The Anaerobic Crew - Gut Feelings
- Normal flora of the GI tract (colon), oral cavity, and vagina. Predominantly gram-negative rods.
- Obligate anaerobes; lack enzymes like catalase and superoxide dismutase to defend against oxidative stress.
- Pathogenesis: Cause abscesses (intra-abdominal, pelvic, pulmonary) when displaced from normal flora sites (e.g., surgery, trauma). Infections are typically polymicrobial and foul-smelling.
- Bacteroides fragilis: Most common anaerobe causing clinical infection. Its polysaccharide capsule is a key virulence factor.
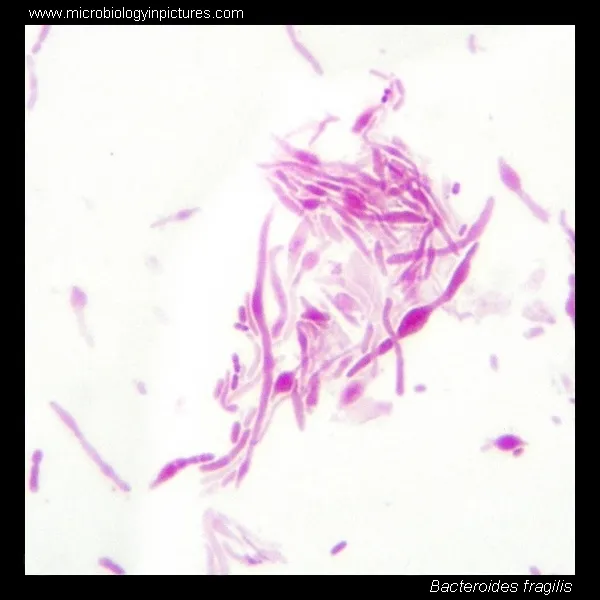
⭐ Bacteroides fragilis produces beta-lactamase, conferring resistance to many penicillins and cephalosporins. It is aerotolerant, allowing it to survive transit to deeper tissues.
Bacteroides fragilis - The Abscess Artist
- Gram-negative obligate anaerobe, a key component of normal colonic flora.
- Most common anaerobe in clinical infections, famed for causing intra-abdominal abscesses.
- Virulence Factors:
- Polysaccharide capsule: Unique zwitterionic structure; antiphagocytic and directly promotes abscess formation.
- Modified Lipopolysaccharide (LPS) with low endotoxin activity, causing less fever and shock.
- Enzymes like heparinase and collagenase facilitate tissue invasion.
📌 Bacteroides = Belly Abscesses.
⭐ High-Yield: The B. fragilis polysaccharide capsule alone is sufficient to induce abscess formation in animal models, even without the whole bacterium.
- Treatment: Requires anaerobic coverage (e.g., metronidazole, piperacillin-tazobactam) AND surgical drainage of the abscess.
Prevotella & Fusobacterium - Beyond the Gut
- Anaerobic, gram-negative rods, primarily colonizing the oral cavity & upper respiratory tract (unlike gut-dominant Bacteroides).
- Prevotella intermedia
- Forms black-pigmented colonies on blood agar.
- Associated with "pregnancy gingivitis," ANUG (Acute Necrotizing Ulcerative Gingivitis), and aspiration pneumonia.
- Fusobacterium nucleatum
- Distinctive spindle-shaped (fusiform) morphology.
- A key component of dental plaque; implicated in periodontal disease and aspiration pneumonia.
⭐ Lemierre's Syndrome: Caused by Fusobacterium necrophorum, this is an infected thrombophlebitis of the internal jugular vein, typically following a sore throat. Leads to septic emboli, often to the lungs.
Treatment Plan - Anaerobe Annihilators
- Primary Strategy: Select antibiotics based on the site of infection, as this predicts the likely pathogens.
- Drug Resistance: Many anaerobes, especially Bacteroides, produce β-lactamases, conferring resistance to penicillins.
- Broad Spectrum Options: For severe or polymicrobial infections, use Piperacillin-Tazobactam or Carbapenems.
- 📌 Mnemonic: Use Clindamycin for Chest infections (above diaphragm); use Metronidazole for Metro/belly infections (below diaphragm).
⭐ Bacteroides fragilis is the most common anaerobe causing intra-abdominal infections and is frequently resistant to penicillin alone due to β-lactamase production. This makes metronidazole a cornerstone of therapy for gut-related anaerobic infections.
- Bacteroides fragilis is the most important clinical anaerobe, dominating the normal colonic flora.
- It is a primary cause of polymicrobial intra-abdominal abscesses, especially post-surgery or trauma.
- The major virulence factor is its polysaccharide capsule, which is sufficient to cause abscesses.
- Frequently produces β-lactamases, making it resistant to penicillins and some cephalosporins.
- Infections are classically associated with foul-smelling discharge due to anaerobic metabolism.
- Key treatments include metronidazole, carbapenems, and piperacillin-tazobactam.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

