Microbiology & Virulence - The Chocolate-Loving Vampire
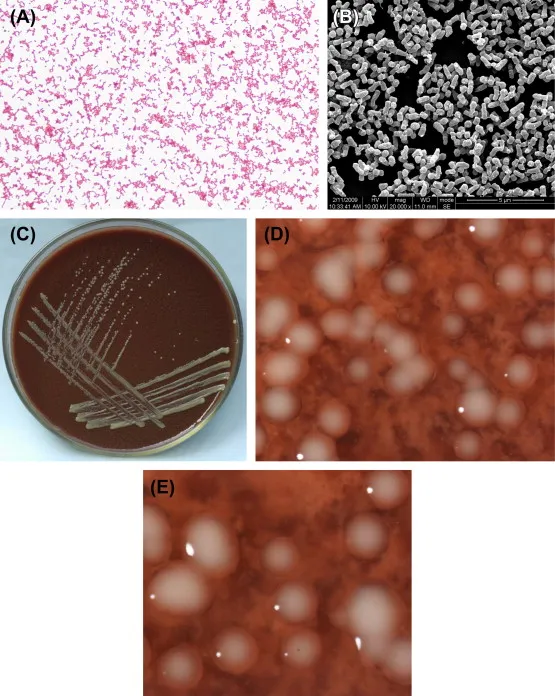
- Gram-negative coccobacillus.
- Pleomorphic: can appear as long filaments, or coccoid.
- Grows on chocolate agar, which contains heat-lysed blood cells.
- 📌 Requires both Factor V (NAD+) and Factor X (hematin) for growth - "The Vampire needs his X and V's".
- Virulence Factors:
- Polysaccharide capsule: Antiphagocytic. Type b (Hib) is the most virulent, containing polyribosylribitol phosphate (PRP).
- IgA protease: Cleaves IgA at mucosal sites, facilitating colonization.
⭐ The Hib conjugate vaccine, which links the PRP capsule to a protein carrier (e.g., tetanus toxoid), has dramatically reduced the incidence of invasive H. influenzae type b diseases like meningitis and epiglottitis.
Clinical Syndromes - From Ear to Everywhere
H. influenzae presents as two main clinical entities: non-typeable (NTHi) strains causing mucosal infections and encapsulated type b (Hib) causing invasive disease.
-
Non-typeable (NTHi) - Local Invasion
- Major cause of otitis media, sinusitis, and conjunctivitis.
- Frequently exacerbates COPD, leading to bronchitis and pneumonia.
-
Encapsulated (Hib) - Systemic Invasion (mainly in unvaccinated children)
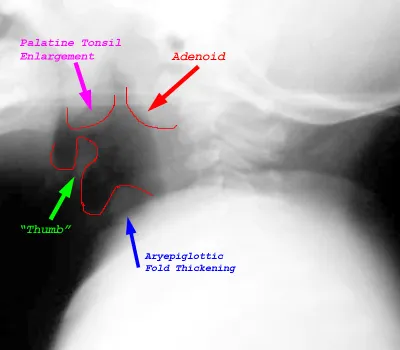
- 📌 EMOP: Epiglottitis, Meningitis, Otitis media, Pneumonia.
- Acute Epiglottitis: Medical emergency! Characterized by dysphagia, drooling, and distress. Cherry-red epiglottis.
- Meningitis: Previously the leading cause in children aged 3 months to 3 years.
- Septic arthritis, Sepsis.
⭐ The Hib conjugate vaccine, given between 2 and 15 months, has dramatically reduced invasive disease. Consequently, NTHi is now the predominant strain causing infections in the US.
Diagnosis - Lab Detective Work
- Specimen: CSF, blood, sputum, or pus.
- Microscopy: Gram-negative coccobacilli or pleomorphic rods.
- Culture: Requires chocolate agar (heated blood) to release factors X (hematin) and V (NAD+).
- 📌 "Satellitism": H. influenzae grows around S. aureus colonies on blood agar, as S. aureus lyses RBCs and provides the necessary V factor.
- Quellung Reaction: For capsular serotyping (e.g., type b); capsule swells with specific antiserum.
⭐ Antigen detection in CSF via latex agglutination is a rapid method for diagnosing H. influenzae meningitis.
Treatment & Prevention - Drugs, Jabs, and Victory
- Systemic Disease (Meningitis, Epiglottitis):
- IV Ceftriaxone is the empirical treatment of choice.
- Mucosal Infections (Otitis Media, Sinusitis):
- Amoxicillin-clavulanate is effective against β-lactamase producing strains.
- Chemoprophylaxis for Close Contacts:
- Rifampin is used to eliminate nasopharyngeal carriage in unvaccinated contacts.
- Vaccination (The Ultimate Victory):
- Hib conjugate vaccine has dramatically ↓ incidence.
- Contains capsular polysaccharide (PRP) conjugated to a carrier protein (e.g., tetanus toxoid).
- Routinely given between 2 and 18 months of age.
⭐ For invasive H. influenzae meningitis, ceftriaxone is the primary antibiotic. Dexamethasone is often co-administered to reduce the risk of neurological sequelae, such as sensorineural hearing loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Gram-negative coccobacillus requiring chocolate agar with growth factors V (NAD+) and X (hematin).
- Causes Meningitis, Epiglottitis, Pneumonia, and Otitis Media, mainly in unvaccinated children.
- The primary virulence factor for invasive disease is the type b (Hib) capsule (a polyribosylribitol phosphate polymer).
- The Hib conjugate vaccine (PRP-protein) has nearly eliminated invasive Hib disease.
- Treat systemic disease with ceftriaxone; use rifampin for prophylaxis in close contacts.
- Non-typeable (unencapsulated) strains commonly cause mucosal infections (otitis, sinusitis).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

