Viral Gastroenteritis - Tiny Gut Wreckers
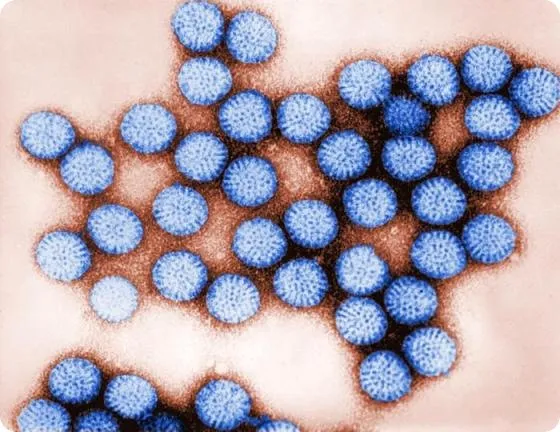
- Rotavirus: Was the #1 cause of severe dehydrating diarrhea in young children; now vaccine-preventable. Peaks in winter. Stool ELISA for diagnosis.
- Norovirus: Leading cause now. "Winter vomiting bug." Explosive vomiting, short incubation. Common in outbreaks (cruise ships, schools).
- Adenovirus: Can cause prolonged diarrhea (up to 2 weeks) and may be associated with pharyngoconjunctival fever.
Management:
- Cornerstone: Low-osmolarity ORS.
- Zinc supplementation: 10-20 mg/day for 14 days reduces duration & severity.
- Probiotics (e.g., Lactobacillus rhamnosus GG) may shorten course.
⭐ The Rotavirus vaccine carries a small risk of intussusception, typically within a week of the 1st or 2nd dose.
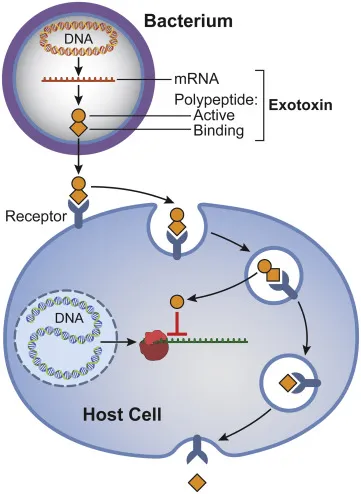
Bacterial Gastroenteritis - The Toxin Titans
-
Preformed Toxin (Rapid Onset: 1-6 hrs)
- Staphylococcus aureus: Heat-stable toxin. Source: Mayonnaise, creams, poultry. Predominantly vomiting.
- Bacillus cereus (Emetic form): Source: Reheated fried rice. Mimics S. aureus.
-
Toxin Formed In-Vivo (Slower Onset)
- Bacillus cereus (Diarrheal form): Onset 6-18 hrs. Source: Meats, vegetables. Watery diarrhea.
- Clostridium perfringens: Onset 8-16 hrs. Source: Reheated meat, gravy. Spores germinate in gut.
- ETEC (Enterotoxigenic E. coli): Major cause of Traveler's Diarrhea. Watery, non-bloody stools.
⭐ ETEC Toxins: Heat-Labile (LT) toxin ↑cAMP, similar to cholera toxin. Heat-Stable (ST) toxin ↑cGMP. Both cause chloride and water secretion.
Protozoal Diarrhea - Unwelcome Houseguests
- Giardia lamblia: Most common cause. Greasy, foul-smelling, floating stools (steatorrhea) leading to malabsorption & FTT. Rx: Metronidazole.
- Entamoeba histolytica: Amoebic dysentery (bloody stools); classic flask-shaped ulcers. Can cause liver abscess. Rx: Metronidazole + luminal agent (e.g., Diloxanide).
- Cryptosporidium parvum: Profuse, watery diarrhea. Severe/chronic in immunocompromised (e.g., HIV). Dx: Oocysts on modified acid-fast stain. Rx: Nitazoxanide.
⭐ Amoebiasis: Liver abscess is the most common extra-intestinal manifestation, presenting with fever, RUQ pain, and "anchovy sauce" pus on aspiration.
Dehydration & Management - The Rehydration Rescue
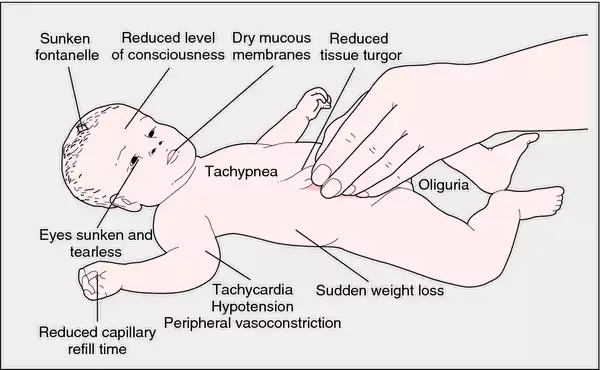
- Assessment: Graded by weight loss (Mild <5%, Moderate 5-10%, Severe >10%), sensorium, thirst, and skin turgor.
- Low-Osmolarity WHO ORS: The cornerstone. Composition (mEq/L): Na⁺ 75, K⁺ 20, Cl⁻ 65, Citrate 10, Glucose 75. Total osmolarity: 245 mOsm/L.
⭐ In severe dehydration, the initial fluid bolus is always with an isotonic crystalloid like Ringer's Lactate or 0.9% Normal Saline to rapidly restore circulatory volume. Avoid dextrose-containing fluids initially.
High‑Yield Points - ⚡ Biggest Takeaways
- Rotavirus is the most common cause of severe diarrhea in infants; live-attenuated vaccine is preventive.
- Cholera causes profuse “rice-water” stools leading to severe dehydration; requires aggressive fluid replacement.
- Shigella causes bacillary dysentery (bloody, mucoid stools) and may trigger febrile seizures.
- Typhoid fever presents with “pea-soup” diarrhea, step-ladder fever, and characteristic rose spots.
- Giardiasis leads to foul-smelling, fatty stools (steatorrhea); common in daycare attendees.
- Management cornerstone: Low-osmolality ORS for rehydration and Zinc supplementation to shorten duration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

