The Vulnerable Host - Setting the Stage
- Immunocompromised State: A condition of defective host immunity, predisposing to opportunistic infections (OIs). Key causes include:
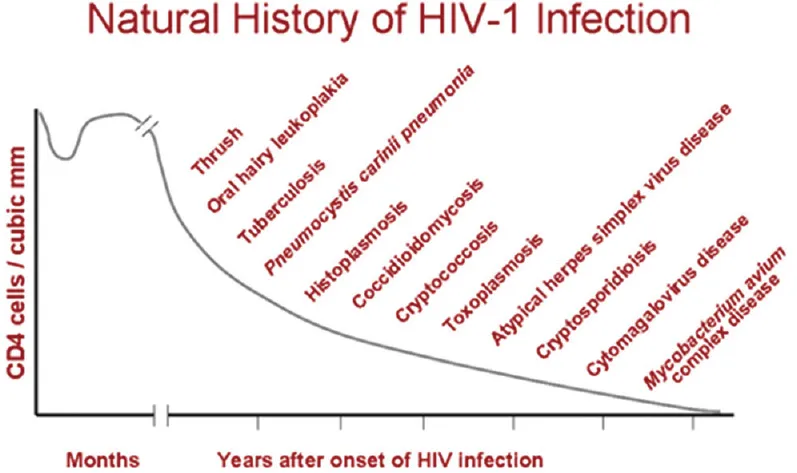
- HIV/AIDS: Defined by a CD4+ T-cell count < 200 cells/µL. Risk of specific OIs correlates with progressively lower CD4 counts.
- Neutropenia: Severe risk at Absolute Neutrophil Count (ANC) < 500/µL. Calculated as $ANC = \text{WBC} \times (% \text{Segs} + % \text{Bands})$.
- Solid Organ/Stem Cell Transplant: Due to potent immunosuppressive therapy (e.g., calcineurin inhibitors, anti-proliferatives).
- Chronic Glucocorticoids: Prednisone dose ≥ 20 mg/day for ≥ 2 weeks impairs cell-mediated immunity.
⭐ Neutropenic Fever (T > 38.3°C & ANC < 500/µL) is a medical emergency requiring immediate broad-spectrum antibiotics after blood cultures are drawn.
Fungal Foes - Spores on Tour
- Pneumocystis jirovecii (PCP)
- Presentation: Hypoxia, non-productive cough, fever.
- Diagnosis: CXR with diffuse bilateral ground-glass opacities. Bronchoalveolar lavage (BAL) with silver stain.
- Treatment: TMP-SMX.
- Candida albicans
- Presentation: Esophagitis (painful swallowing), oral thrush, vaginitis.
- Diagnosis: Endoscopy with biopsy shows yeast and pseudohyphae.
- Treatment: Fluconazole.
- Aspergillus fumigatus
- Presentation: Allergic bronchopulmonary aspergillosis (ABPA), aspergilloma in cavities, invasive disease.
- Diagnosis: Galactomannan assay. CT shows "halo" or "air-crescent" sign.
- Treatment: Voriconazole.
- Cryptococcus neoformans
- Presentation: Meningoencephalitis in HIV/AIDS.
- Diagnosis: India ink stain of CSF shows encapsulated yeast. Cryptococcal antigen test.
- Treatment: Amphotericin B + Flucytosine, then Fluconazole.
⭐ Prophylaxis for Pneumocystis pneumonia (PCP) with TMP-SMX is initiated when CD4+ count drops below 200 cells/μL.
Viral & Protozoan Villains - Intracellular Invaders
| Pathogen | Key System & Findings | Diagnosis | Treatment |
|---|---|---|---|
| CMV | Retina: "Pizza-pie" retinitis. CD4 < 50. | Fundoscopy, PCR | Ganciclovir, Foscarnet |
| Toxoplasma | Brain: Multiple ring-enhancing lesions. | Serology, MRI | Pyrimethamine + Sulfadiazine |
| JC Virus (PML) | Brain: Non-enhancing white matter lesions. | MRI, CSF PCR | Supportive, ART |
| Cryptosporidium | Gut: Chronic, watery diarrhea. | Stool acid-fast stain | Nitazoxanide, rehydration |
⭐ In HIV patients with ring-enhancing brain lesions, empiric treatment for Toxoplasmosis is initiated. If lesions do not improve, consider primary CNS lymphoma (EBV-associated) and proceed with a brain biopsy.
Prophylaxis Playbook - Defensive Strategy
- Nocardia: Prophylaxis with TMP-SMX for high-risk patients (e.g., transplant, chronic steroids).
- Mycobacterium avium complex (MAC): Azithromycin weekly if CD4 < 50 & not on ART.
⭐ Discontinuation Criteria: Prophylaxis can often be stopped when CD4 count rises > 200 for > 3 months on ART.
High‑Yield Points - ⚡ Biggest Takeaways
- CD4 count dictates prophylaxis for opportunistic infections in HIV.
- Start PJP prophylaxis (TMP-SMX) at CD4 < 200.
- Add Toxoplasmosis prophylaxis (TMP-SMX) at CD4 < 100 if IgG positive.
- Begin MAC prophylaxis (Azithromycin) when CD4 count is < 50.
- CMV retinitis ("pizza-pie" fundoscopy) occurs at CD4 < 50; treat with ganciclovir.
- Suspect Cryptococcal meningitis with fever/headache; diagnose with CSF cryptococcal antigen.
- PML (JC virus) presents with non-enhancing white matter lesions on brain MRI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

