Mechanism of Action - Unwinding the Damage
-
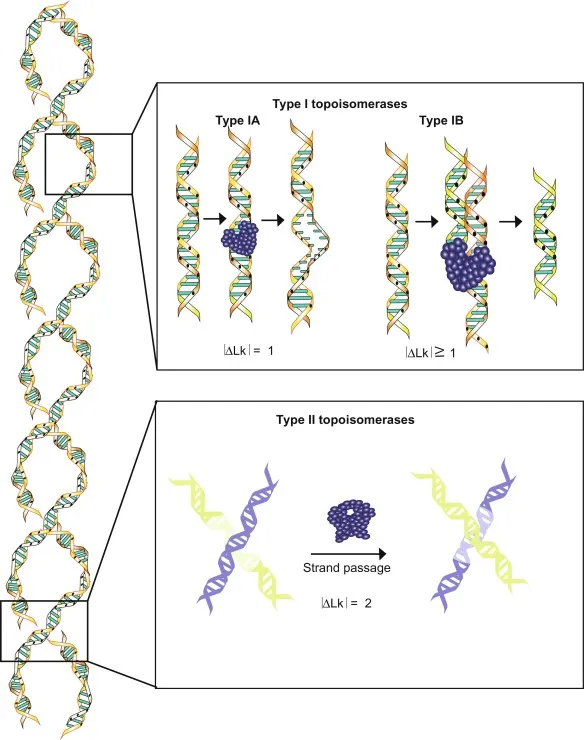
Topoisomerase I Inhibitors (e.g., Irinotecan, Topotecan):
- Create single-strand nicks in DNA to relieve supercoiling.
- Inhibitors bind to the Topo-I-DNA complex, preventing re-ligation of the nick.
-
Topoisomerase II Inhibitors (e.g., Etoposide, Teniposide):
- Create transient double-strand breaks.
- Inhibitors stabilize the Topo-II-DNA complex, preventing re-ligation.
-
Result: Accumulation of DNA strand breaks triggers cell cycle arrest and apoptosis.
⭐ High-Yield: Topoisomerase II inhibitors are cell cycle-specific, acting primarily during the S and G2 phases.
📌 Mnemonic: Topo-I makes 1 cut. Topo-II makes 2 cuts.
Topoisomerase I Inhibitors - The 'Tecan' Team
📌 Mnemonic: Irinotecan & Topotecan inhibit Topoisomerase I ('1 T-can').
- Mechanism: Inhibit topoisomerase I, preventing the re-ligation of single-strand breaks in DNA. This leads to the accumulation of DNA damage and triggers apoptosis during the S-phase of the cell cycle.
| Drug | Primary Use | Key Toxicities |
|---|---|---|
| Irinotecan | Metastatic colorectal cancer (often in FOLFIRI regimen) | Severe Diarrhea (cholinergic, acute; secretory, delayed). Myelosuppression. |
| Topotecan | Ovarian cancer, Small Cell Lung Cancer (SCLC) | Myelosuppression (dose-limiting neutropenia, thrombocytopenia), alopecia. |
Topoisomerase II Inhibitors - Double-Strand Breakers
These agents prevent the re-ligation of double-strand DNA breaks induced by Topoisomerase II, leading to permanent DNA damage and apoptosis.
| Agent Class | Mechanism of Action (MOA) | Clinical Use | Key Toxicities |
|---|---|---|---|
| Etoposide, Teniposide | Inhibit Topoisomerase II, causing DNA degradation. Cell cycle-specific for late S & G2 phases. | Solid tumors (testicular, small cell lung), leukemias, lymphomas. | Myelosuppression, alopecia. |
| Anthracyclines (Doxorubicin, Daunorubicin) | 1. Inhibit Topoisomerase II. 2. Generate free radicals via iron-dependent reactions. 3. Intercalate into DNA. | Broad spectrum: solid tumors (breast, ovary), hematologic malignancies (leukemias, lymphomas). | Cardiotoxicity (dose-dependent dilated cardiomyopathy), myelosuppression, alopecia, red urine. |
⭐ The lifetime cumulative dose of doxorubicin must be monitored closely. Cardiotoxicity is prevented with dexrazoxane, an iron-chelating agent.
High‑Yield Points - ⚡ Biggest Takeaways
- Topoisomerase I inhibitors (Irinotecan, Topotecan) cause single-strand DNA breaks. A key toxicity of Irinotecan is severe diarrhea.
- Topoisomerase II inhibitors (Etoposide, Teniposide) induce double-strand DNA breaks. Their dose-limiting toxicity is myelosuppression.
- Anthracyclines (e.g., Doxorubicin) also inhibit Topo II; their most feared side effect is irreversible, dose-dependent cardiotoxicity.
- Bleomycin induces free radical damage to DNA and is uniquely associated with pulmonary fibrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

