Oral Microbiome - Mouth's Microbial Menagerie
- Definition: A dynamic community of commensal microbes (bacteria, fungi, viruses) in the oral cavity, vital for homeostasis.
- Key Phyla: Firmicutes, Bacteroidetes, Proteobacteria, Actinobacteria.
- Dominant Genera: Streptococcus, Veillonella, Prevotella, Fusobacterium.

⭐ Streptococcus mutans metabolizes sucrose to lactic acid, which demineralizes enamel, leading to dental caries. This biofilm formation is known as plaque.
Key Species - The Usual Suspects
| Bacterium | Gram Stain | Key Virulence Factor(s) | Associated Disease |
|---|---|---|---|
| Streptococcus mutans | Gram (+) cocci | Glucan production (biofilm), acidogenicity | Dental Caries |
| Porphyromonas gingivalis | Gram (-) rod | Gingipains (proteases), fimbriae | Periodontitis |
| Tannerella forsythia | Gram (-) rod | Proteases, cell surface glycoproteins | Periodontitis |
| Treponema denticola | Spirochete | Motility, protease activity | Periodontitis (ANUG) |
⭐ The "Red Complex" (P. gingivalis, T. forsythia, T. denticola) is a group of bacteria strongly associated with severe forms of periodontal disease.
Dental Plaque - Biofilm Builders' Brigade
- Dental plaque is a classic example of a biofilm, a structured community of bacteria that adheres to tooth surfaces.
- Its development is a multi-stage process involving specific bacterial species in a predictable sequence.
- Primary Colonizers: Aerobic bacteria like S. sanguinis attach to the pellicle.
⭐ Streptococcus mutans metabolizes sucrose into dextrans (glucans), which forms the scaffolding of plaque, enabling other bacteria to adhere.
- Secondary Colonizers: Fusobacterium nucleatum acts as a crucial bridging organism, co-aggregating with both early and late colonizers.
- Mature Biofilm: Creates an anaerobic niche, promoting the growth of pathogenic, gram-negative anaerobes (Porphyromonas gingivalis, Tannerella forsythia).
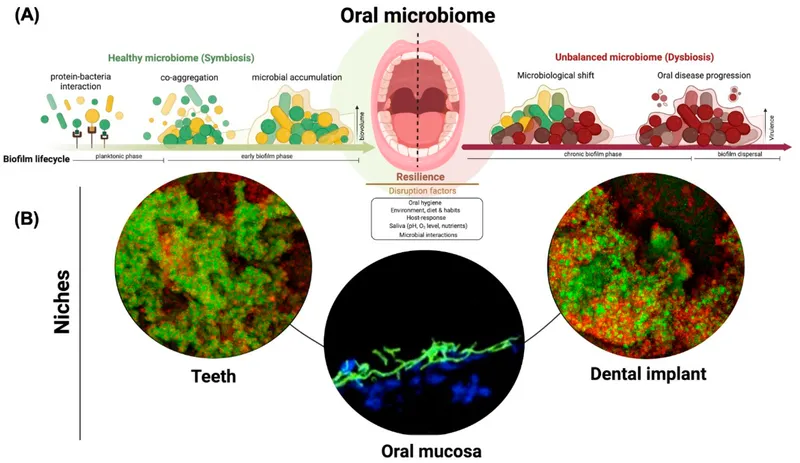
Clinical Correlations - When Good Microbes Go Bad
-
Dental Caries: Caused by acidogenic bacteria, primarily Streptococcus mutans. They ferment dietary sugars (especially sucrose) into lactic acid, which demineralizes tooth enamel.
- $Sucrose \xrightarrow{S. mutans} Lactic;Acid + Glucans/Fructans;(Biofilm)$
-
Gingivitis & Periodontitis: Results from dysbiosis-a shift to Gram-negative, anaerobic bacteria (e.g., Porphyromonas gingivalis, Tannerella forsythia) below the gumline. The host's inflammatory response to these pathogens causes progressive destruction of gingival tissue and alveolar bone.

- Systemic Disease Links:
- Infective Endocarditis: Transient bacteremia, often after dental procedures, can allow Streptococcus viridans to colonize damaged heart valves.
- Aspiration Pneumonia: Aspiration of oral anaerobes can cause lung abscesses.
⭐ High-Yield: The viridans group streptococci produce dextrans from sucrose, which helps them adhere to fibrin-platelet aggregates on previously damaged heart valves, a critical step in causing Subacute Bacterial Endocarditis (SBE).
High‑Yield Points - ⚡ Biggest Takeaways
- Viridans streptococci are the most abundant organisms, primarily α-hemolytic.
- Streptococcus mutans is the main cause of dental caries by synthesizing dextrans from sucrose.
- S. sanguinis is a major component of dental plaque and a cause of subacute bacterial endocarditis after dental work.
- Actinomyces israelii is associated with actinomycosis, forming characteristic sulfur granules.
- Porphyromonas gingivalis is a key pathogen in chronic periodontitis.
- Oral flora form biofilms (plaque), protecting them from host defenses and antimicrobials.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

