HIV & Malignancy - The Unholy Alliance
- Mechanism: A triad of immunosuppression (low CD4 count), chronic inflammation, and co-infection with oncogenic viruses drives malignancy risk.
- Key Viral Co-infections:
- HHV-8: Kaposi Sarcoma
- EBV: Primary CNS Lymphoma, Burkitt Lymphoma
- HPV: Cervical & Anal Cancer
- HAART Era Shift: While effective antiretroviral therapy has ↓ AIDS-defining cancers (ADCs), non-AIDS-defining cancers (NADCs) like lung and liver cancer are now more common due to longer lifespans.
⭐ Primary CNS Lymphoma in an HIV patient is almost always associated with EBV infection and typically occurs with CD4 counts < 50/mm³.

AIDS-Defining Cancers - The Classic Trio
The risk of certain cancers skyrockets with severe immunosuppression (CD4+ < 200 cells/μL). These virally-driven malignancies are hallmarks of advanced HIV disease and are recognized as AIDS-defining conditions.
| Malignancy | Associated Virus | Key Presentation | Diagnostic Clue |
|---|---|---|---|
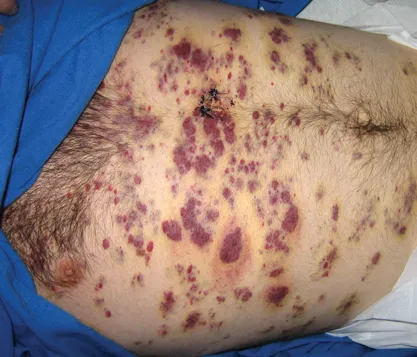
| Kaposi Sarcoma | HHV-8 | Violaceous papules/nodules on skin, hard palate, GI tract, or respiratory tract. | Biopsy: Spindle cells, neovascularization, and extravasated RBCs. |
| Primary CNS Lymphoma | EBV | Altered mental status, seizures, or focal neurological deficits. Typically a single ring-enhancing lesion on contrast MRI. | Definitive diagnosis via brain biopsy. EBV DNA in CSF is highly suggestive. |
| Invasive Cervical Cancer | HPV (16, 18) | Abnormal vaginal bleeding (often post-coital), pelvic pain, or vaginal discharge. HIV+ women require more frequent screening. | Pap smear shows dysplasia (CIN); confirmed by colposcopy and biopsy. |
Emerging Threats - The NADC List
With effective antiretroviral therapy (ART), patients with HIV live longer but face a rising tide of Non-AIDS-Defining Cancers (NADCs). These are now a more frequent cause of mortality than classic AIDS-defining cancers in the ART era.
- Key NADCs & Viral Associations:
- Anal Cancer: Human Papillomavirus (HPV)
- Hodgkin Lymphoma: Epstein-Barr Virus (EBV)
- Hepatocellular Carcinoma: Hepatitis B (HBV) & C (HCV)
- Lung Cancer: ↑ risk independent of smoking.
⭐ In the HIV population, the standardized incidence ratio for anal cancer and Hodgkin lymphoma is significantly elevated compared to the general population.
Mechanism of Malice - How HIV Drives Cancer
HIV cripples the immune system, creating a permissive environment for cancer through two primary mechanisms:
⭐ Most HIV-associated lymphomas are aggressive, high-grade B-cell types (e.g., Diffuse Large B-cell, Burkitt). Primary CNS lymphoma, caused by EBV, is an AIDS-defining illness and often presents with a solitary ring-enhancing lesion on imaging.
High‑Yield Points - ⚡ Biggest Takeaways
- Kaposi Sarcoma, caused by HHV-8, presents with characteristic violaceous skin lesions.
- Primary CNS Lymphoma, driven by EBV, typically appears as a solitary, ring-enhancing lesion on brain MRI.
- Systemic Non-Hodgkin Lymphomas are also EBV-related and frequently present in extranodal sites.
- Invasive cervical and anal cancers, caused by HPV, have a significantly higher incidence and more rapid progression.
- These malignancies often serve as an AIDS-defining illness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

