Omphalitis - Belly Button Blues
-
Definition: Infection of the umbilical stump and/or periumbilical tissues, typically occurring in the first two weeks of life.
-
Etiology: Polymicrobial. Most common organisms are Staphylococcus aureus, Streptococcus pyogenes, and Gram-negative bacteria (E. coli, Klebsiella pneumoniae).
-
Risk Factors: Low birth weight, home birth, non-sterile delivery conditions, umbilical catheterization, and prolonged rupture of membranes.
⭐ Omphalitis is a clinical diagnosis. Any umbilical discharge should be cultured, but treatment should not be delayed pending results.
Clinical Features & Staging - The Red Flag Stump

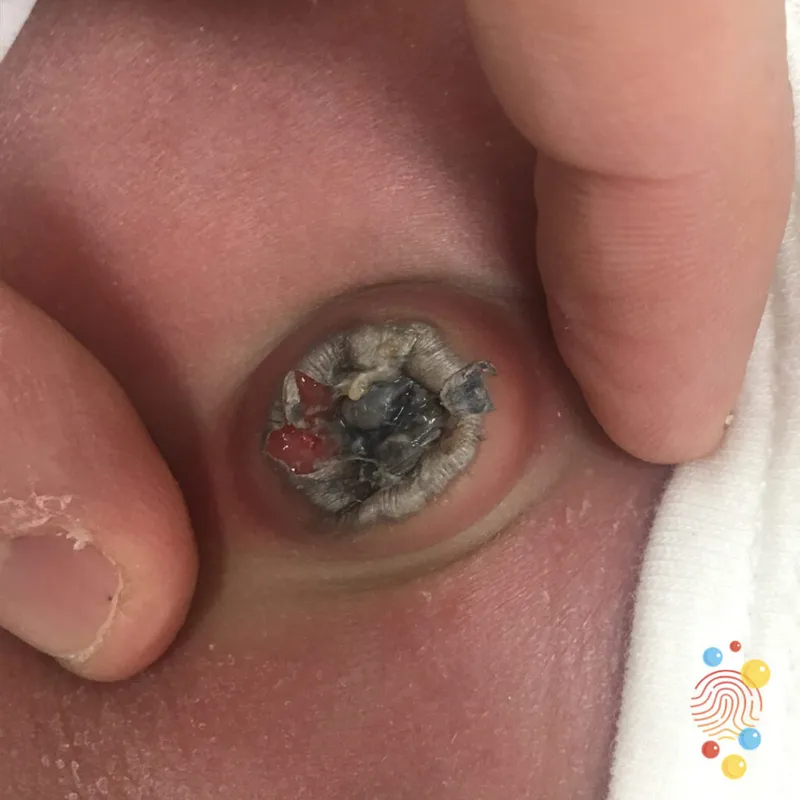
- Local Signs: Periumbilical erythema, edema, tenderness, foul-smelling purulent discharge.
- Systemic Signs (Sepsis): Fever/hypothermia, lethargy, poor feeding, irritability.
- Stage 1: Localized infection without systemic toxicity.
- Stage 2: Cellulitis extending >2 cm from the umbilicus, with systemic signs.
⭐ The most common complication of omphalitis is peritonitis.
- Stage 3: Extensive cellulitis with evidence of deeper tissue involvement (e.g., necrotizing fasciitis).
Diagnosis & Differentials - Rule-Out Roundup
- Primarily Clinical: Diagnosis rests on periumbilical erythema, tenderness, induration, or purulent discharge.
- Investigations (for systemic illness/complications):
- Labs: Blood culture, CBC, CRP.
- Local: Pus swab for culture & sensitivity.
- Imaging: Ultrasound Doppler to exclude portal vein thrombosis or intra-abdominal abscesses.
- Differential Diagnosis:
- Umbilical Granuloma: Moist, pink, friable tissue; no periumbilical inflammation.
- Patent Urachus: Persistent clear/straw-colored discharge.
- Umbilical Hernia.
⭐ Omphalitis is a major risk factor for portal vein thrombosis in neonates, potentially leading to portal hypertension later in life.
Management - Stump Strategy
-
Mild Disease (Erythema <2 cm, no systemic signs):
- Topical antimicrobials (e.g., mupirocin) and dry cord care.
-
Moderate/Severe Disease (Erythema >2 cm or systemic signs):
- Requires hospitalization and parenteral IV antibiotics.
⭐ The umbilical cord is a potential site for tetanus infection in neonates (Tetanus neonatorum).
- IV Regimen: Ampicillin + Gentamicin OR Cloxacillin + Cefotaxime.
- Surgical consultation for debridement if necrotizing fasciitis is suspected.
Complications - When It Goes Wrong
- Local Spread:
- Cellulitis, abscess formation.
- Necrotizing fasciitis (NF): Rapidly spreading necrosis.
- Systemic Invasion:
- Sepsis, septic shock.
- Vascular & Contiguous Spread:
- Portal Vein Thrombosis (via umbilical vein).
- Peritonitis.
- Liver abscess.
⭐ Necrotizing fasciitis is the most dreaded local complication, carrying high mortality.
📌 Mnemonic: '''Sepsis And Nasty Fasciitis Lead to Peritonitis'''
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of omphalitis is Staphylococcus aureus.
- Presents with periumbilical erythema, edema, and tenderness, often with purulent discharge.
- Systemic signs like fever or lethargy warrant immediate IV antibiotics.
- Most common complication is sepsis/peritonitis; the most feared is necrotizing fasciitis.
- Treatment is with IV antistaphylococcal antibiotics and an aminoglycoside.
- Clean, dry cord care is the most important preventive measure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

