Definition & Diagnosis - The Stubborn Afterthought
- Definition: Failure of the placenta to deliver within 30 minutes of birth with active management, or 60 minutes with physiological management.
- Etiologies:
- Placenta Adherens: Weak myometrial contractions fail to detach a normally implanted placenta.
- Trapped Placenta: Detached placenta is trapped by a closing cervix.
- Placenta Accreta Spectrum: Abnormal placental invasion into the uterine wall.
- Diagnosis:
- Primarily clinical, based on the time criteria.
- Signs: Umbilical cord does not lengthen, no gush of blood, fundus remains high.
- Ultrasound can confirm retained products of conception.

⭐ Gentle cord traction during active management (Brandt-Andrews maneuver) is diagnostic and therapeutic, but excessive force can cause uterine inversion or cord avulsion.
Initial Management - Gentle Persuasion
First-line, non-invasive techniques employed immediately after the diagnosis of retained placenta, prioritizing maternal stability and avoiding uterine trauma.
- Conservative Measures:
- Ensure bladder is empty (catheterize if needed).
- Initiate uterine massage to promote contraction.
- Encourage breastfeeding or nipple stimulation to release endogenous oxytocin.
- Controlled Cord Traction (CCT):
- Brandt-Andrews Maneuver: Apply gentle, sustained downward traction on the umbilical cord while simultaneously providing suprapubic counter-pressure with the other hand to prevent uterine inversion.
- Only attempt if the uterus is well-contracted.
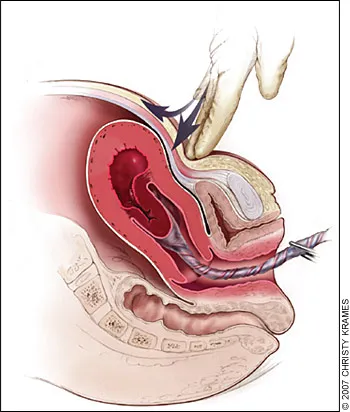
⭐ Before attempting any traction, always confirm the uterus is firm and contracted. Applying traction to an atonic uterus is a leading cause of uterine inversion.
Invasive Management - The Manual Override
- Manual Placental Extraction
- Indication: Placenta not delivered within 30 minutes of fetus.
- Prerequisites: Adequate analgesia (IV sedation/regional anesthesia), empty bladder.
- Technique: Aseptically insert one hand into the uterus, following the umbilical cord. Identify the cleavage plane between the placenta and uterine wall. Use the side of the hand in a shearing motion to separate, then gently withdraw.

- Uterine Curettage
- Indication: Failure of manual extraction or persistent bleeding from suspected retained fragments.
- Setting: Operating room with anesthesia.
- Tool: Large, blunt Bumm or "banjo" curette is preferred.
- 💡 Ultrasound guidance is critical to minimize the risk of uterine perforation and ensure complete removal.
⭐ Exam Favorite: Aggressive uterine instrumentation, particularly curettage for retained products, is the leading cause of Asherman syndrome (intrauterine adhesions), which can cause secondary amenorrhea and infertility.
High-Yield Points - ⚡ Biggest Takeaways
- Retained placenta is the failure to deliver the placenta within 30 minutes of birth.
- The placenta accreta spectrum is the most common underlying cause.
- Initial management involves controlled cord traction and uterotonic agents like oxytocin.
- If initial attempts fail, proceed to manual extraction under adequate anesthesia.
- Manual removal increases the risk of both uterine atony and endometritis.
- Suspect retained fragments in any patient with secondary PPH or uterine subinvolution.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

