Poliovirus - Paralytic Poltergeist
- Virus: Picornaviridae family (enterovirus). Small, non-enveloped, single-stranded (+) RNA virus.
- Transmission: Fecal-oral route.
- Pathogenesis:
- Replicates in oropharynx & Peyer's patches → viremia.
- Invades CNS, causing destruction of motor neurons in the anterior horn of the spinal cord.
- Clinical Features:
- Presents as asymmetric flaccid paralysis, predominantly in lower limbs.
- Sensation is intact; deep tendon reflexes are lost.
- Can lead to respiratory failure from diaphragmatic/intercostal muscle paralysis.
⭐ Post-Polio Syndrome (PPS): Decades after recovery, patients may develop new, slowly progressive muscle weakness, fatigue, and pain in previously affected muscles. This is not a reinfection.
Haemophilus influenzae - The HiB Hijacker
- Gram-negative coccobacillus (pleomorphic). Requires chocolate agar with Factor V (NAD+) and Factor X (hematin) for growth.
- Main virulence factor is the polyribosylribitol phosphate (PRP) capsule; type b (HiB) is the most pathogenic serotype, causing invasive disease.

- Pre-vaccine diseases (📌 EMOP):
- Epiglottitis (cherry-red epiglottis, drooling, dysphagia)
- Meningitis
- Otitis media
- Pneumonia
- Vaccine: HiB conjugate vaccine links the PRP capsule to a protein (e.g., tetanus toxoid), inducing a T-cell-dependent immune response and robust immunity.
- Treatment: Ceftriaxone for invasive disease; rifampin for prophylaxis of close contacts.
⭐ While the HiB vaccine is highly effective against type b, non-typeable H. influenzae (NTHi) strains lacking a capsule are now a leading cause of otitis media, sinusitis, and COPD exacerbations.
Vaccines - Jab Showdown
-
Poliovirus Vaccine:
- Inactivated (IPV - Salk): Killed virus, used in the US. Injection only. Forms IgG, but no mucosal IgA. No risk of vaccine-associated paralytic poliomyelitis (VAPP).
- Oral (OPV - Sabin): Live-attenuated. Oral route induces robust mucosal IgA. ⚠️ Carries a small risk of VAPP, especially for immunodeficient contacts. Not used in the US.
-
Haemophilus influenzae type b (Hib) Vaccine:
- Conjugate vaccine (polysaccharide + protein).
- Links PRP capsular polysaccharide to a carrier protein (e.g., tetanus toxoid).
- This design elicits a T-cell dependent response, effective in infants <2 years old.
- Prevents: Meningitis, Epiglottitis, Pneumonia.
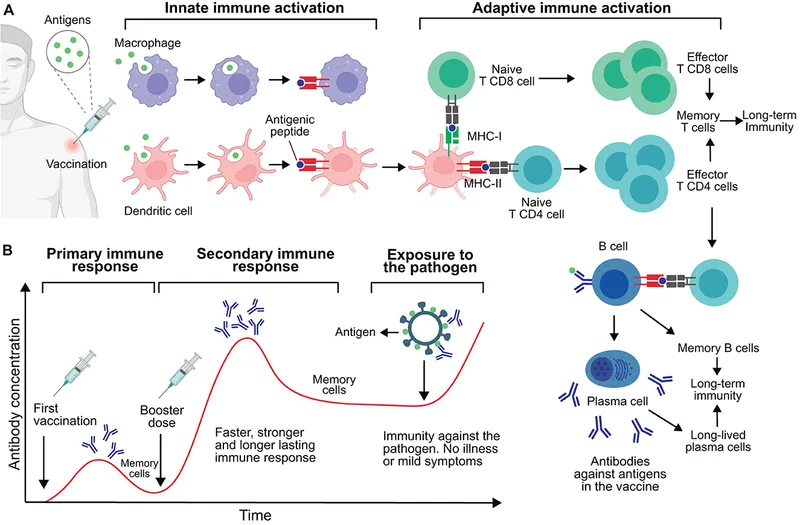
⭐ The Hib conjugate vaccine's design (linking a polysaccharide to a protein) brilliantly converts a T-cell independent antigen into a T-cell dependent one, generating a strong, long-lasting immune response in infants.
High‑Yield Points - ⚡ Biggest Takeaways
- Poliovirus, an enterovirus, causes asymmetric flaccid paralysis by destroying anterior horn cells.
- Transmission is fecal-oral; the Salk (IPV, inactivated) vaccine is used in the US to prevent rare vaccine-associated paralysis.
- Haemophilus influenzae type b (Hib) is a gram-negative coccobacillus causing meningitis, epiglottitis, and sepsis.
- Hib requires chocolate agar with factors V (NAD+) and X (hematin) for growth.
- The Hib vaccine is a polysaccharide-protein conjugate vaccine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

