Etiology & Pathophysiology - The Broken Factory
- Primary Causes:
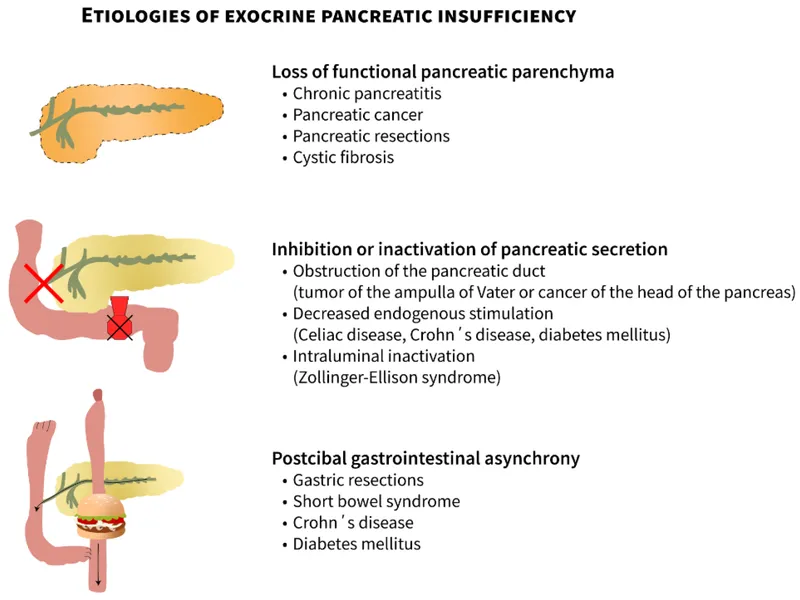
- Adults: Chronic pancreatitis (most common), pancreatic surgery, ductal obstruction (e.g., neoplasm).
- Children: Cystic fibrosis (most common), Shwachman-Diamond syndrome.
- Pathophysiology: Progressive loss of acinar cells impairs digestive enzyme production. Fat and protein digestion are most affected due to reduced lipase and protease secretion.
⭐ Clinical symptoms of malabsorption, particularly steatorrhea, do not manifest until >90% of the pancreas's exocrine function is lost.
Clinical Features - The Greasy Truth
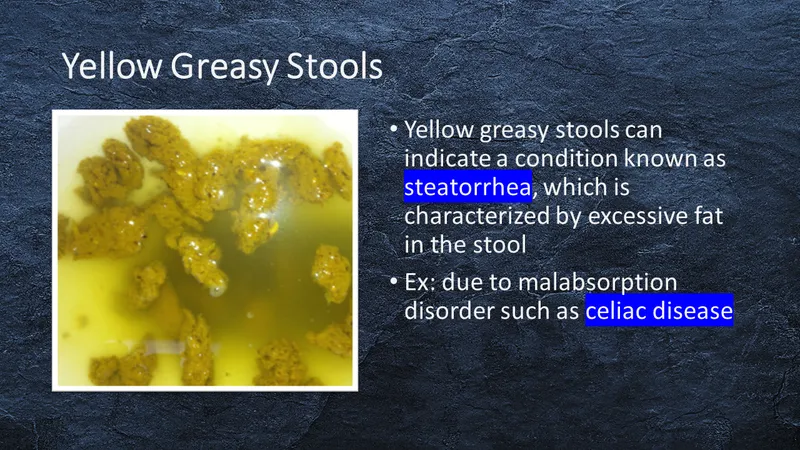
- Steatorrhea: The hallmark symptom. Stools are greasy, foul-smelling, voluminous, and difficult to flush due to fat malabsorption (fecal fat >7 g/day).
- Weight Loss & Malnutrition: Occurs despite a normal or even increased appetite (polyphagia).
- Abdominal Discomfort: Bloating, cramping, and excessive flatulence are common.
- Fat-Soluble Vitamin Deficiency:
- A: Night blindness
- D: Bone pain, fractures (osteomalacia/osteoporosis)
- E: Neuropathy, ataxia
- K: Easy bruising, bleeding (↑ PT/INR)
⭐ Symptoms of malabsorption typically do not manifest until over 90% of the pancreas's exocrine function is lost. Chronic pancreatitis is the leading cause in adults.
Diagnosis - Catching the Culprit
- Indirect Pancreatic Function Tests (PFTs):
- Fecal Elastase-1 (FE-1): Test of choice. Not affected by pancreatic enzyme replacement therapy (PERT).
- Result < 200 µg/g confirms diagnosis.
- 72-hour Fecal Fat: Gold standard but cumbersome. Measures steatorrhea (> 7 g/day).
- Serum Trypsinogen: Low levels (< 20 ng/mL) suggest severe EPI.
- Fecal Elastase-1 (FE-1): Test of choice. Not affected by pancreatic enzyme replacement therapy (PERT).
- Direct PFTs:
- Secretin/CCK Stimulation Test: Most sensitive & specific. Invasive (endoscopic), reserved for equivocal cases. Measures bicarbonate and enzyme output.
⭐ Fecal elastase-1 is the preferred initial test for EPI. Its measurement is not affected by concurrent pancreatic enzyme replacement therapy (PERT), unlike other fecal tests.
Management - Restoring the Flow
- Pancreatic Enzyme Replacement Therapy (PERT) is the cornerstone.
- Contains lipase, amylase, and protease.
- Dosing is based on lipase component: start 500-2,500 lipase units/kg per meal.
- Administer with the first bite of meals and snacks; do not crush or chew capsules.
- Adjunctive Acid Suppression
- PPIs or H2 blockers may be added to prevent the gastric acid degradation of lipase.
- Dietary & Lifestyle Modification
- Small, frequent, moderate-fat meals.
- Supplement fat-soluble vitamins (A, D, E, K) as needed.
- Strict alcohol cessation.
⭐ The primary goal of PERT is not just to resolve steatorrhea, but to reverse the nutritional deficiencies, especially of fat-soluble vitamins.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic pancreatitis is the most common cause of EPI in adults; cystic fibrosis is the primary cause in children.
- Classic presentation includes steatorrhea (greasy, foul-smelling stools), weight loss, and deficiency of fat-soluble vitamins (A, D, E, K).
- Fecal elastase-1 is the most sensitive and specific non-invasive diagnostic test; a level <200 µg/g is confirmatory.
- Management is centered on pancreatic enzyme replacement therapy (PERT), administered with all meals and snacks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

