Core Indications - The Green Light
-
Patient Selection:
- Good pre-stroke functional status (mRS 0-1).
- Disabling neurological deficit (NIHSS score ≥ 6).
-
Vascular & Parenchymal Imaging:
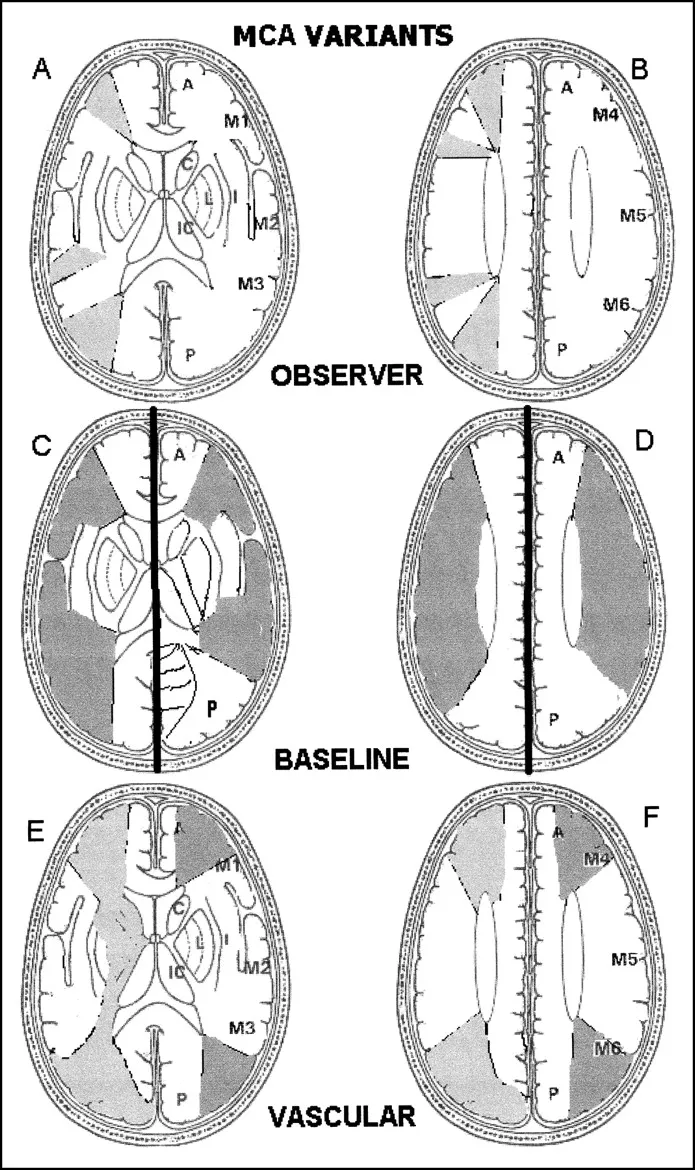
- Confirmed large vessel occlusion (LVO) in the anterior circulation (ICA or MCA M1 segment).
- Small established infarct core, indicating significant salvageable brain tissue (penumbra). A non-contrast CT-based ASPECTS score ≥ 6 is the classic threshold.
-
Time Window:
- Standard window: treatment within 6 hours of symptom onset.
⭐ The DAWN and DEFUSE 3 trials radically extended the window to 24 hours for select patients demonstrating a "clinical-core mismatch" on advanced imaging (e.g., CT perfusion), where a small infarct core contrasts with a severe clinical deficit.
Time Windows & Imaging - Race Against the Clock
-
Core Principle: Identify Large Vessel Occlusion (LVO) and salvageable brain tissue (penumbra).
-
Initial Imaging: Non-contrast CT (to rule out hemorrhage) followed by CT Angiography (CTA) to identify LVO.
-
Early Window (< 6 hours from LKW):
- Criteria: LVO in anterior circulation (ICA, M1) + NIHSS score ≥ 6 + ASPECTS score ≥ 6.
-
Late Window (6-24 hours from LKW):
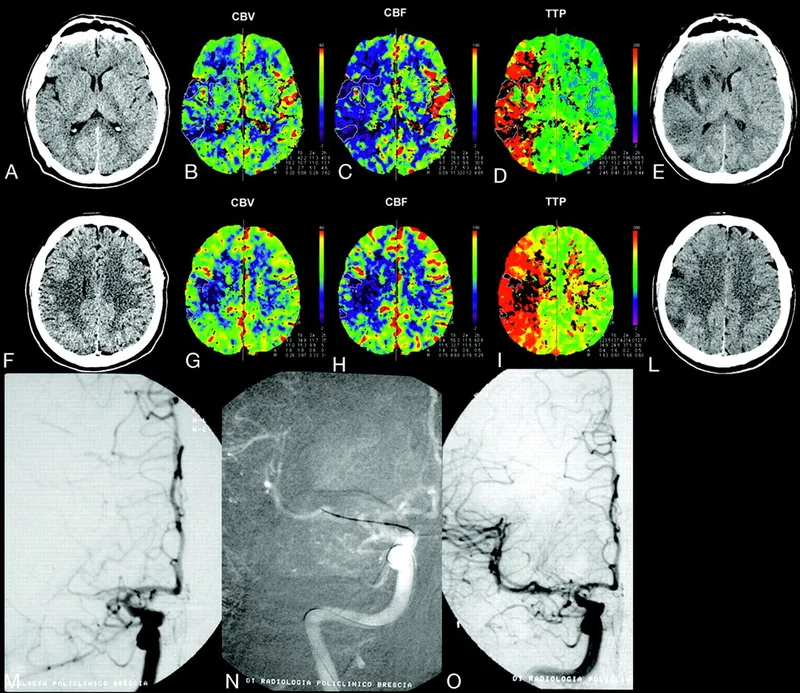
- Requires advanced imaging (CT Perfusion or DWI-MRI) to assess for mismatch.
- Mismatch: Small infarct core, large clinical deficit/penumbra.
- 📌 Mnemonic: DAWN/DEFUSE the time bomb.
⭐ High-Yield: The DAWN trial selected patients with a severe clinical deficit (NIHSS ≥ 10) but a small infarct core on imaging, demonstrating the principle of "tissue window" over "time window."
Key Trials - DAWN & DEFUSE 3
Expanded the mechanical thrombectomy (MT) window beyond 6 hours by prioritizing brain tissue status over strict time cutoffs. Patient selection relies on identifying a mismatch between the clinical deficit or salvageable tissue and the actual infarct size using advanced imaging.
-
DAWN Trial
- Window: 6-24 hours from last known well (LKW).
- Concept: Clinical-Core Mismatch.
- Criteria: High NIHSS score (≥10) despite a small infarct core on imaging. This mismatch implies a large salvageable penumbra.
-
DEFUSE 3 Trial
- Window: 6-16 hours from LKW.
- Concept: Target Mismatch Profile.
- Criteria: Favorable perfusion imaging profile: small infarct core (<70 mL) and a penumbra-to-core volume ratio ≥1.8.
⭐ These trials proved that selecting patients based on salvageable brain tissue ("tissue is brain") is superior to rigid time windows ("time is brain") for late-presenting large vessel occlusion strokes.
High-Yield Points - ⚡ Biggest Takeaways
- Indicated for large vessel occlusion (LVO) in the anterior circulation (e.g., MCA, ICA).
- Standard treatment window is within 6 hours of symptom onset.
- The window can be extended up to 24 hours for select patients based on perfusion imaging (DAWN/DEFUSE-3 criteria).
- Requires a significant neurological deficit, typically an NIHSS score ≥ 6.
- Imaging must show a small infarct core (e.g., ASPECTS > 6).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

