ARF: Definition & Diagnosis - Kidney Crisis Kickstart
- Definition: Abrupt decline in kidney function, leading to the retention of urea and other nitrogenous waste products.
- KDIGO Diagnostic Criteria (1 of 3):
- ↑ SCr by ≥0.3 mg/dL within 48 hours
- ↑ SCr to ≥1.5x baseline within 7 days
- Urine volume <0.5 mL/kg/h for 6 hours
- Initial Workup: BMP, urinalysis with microscopy, and renal ultrasound to rule out post-renal obstruction.
⭐ Fractional excretion of sodium ($FeNa$) is a key test to differentiate pre-renal azotemia ($FeNa$ <1%) from acute tubular necrosis (ATN) ($FeNa$ >2%).
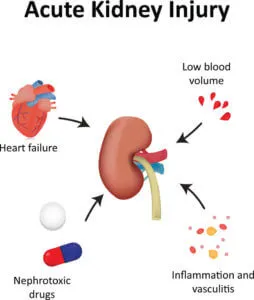
ARF: Etiology - The Usual Suspects
-
Pre-renal (Hypoperfusion)
- Causes: Hypovolemia (hemorrhage, dehydration), ↓ cardiac output (heart failure), sepsis, renal artery stenosis.
- Labs: BUN/Cr > 20:1, FeNa < 1%, concentrated urine (Uosm > 500).
-
Intrinsic (Kidney Damage)
- Acute Tubular Necrosis (ATN): Most common. Ischemic (prolonged pre-renal) or nephrotoxic (contrast, aminoglycosides, myoglobin). muddy brown casts.
- Acute Interstitial Nephritis (AIN): Allergic reaction. 📌 Pee (diuretics), Pain-free (NSAIDs), Penicillins, PPIs, rifamPin. WBC casts, eosinophils.
- Glomerulonephritis: Hematuria, RBC casts.
-
Post-renal (Obstruction)
- Causes: BPH, kidney stones, tumors, neurogenic bladder.
⭐ Fractional Excretion of Sodium (FeNa) is key to differentiate pre-renal from ATN. $FeNa = \frac{(P_{Cr} \times U_{Na})}{(P_{Na} \times U_{Cr})} \times 100$. An FeNa < 1% suggests a pre-renal cause, while > 2% points towards ATN.
ARF: Workup & Management - Fixing the Filters
- Initial Steps: Discontinue nephrotoxic agents (e.g., NSAIDs, ACE-I). Assess and optimize volume status. Rule out and relieve any urinary obstruction.
- Monitoring: Track vital signs, strict I/O, daily weights, and serial chemistry panels (BUN, Cr, K+).
⭐ In oliguric patients, a Fractional Excretion of Sodium ($F_eNa$) <1% strongly suggests a pre-renal state, whereas a $F_eNa$ >2% points towards Acute Tubular Necrosis (ATN). Note: recent diuretic use can render $F_eNa$ unreliable.
ARF: Dialysis Indications - The AEIOU Exits
📌 AEIOU mnemonic for emergent dialysis:
- Acidosis: Severe metabolic acidosis (pH < 7.1)
- Electrolytes: Refractory hyperkalemia (K⁺ > 6.5 mEq/L) or symptomatic changes
- Ingestions: Toxic alcohols (methanol, ethylene glycol), salicylates, lithium
- Overload: Refractory volume overload (e.g., pulmonary edema)
- Uremia: Symptomatic (encephalopathy, pericarditis, bleeding)
⭐ Uremic pericarditis is an absolute indication for dialysis, regardless of BUN/creatinine levels. It may not show classic diffuse ST elevation on ECG.

High-Yield Points - ⚡ Biggest Takeaways
- Prerenal azotemia, the most common cause of AKI, typically responds to IV fluids.
- Differentiate prerenal from ATN using a BUN/Cr ratio >20 and FeNa <1%.
- For postrenal failure, the priority is to relieve the obstruction, often with a Foley catheter.
- Immediately discontinue all nephrotoxic agents (e.g., NSAIDs, ACE inhibitors, contrast).
- Treat severe hyperkalemia emergently with calcium gluconate, followed by insulin/glucose.
- Indications for urgent dialysis follow the AEIOU mnemonic: Acidosis, Electrolytes, Ingestions, Overload, Uremia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

