HIV-HBV Co-infection - Double Trouble Diagnosis
- Universal Screening: All HIV-positive individuals require HBV screening at initial diagnosis.
- Initial Serology Panel:
- HBsAg (Hepatitis B surface antigen)
- anti-HBs (Hepatitis B surface antibody)
- anti-HBc (Total hepatitis B core antibody)
- Key Interpretations:
- HBsAg (+): Active HBV infection.
- anti-HBs (+) & anti-HBc (+/-): Immune (natural infection or vaccination).
- Isolated anti-HBc (+): May indicate occult infection; check HBV DNA.
⭐ HIV infection significantly accelerates liver fibrosis progression in patients with chronic HBV, increasing the risk of cirrhosis and hepatocellular carcinoma by 3-6x.
HIV-HCV Co-infection - The Liver's Other Foe
- Epidemiology: Affects ~25% of HIV+ individuals, especially people who inject drugs (PWID). HIV co-infection increases the risk of chronic HCV to >80%.
- Pathophysiology: HIV accelerates HCV progression by impairing HCV-specific T-cell immunity.
- This leads to faster liver fibrosis, earlier onset of cirrhosis, and a higher risk of hepatocellular carcinoma (HCC).
- HCV itself does not accelerate HIV progression.
- Management:
- Screen all HIV+ patients with an HCV antibody test; if positive, confirm with an HCV RNA viral load.
- Initiate antiretroviral therapy (ART) for HIV first.
- Once HIV is virologically suppressed, treat HCV with Direct-Acting Antivirals (DAAs), achieving >95% cure rates.
- ⚠️ Monitor for drug-drug interactions between ART and DAAs.
⭐ In co-infected patients on effective ART, liver disease (cirrhosis, ESLD) surpasses AIDS-defining illnesses as a leading cause of mortality.
HIV-TB Co-infection - The Lethal Alliance
- HIV is the most potent risk factor for reactivating latent Mycobacterium tuberculosis (MTB), increasing annual risk from 5-10% (lifetime) to 5-10% (annually).
- Clinical presentation is stratified by CD4 count:
- CD4 >200 cells/μL: Classic upper-lobe cavitary pulmonary TB.
- CD4 <200 cells/μL: Atypical patterns; extrapulmonary disease (lymphadenitis, meningitis) and disseminated/miliary TB are common. Chest X-rays can be normal.
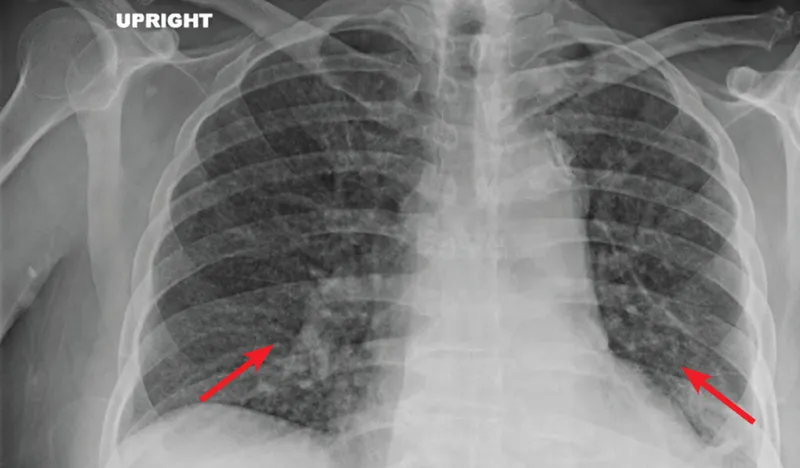
- Diagnosis: Tuberculin skin tests (TST) are unreliable due to anergy; Interferon-Gamma Release Assays (IGRAs) are preferred for latent TB. For active TB, nucleic acid amplification tests (NAAT) like Xpert MTB/RIF on sputum are crucial due to paucibacillary disease.
⭐ Paradoxical worsening of TB symptoms after starting antiretroviral therapy (ART) is the hallmark of TB-Immune Reconstitution Inflammatory Syndrome (TB-IRIS).
- Treatment Principles:
High‑Yield Points - ⚡ Biggest Takeaways
- HIV accelerates HBV and HCV progression to cirrhosis and liver cancer. Screen all new HIV patients for these co-infections.
- Tenofovir-based ART is dual-acting and preferred for HIV/HBV co-infection.
- Screen for latent TB in all HIV patients; a tuberculin skin test (TST) ≥5 mm is considered positive.
- Starting ART can trigger Immune Reconstitution Inflammatory Syndrome (IRIS), paradoxically worsening TB symptoms.
- Watch for drug-drug interactions between HCV direct-acting antivirals (DAAs) and antiretroviral therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

