CoNS ID - The Usual Suspects
- Catalase-positive, coagulase-negative Gram-positive cocci in clusters.
- Often part of normal skin flora; opportunistic pathogens.
| Organism | Key Association | Novobiocin |
|---|---|---|
| S. epidermidis | Biofilms on hardware (catheters, prosthetics) | Sensitive |
| S. saprophyticus | UTIs in young, sexually active women | Resistant |
| S. lugdunensis | Aggressive endocarditis, abscesses | Sensitive |
S. epidermidis - The Biofilm King
- Normal flora of the skin; a major opportunistic pathogen, especially in hospital settings (nosocomial).
- Primary Virulence Factor: Production of a polysaccharide slime layer (biofilm). This allows adherence to foreign materials and protects from antibiotics and host defenses.
- Associated Infections:
- Prosthetic devices: Joints, heart valves (endocarditis).
- Intravascular catheters & IV lines → bacteremia/sepsis.
- Cerebrospinal fluid (CSF) shunts.
- Treatment: Vancomycin is the drug of choice due to widespread methicillin resistance (MRSE).
⭐ The most common cause of endocarditis on prosthetic heart valves, especially within the first 1 year post-surgery.
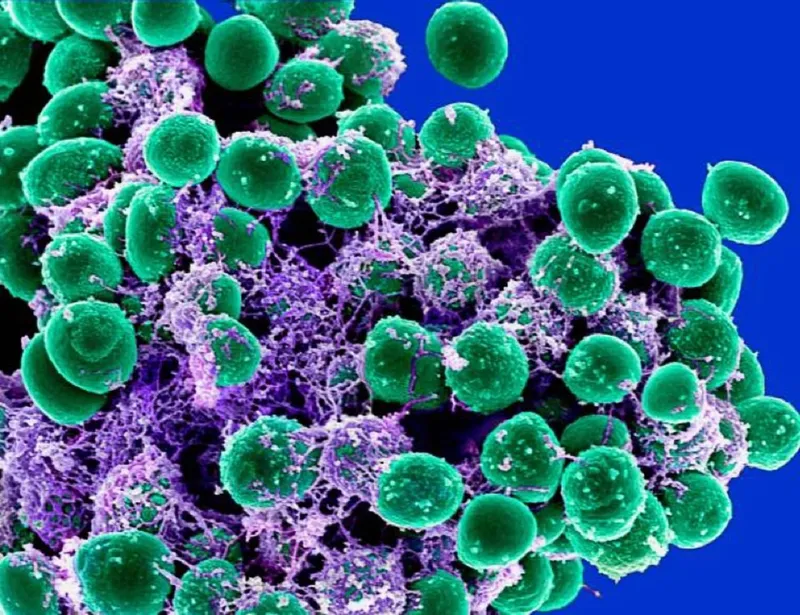
Biofilm Formation:
S. saprophyticus - UTI Specialist
- Clinical Role: A leading cause of community-acquired UTIs (cystitis), ranking second only to E. coli in its primary demographic.
- Classic Vignette: Presents as acute cystitis in young, sexually active women, often termed "honeymoon cystitis."
- Pathogenesis: Colonizes the urinary tract by adhering strongly to urothelial cells.
- Lab Diagnosis: Catalase (+), Coagulase (-).
- Treatment: Responds well to standard UTI antibiotics like TMP-SMX.
⭐ Key Distinguisher: Unlike most other coagulase-negative staphylococci, S. saprophyticus is innately resistant to novobiocin.
📌 Mnemonic: No StRESs: Novobiocin Resistant, Epidermidis is Sensitive.
Treatment Strategy - Attack & Remove
- Two-Pronged Approach: Success hinges on combining antimicrobial therapy with aggressive source control, especially removing colonized hardware.
- Primary Challenge: High prevalence of methicillin resistance and robust biofilm formation on foreign materials.
⭐ Biofilm is the Fortress: CoNS biofilms can increase antibiotic resistance up to 1000-fold, making device removal, not just drug therapy, the cornerstone of successful treatment.
High‑Yield Points - ⚡ Biggest Takeaways
- Coagulase-negative staphylococci (CoNS) are gram-positive, catalase-positive cocci.
- S. epidermidis is notorious for biofilm formation on prosthetic devices and catheters, leading to nosocomial infections.
- It is frequently methicillin-resistant (MRSE), often requiring vancomycin.
- S. saprophyticus is a common cause of UTIs in sexually active young women.
- Key differentiator: S. saprophyticus is novobiocin-resistant, whereas other CoNS are novobiocin-sensitive.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

