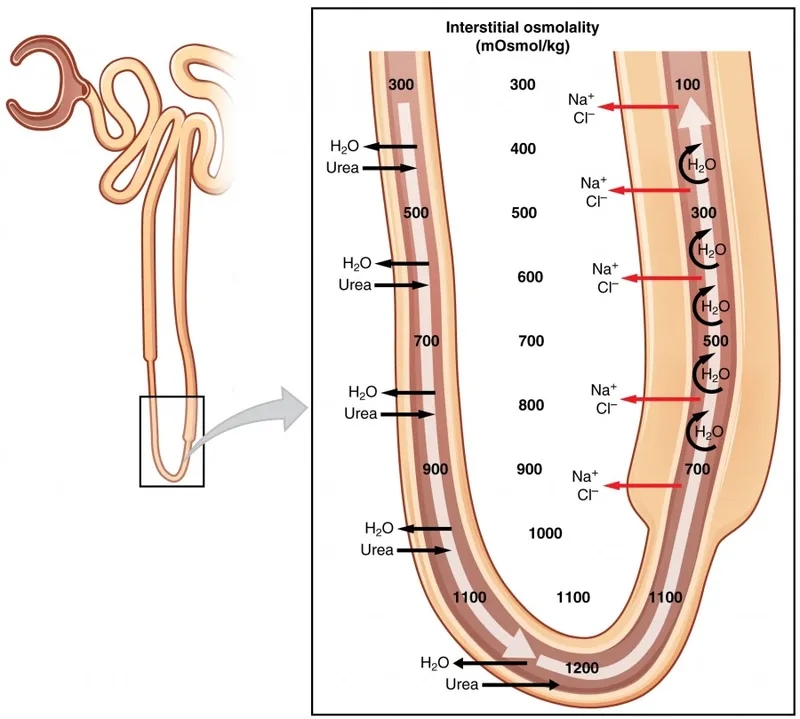
⭐ Urea recycling from the collecting duct into the medullary interstitium accounts for up to 50% of the osmotic gradient, maximizing urine concentrating ability.
High‑Yield Points - ⚡ Biggest Takeaways
- The descending limb is highly permeable to water but not solutes, which concentrates the tubular fluid.
- The thick ascending limb (TAL) is impermeable to water; it actively reabsorbs Na+, K+, and 2Cl- via the NKCC2 cotransporter.
- The TAL is the nephron's primary diluting segment.
- Countercurrent multiplication creates a hypertonic medullary interstitium, essential for final urine concentration.
- Lumen-positive potential drives paracellular reabsorption of Mg2+ and Ca2+.
- Loop diuretics inhibit the NKCC2 transporter.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

