Uterine Compression Sutures - The Uterine Squeeze
- Surgical technique for postpartum hemorrhage (PPH) refractory to medical management, primarily for uterine atony.
- Physically compresses the myometrium to control bleeding from open uterine sinuses.
- Common types include the B-Lynch, Hayman, and Pereira sutures.

⭐ A major advantage is uterine preservation, offering a crucial alternative to hysterectomy and maintaining the patient's future fertility potential.
Technique Types - Stitching to Stop
- Primary Goal: Apply continuous mechanical compression to the myometrium to control atonic PPH, effectively "squeezing" the bleeding vessels shut.
- 📌 Mnemonic: "Big Hug, Please!" for common suture types (B-Lynch, Hayman, Pereira).
| Technique | Description | Key Feature |
|---|---|---|
| B-Lynch | The original "uterine sandwich." A continuous "brace-like" suture is placed from the anterior uterine segment, over the fundus, to the posterior wall, and back through the cavity. | Requires a hysterotomy. The most studied technique. |
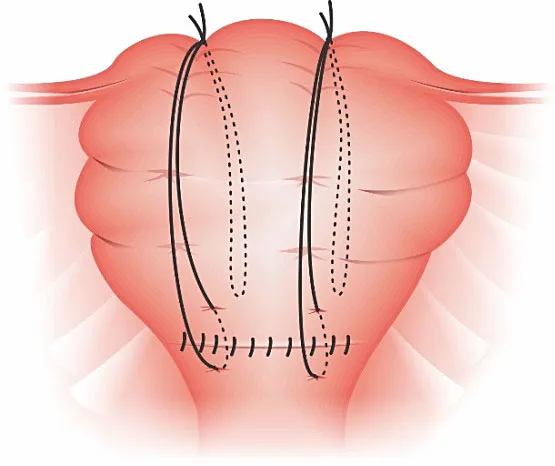
| Hayman | Simplified vertical compression sutures. Straight needles pass from the anterior uterine wall through to the posterior wall, tied over the fundus. | No hysterotomy needed. Can be performed more quickly. |
| Pereira | Uses a series of transverse and longitudinal sutures to create a constricting network around the uterus. | Avoids hysterotomy. Less commonly performed. |
- ⚠️ Potential Complications: Though rare, risks include uterine ischemia, necrosis, and pyometra.
Placement & Principles - The How-To Guide
- Goal: Mechanically compress the myometrium to occlude bleeding sinuses.
- Suture: Use large, absorbable sutures (e.g., #1-0 chromic or vicryl) on a 70-90 mm needle.
- Techniques:
- B-Lynch: Most common. Suture placed like "braces" over the uterus. Requires hysterotomy.
- Hayman/Pereira: Simpler, faster. No hysterotomy needed. Multiple vertical sutures.
⭐ Pearl: Always use absorbable suture material to prevent long-term complications like uterine erosion or sinus tract formation. The suture dissolves as the uterus involutes.
Complications & Outcomes - Risks vs Rewards
-
Risks & Complications:
- ⚠️ Uterine Ischemia/Necrosis: Most feared complication, potentially leading to uterine wall sloughing and requiring hysterectomy.
- Infection: Endometritis or pyometra formation.
- Intrauterine Adhesions (Asherman's Syndrome): May form, impairing future fertility.
- Suture Erosion: Sutures can migrate through the myometrium into the cavity.
-
Rewards & Outcomes:
- High Success Rate: Effectively controls hemorrhage in >90% of cases, preserving the uterus.
- Fertility Preservation: Successful subsequent pregnancies are frequently reported.
⭐ The primary reward is avoiding emergency peripartum hysterectomy, thereby preserving fertility in patients with uterine atony unresponsive to medical therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Uterine compression sutures are a crucial surgical option for postpartum hemorrhage (PPH) unresponsive to medical therapy, most often from uterine atony.
- The B-Lynch suture is the most well-known technique; others include the Hayman and Pereira methods.
- The primary goal is mechanical compression of the myometrium to control bleeding by physically closing open sinuses.
- This intervention is uterus-sparing, often preventing the need for a peripartum hysterectomy.
- Potential risks, though rare, include uterine ischemia, necrosis, and intrauterine adhesions (Asherman syndrome).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

