Contractility Basics - Calcium is King
- Inotropy (Contractility): The intrinsic ability of the myocardium to contract, independent of preload and afterload.
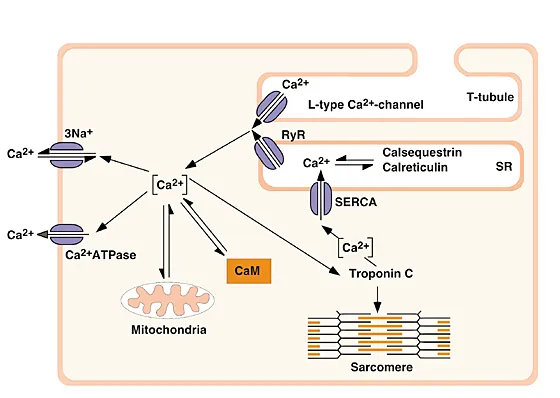
- Calcium's Role: The force of contraction is directly proportional to the intracellular Ca²⁺ concentration ($[Ca^{2+}]_i$).
- ↑ $[Ca^{2+}]_i$ leads to more $Ca^{2+}$ binding to Troponin C.
- This conformational change exposes actin-binding sites for myosin heads.
- Initiates actin-myosin cross-bridge cycling, causing muscle contraction.
⭐ Contractility is represented by the slope of the end-systolic pressure-volume relationship (ESPVR). An increase in contractility shifts the curve up and to the left.
Autonomic & Rate Effects - The Neural Knobs
-
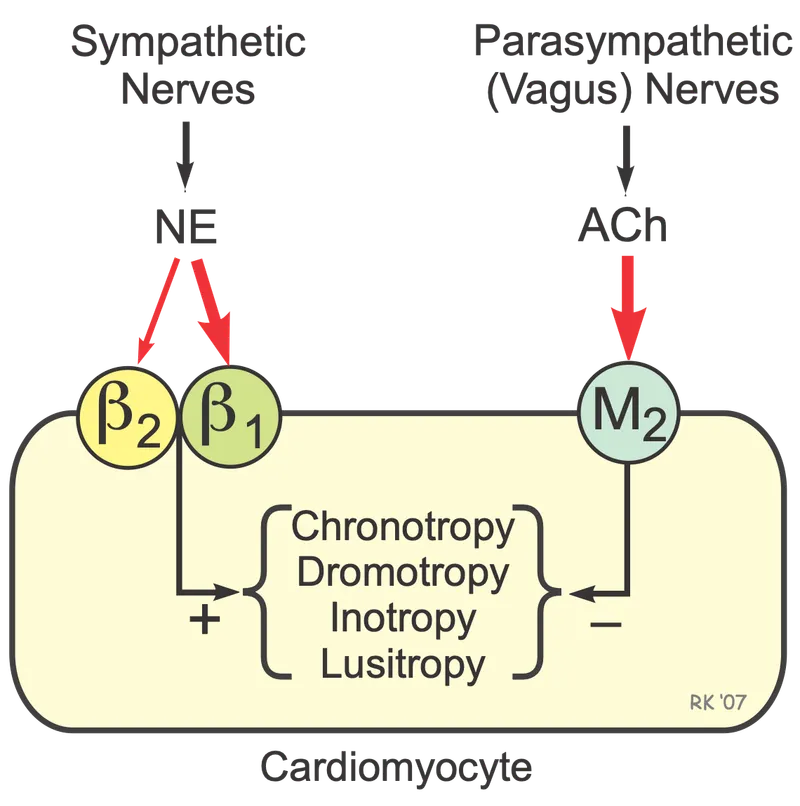
Sympathetic (β1) Stimulation: Increases contractility (positive inotropy).
-
Parasympathetic (M2) Stimulation: Opposes sympathetic effects via Gi protein, leading to ↓cAMP and reduced contractility.
-
Bowditch Effect (Treppe): An ↑ in heart rate leads to a gradual ↑ in intracellular $Ca^{2+}$ and contractility, as the $Na^+/K^+$ pump can't keep up, reducing $Na^+/Ca^{2+}$ exchanger function.
⭐ Phosphorylation of phospholamban removes its inhibition of SERCA2a, leading to faster calcium reuptake into the sarcoplasmic reticulum. This not only increases contractility but also improves relaxation (lusitropy).
Pharmacologic Inotropes - The Pharmacy Pump-Up
Pharmacologic agents modulate myocardial contractility, a key determinant of cardiac output.
| Inotrope Type | Mechanism & Examples |
|---|---|
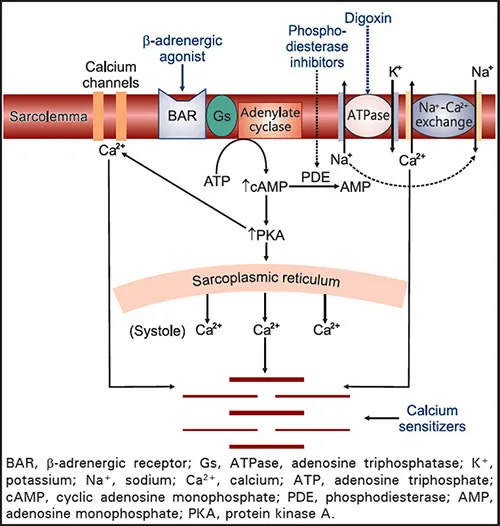
| Positive | ↑ Contractility - Digoxin: Inhibits Na⁺/K⁺-ATPase → ↑$[Na⁺]_i$ → ↓Na⁺/Ca²⁺ exchange → ↑$[Ca²⁺]_i$. - β-agonists (Dobutamine): ↑ cAMP. - PDE inhibitors (Milrinone): ↑ cAMP. |
| Negative | ↓ Contractility - β-blockers: ↓ cAMP. - Non-dihydropyridine Ca²⁺ channel blockers (Verapamil, Diltiazem): Block L-type Ca²⁺ channels. - Class I antiarrhythmics. |
⭐ Milrinone is an inodilator; it increases contractility (inotropy) by preventing cAMP breakdown in cardiac muscle and causes vasodilation by the same mechanism in smooth muscle.
Pathophysiology - Sick Heart Blues
- Factors Decreasing Contractility:
- Acidosis: ↑ $H⁺$ ions compete with $Ca²⁺$ for binding to troponin C, reducing available binding sites.
- Hypoxia/Ischemia: ↓ ATP production impairs cross-bridge cycling and $Ca²⁺$ reuptake by SERCA.
- Hypercapnia: Elevated $CO₂$ leads to respiratory acidosis, compounding the effects of low pH.
⭐ In heart failure with reduced ejection fraction (HFrEF), there is a state of chronically decreased intrinsic contractility due to receptor downregulation and impaired signaling.
High‑Yield Points - ⚡ Biggest Takeaways
- Contractility is the heart's intrinsic pumping force, independent of preload and afterload.
- It's primarily driven by intracellular Ca²⁺ concentration; more Ca²⁺ means a stronger contraction.
- Sympathetic stimulation (via β₁ receptors) and catecholamines are major positive inotropes, increasing cAMP and Ca²⁺.
- Digoxin boosts contractility by inhibiting the Na⁺/K⁺-ATPase, leading to increased intracellular Ca²⁺.
- Negative inotropes include β-blockers, calcium channel blockers, acidosis, and hypoxia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

