Risk Factors - Fungal Crash Gate
-
Maternal Factors:
- Maternal candidal vaginitis
- Chorioamnionitis
- Prolonged rupture of membranes
-
Neonate Factors (📌 CANDIDA):
- Central venous catheters (CVC) & TPN
- Antibiotics (prolonged, broad-spectrum)
- Necrotizing enterocolitis (NEC) / GI surgery
- Devices (endotracheal tubes, V-P shunts)
- Immaturity: Extreme prematurity (< 28 wks), VLBW (< 1500 g)
- Dermal breakdown / Congenital skin defects
- Adrenal steroids (postnatal)
⭐ The single most important risk factor for invasive candidiasis is extreme prematurity, especially VLBW (< 1500 g) and ELBW (< 1000 g) infants.
Clinical Features - Yeast Beast's Manifestations
-
Congenital Candidiasis (Acquired in-utero)
- Presents within < 6 days of life.
- Skin: Generalized erythematous maculopapular rash, vesicles, or pustules; scaling on palms/soles.
- Cord: Funisitis (inflammation of the umbilical cord).
- Systemic invasion is rare but severe.
-
Acquired Candidiasis (Postnatal)
- Mucocutaneous:
- Oral Thrush: White, curd-like plaques on buccal mucosa/tongue.
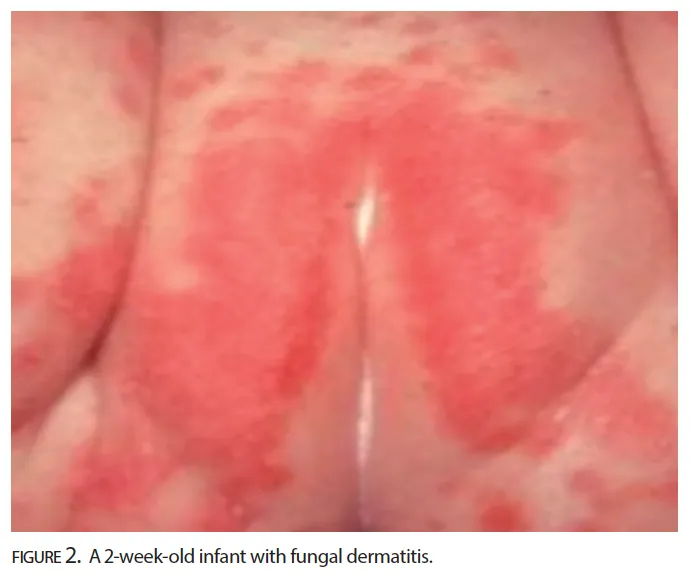
- Diaper Dermatitis: Beefy-red erythema with satellite papules/pustules.
- Invasive/Systemic Disease:
- Mimics bacterial sepsis: apnea, bradycardia, temp instability, poor feeding.
- Renal: Fungus balls → urinary obstruction.
- CNS: Meningitis, ventriculitis, abscess.
- Eyes: Chorioretinitis, endophthalmitis.
- Mucocutaneous:
⭐ All neonates with candidemia require a dilated retinal exam by an ophthalmologist to screen for endophthalmitis.
Diagnosis - Catching the Culprit
- Gold Standard: Blood culture (automated systems).
- ⚠️ Low sensitivity (<50%); may be negative in deep-seated infection.
- Key Samples:
- Urine (catheterized/suprapubic aspirate) is crucial.
- CSF analysis & culture (if CNS signs or positive blood culture).
- Sterile site fluid/tissue biopsy.
- Biomarkers (Rapid Detection):
- Fungal cell wall marker: $1,3-β-D-glucan$.
- PCR-based assays (e.g., T2Candida Panel).
- Screening for Dissemination:
- Dilated fundoscopy (for endophthalmitis).
- Renal & abdominal ultrasound.
- Echocardiogram.
⭐ A positive urine culture for Candida in a high-risk neonate is highly suggestive of systemic infection, even with negative blood cultures.
Management & Prophylaxis - Fungus Fight Plan
-
Systemic Candidiasis (Invasive):
- First-line: Amphotericin B deoxycholate (0.5-1 mg/kg/day IV).
- Alternative/Step-down: Fluconazole (12 mg/kg loading dose, then 6 mg/kg/day).
- Severe/CNS infection: Liposomal Amphotericin B (5 mg/kg/day).
- Duration: Treat for 14 days after first negative blood culture & clinical resolution.
-
Management Flow:
- Prophylaxis (High-Risk Infants):
- Indicated for VLBW/ELBW infants (<1000g or <28 wks) in high-incidence NICUs.
- Regimen: Fluconazole (3-6 mg/kg IV/PO twice weekly).
⭐ In catheter-associated candidemia, prompt removal of the central venous catheter is crucial and associated with significantly lower mortality.

High‑Yield Points - ⚡ Biggest Takeaways
- Systemic neonatal candidiasis is a major cause of late-onset sepsis in VLBW/ELBW infants.
- Key risk factors include prematurity, central lines, and prolonged antibiotic use.
- Candida albicans is the most common cause, but C. parapsilosis is linked to TPN and catheters.
- Diagnosis is confirmed by positive culture from a sterile site like blood or CSF.
- Amphotericin B deoxycholate is the first-line therapy for invasive disease.
- Fungal balls in the kidney are a characteristic complication.
- Fluconazole prophylaxis is crucial for high-risk infants in endemic NICUs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

