Pathophysiology - Guts Under Siege
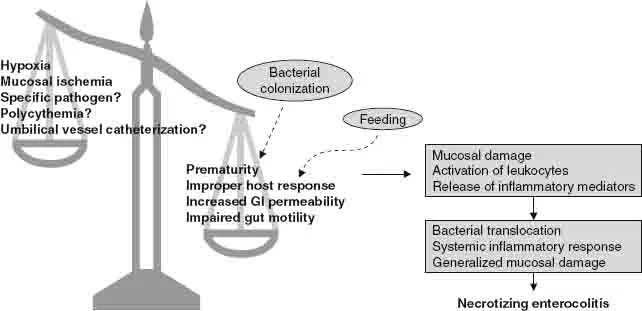
NEC is multifactorial, rooted in a triad of insults targeting the vulnerable premature intestine:
- Intestinal Ischemia: Reduced blood flow from events like perinatal asphyxia or shock compromises mucosal integrity.
- Enteral Feeding: Particularly formula, provides a substrate for pathogenic bacteria to proliferate.
- Bacterial Translocation: An immature gut barrier and abnormal colonization allow bacteria to invade the bowel wall.
This combination unleashes an uncontrolled inflammatory cascade (↑ PAF, TNF-α), leading to coagulative necrosis and potential perforation.
⭐ High-Yield: The terminal ileum and proximal ascending colon are the most commonly affected sites.
Risk Factors & Prevention - Hedging the Bets
-
Major Risk Factors:
- Prematurity & VLBW/ELBW (single biggest risk)
- Formula feeding (vs. human milk)
- Birth asphyxia & shock
- Congenital heart disease (esp. PDA)
- Umbilical catheterization
-
Protective Measures:
- Antenatal steroids
- Exclusive human milk diet
- Probiotics (e.g., Lactobacillus, Bifidobacterium)
⭐ An exclusive human milk diet is the single most effective preventive measure, reducing NEC risk by over 50%.
Clinical Features & Labs - The Telltale Signs
- Systemic Signs: Often subtle and non-specific. Includes lethargy, apnea, bradycardia, and temperature instability.
- Gastrointestinal (GI) Signs: More specific indicators.
- Feeding intolerance (vomiting, increased gastric residuals).
- Abdominal distension and tenderness.
- Hematochezia (bright red blood in stools).
- Lab Findings: Key markers of inflammation and metabolic derangement.
- Metabolic acidosis
- Thrombocytopenia (platelets < 100,000/mm³)
- Hyponatremia
- Elevated C-Reactive Protein (CRP)
⭐ Abdominal distension is the most common and often the earliest clinical sign of NEC.
Imaging & Staging - X-Ray Clues
Abdominal X-ray is the primary imaging modality for diagnosis and staging, based on Modified Bell's criteria.
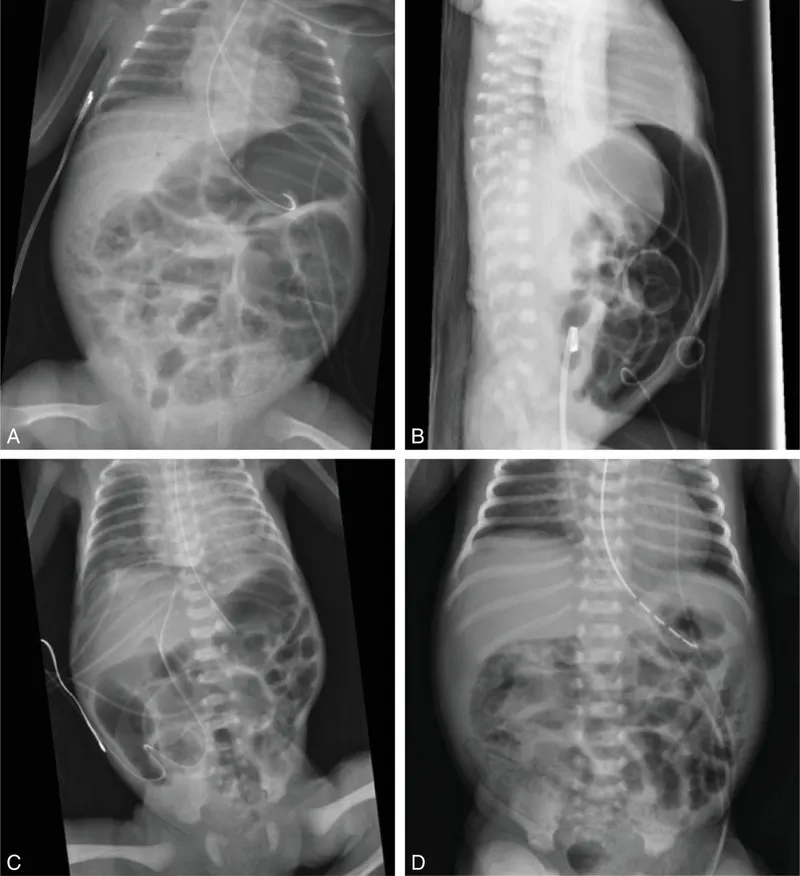
| Stage | Classification | Key X-Ray Findings |
|---|---|---|
| I | Suspected NEC | Normal or mild, non-specific ileus. |
| II | Proven NEC | Pneumatosis intestinalis (hallmark); portal venous gas. > ⭐ Pneumatosis intestinalis (gas in the bowel wall) is the pathognomonic radiological sign for NEC. |
| III | Advanced NEC | Pneumoperitoneum (indicates perforation). |
- Pneumoperitoneum is a surgical emergency.
Management - The Action Plan
-
Medical Management: Initiate supportive care immediately.
- NPO (Nil Per Os), IV fluids, and nasogastric decompression.
- Broad-spectrum antibiotics (e.g., Ampicillin + Gentamicin + Metronidazole).
- Total Parenteral Nutrition (TPN) for nutritional support.
-
Surgical Management:
⭐ Pneumoperitoneum on an abdominal X-ray is an absolute indication for immediate surgical intervention.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common gastrointestinal emergency in neonates, primarily affecting preterm infants.
- Pneumatosis intestinalis (gas in the bowel wall) is the pathognomonic sign on abdominal X-ray.
- Bell's staging is crucial for classifying severity and guiding management.
- Management cornerstone is bowel rest (NPO), broad-spectrum antibiotics, and supportive care.
- Pneumoperitoneum indicates bowel perforation, an absolute indication for surgery.
- The terminal ileum and proximal colon are the most commonly affected sites.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

