Vibrio Basics - Comma-Shaped Critters
- Gram-negative, motile, comma-shaped rods.
- Oxidase-positive (key differentiator from Enterobacteriaceae).
- Facultative anaerobes, found in aquatic/marine environments.
- Transmission: consumption of contaminated water or raw/undercooked seafood (especially oysters).
- Culture on Thiosulfate-Citrate-Bile Salts-Sucrose (TCBS) agar.

⭐ Most pathogenic species are halophilic (require salt for growth), except for V. cholerae and V. mimicus.
Vibrio cholerae - The Diarrhea Dynamo

- Organism: Gram-negative, motile, comma-shaped rod. Oxidase-positive.
- Transmission: Fecal-oral route, typically via contaminated water or raw/undercooked shellfish.
- Disease: Cholera-an acute, severe diarrheal illness. Presents with voluminous, painless, watery stools ("rice-water stool"), leading to rapid dehydration, electrolyte imbalance, and potential hypovolemic shock.
- Diagnosis: Stool culture on Thiosulfate-citrate-bile salts-sucrose (TCBS) agar, where it ferments sucrose to produce yellow colonies.
- Treatment: Prompt and aggressive fluid and electrolyte replacement is critical. Antibiotics (e.g., doxycycline, azithromycin) can reduce disease duration.
⭐ Oral rehydration therapy (ORT) is highly effective because the glucose-Na+ cotransport mechanism (SGLT1) in the gut remains unaffected by the cholera toxin, allowing for efficient water absorption.
Other Vibrios - Seafood Sickness Squad
- Primarily associated with consumption of raw/undercooked seafood (especially oysters) or exposure to contaminated seawater.
- Both are halophilic (salt-loving), unlike V. cholerae.
| Species | Clinical Features | Notes |
|---|---|---|
| V. parahaemolyticus | Gastroenteritis: Explosive, watery diarrhea; self-limiting. | Most common cause of seafood-associated gastroenteritis in the US. |
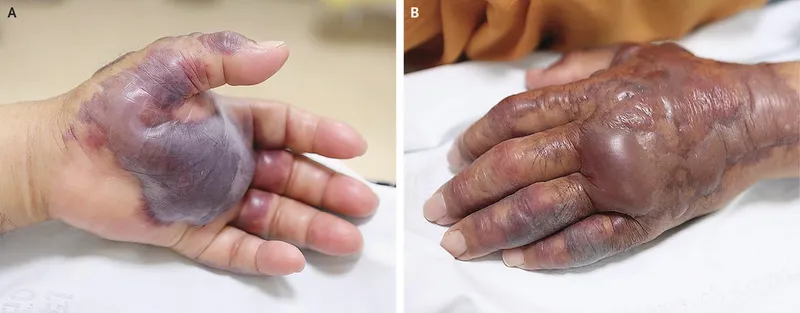
| V. vulnificus | 1. Wound Infections: Rapidly progressive cellulitis, hemorrhagic bullae, necrotizing fasciitis. 2. Septicemia: High fever, shock. | High mortality, especially with underlying liver disease (e.g., cirrhosis, hemochromatosis). |
Diagnosis & Treatment - Taming the Tide
- Specimen: Stool sample for culture; blood culture for septicemia (V. vulnificus).
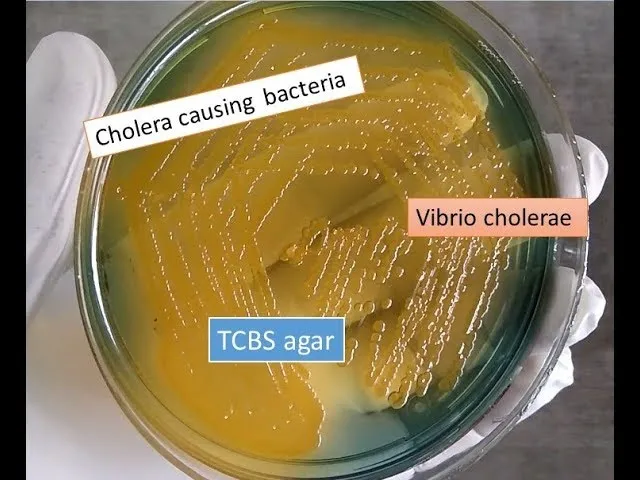
- Culture: Selective Thiosulfate-Citrate-Bile Salts-Sucrose (TCBS) agar is crucial.
- V. cholerae: ferments sucrose → yellow colonies.
- V. parahaemolyticus/vulnificus: non-fermenters → green/blue-green colonies.
- Primary Treatment: Aggressive Rehydration
- Oral Rehydration Salts (ORS) for most cases.
- IV fluids (Ringer's Lactate) for severe dehydration, shock, or altered mental status.
- Antibiotics (adjunctive): Reduce fluid loss & duration.
- Primary: Doxycycline (single dose), Azithromycin.
- Alternative: Ciprofloxacin.
⭐ Prompt fluid and electrolyte replacement is the single most important life-saving intervention in cholera management.
High‑Yield Points - ⚡ Biggest Takeaways
- Vibrio cholerae causes profuse, watery diarrhea (rice-water stool) via the cholera toxin.
- The toxin permanently activates the Gs protein, leading to ↑ cAMP and massive fluid secretion.
- Transmission is fecal-oral, typically through contaminated water or improperly cooked shellfish.
- Grows on TCBS agar (Thiosulfate-Citrate-Bile Salts-Sucrose) and in alkaline media.
- Treatment is aggressive oral or IV rehydration.
- Vibrio vulnificus can cause life-threatening wound infections and sepsis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

